Abdominal and Pelvic Radiology — MCQs

On this page
A 30-year-old female presents with sterile pyuria. The radiograph below is provided. What is the most likely diagnosis?
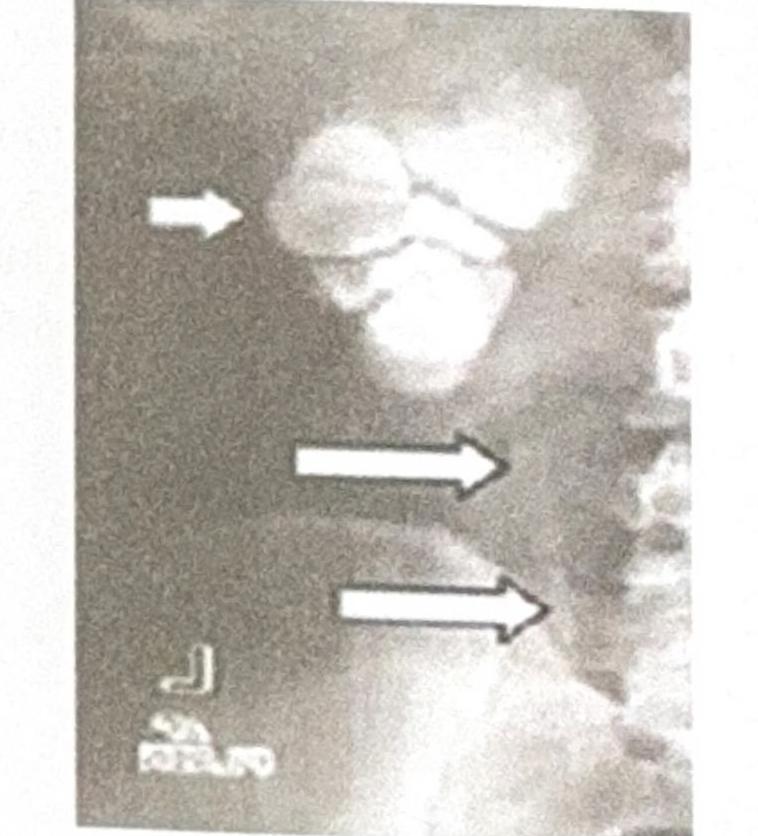
A patient presents with abdominal distension. Based on the X-ray, which of the following bowel loops are dilated?
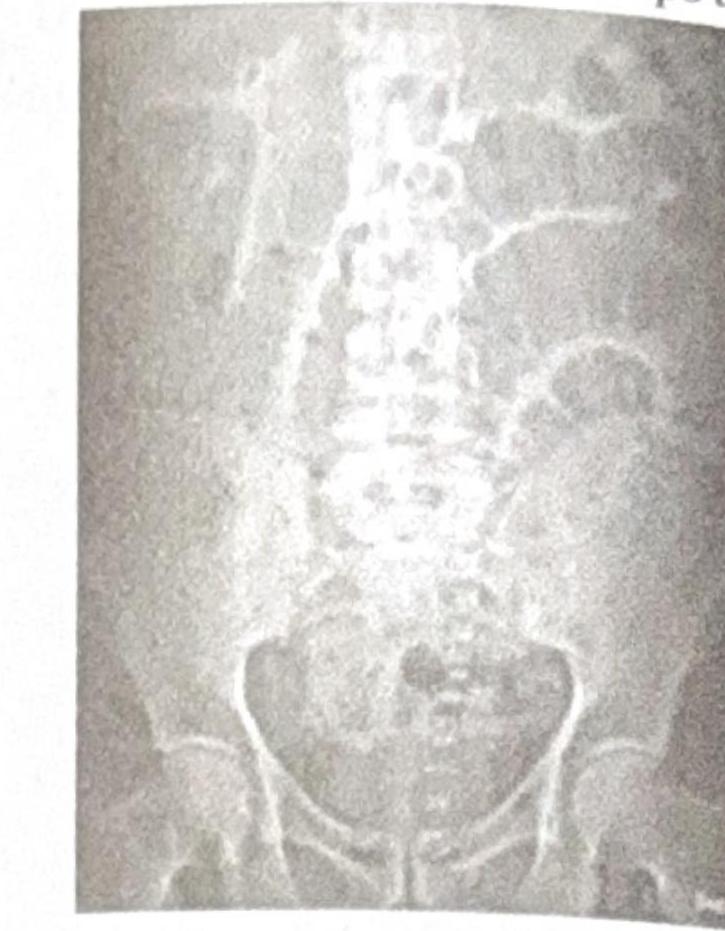
Identify the condition based on the non-contrast CT scan of a patient given below.
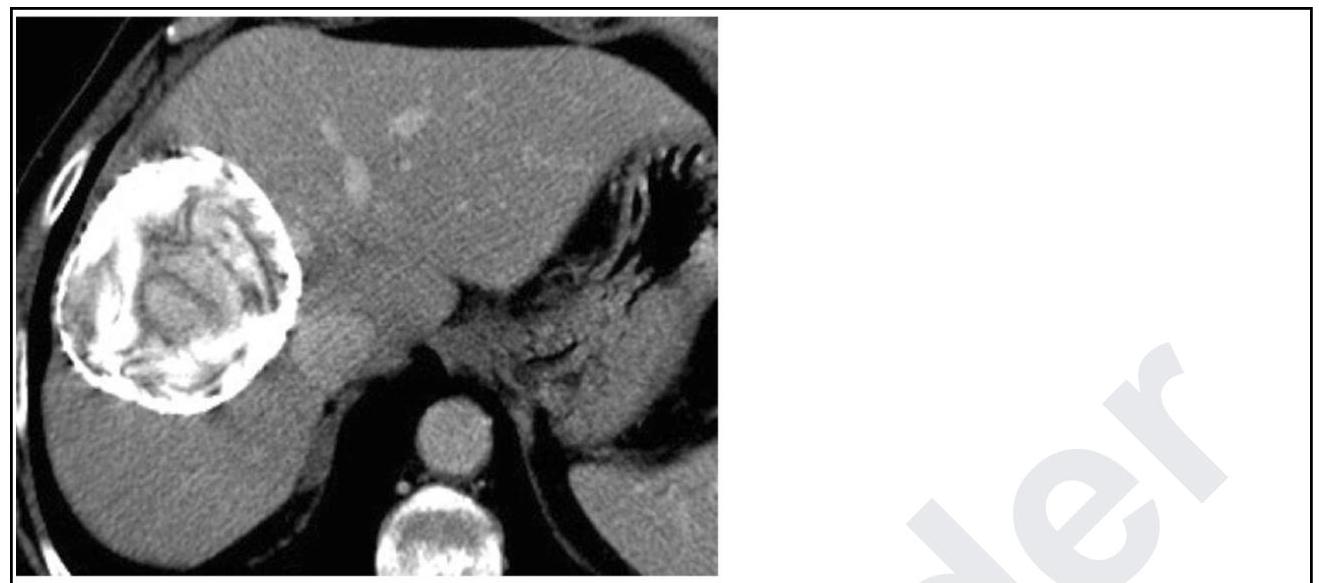
A 45-year-old patient presented with vague abdominal pain. On USG, he was found to have a renal cyst of Bosniak class III. CECT was done, as shown below. What imaging modality is shown?
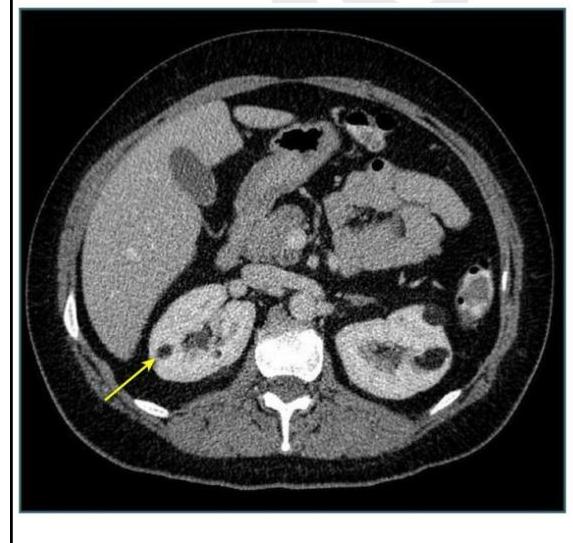
One of the following is characterised by RIM sign?
The best investigation for air in the peritoneal cavity is:
In which of the following conditions is the lead pipe appearance of the colon seen on a barium enema?
In which of the following conditions is air under both sides of diaphragm visualized -
Gas absent from intestine (gasless abdomen) on x-ray is seen in which condition?
What is the characteristic feature of hepatocellular carcinoma on triphasic CT?
Practice by Chapter
Imaging of Liver
Practice Questions
Biliary Tract Imaging
Practice Questions
Pancreatic Imaging
Practice Questions
Spleen and Lymphatic System
Practice Questions
Gastrointestinal Tract Imaging
Practice Questions
Renal and Urinary Tract Imaging
Practice Questions
Adrenal Imaging
Practice Questions
Female Pelvic Imaging
Practice Questions
Male Pelvic Imaging
Practice Questions
Abdominal Trauma Imaging
Practice Questions
Acute Abdomen Imaging
Practice Questions
Imaging of Peritoneal Cavity and Retroperitoneum
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
