Renal Pathology — MCQs

On this page
What is the condition characterized by the triad of glomerulonephritis, pulmonary hemorrhages, and the presence of antibody to the basement membrane?
What is the most common malignant tumor of the kidney in children?
Polycystic kidney disease is most commonly inherited in which pattern?
Which type of Focal Segmental Glomerulosclerosis (FSGS) has the worst prognosis?
In Wegener's granulomatosis, what are the characteristic histopathological features seen in the glomeruli?
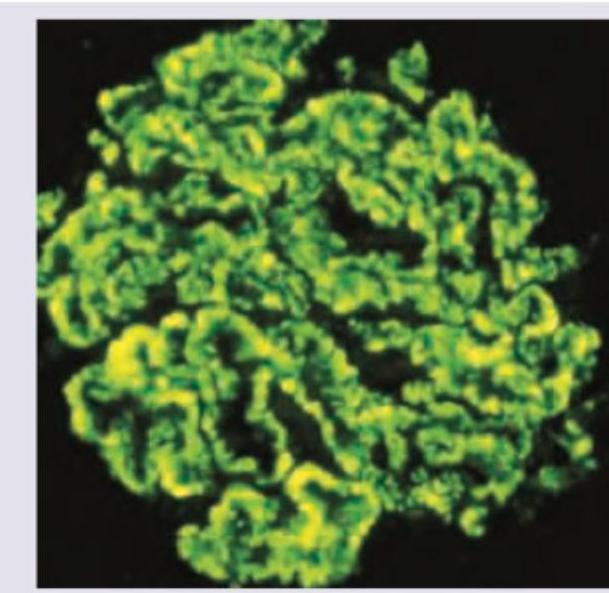
Which is usually a presentation of the condition shown in the immunofluorescence study of the kidney?
Birefringent crystals in urine are seen with which of the following?
Renal biopsy demonstrates concentric, laminated thickening of arteriolar walls due to proliferation of smooth muscle cells. This process is best described by which of the following terms?
Which of the following is the characteristic histological feature of HIV-associated collapsing glomerulopathy?
A patient presents with one normal kidney and the contralateral kidney appearing contracted with evidence of scarring. What is the most probable diagnosis?
Practice by Chapter
Congenital Anomalies of the Kidney
Practice Questions
Glomerular Diseases
Practice Questions
Tubular and Interstitial Diseases
Practice Questions
Vascular Diseases of the Kidney
Practice Questions
Cystic Diseases of the Kidney
Practice Questions
Urinary Tract Obstruction and Stones
Practice Questions
Renal Tumors
Practice Questions
Kidney in Systemic Diseases
Practice Questions
Renal Transplantation Pathology
Practice Questions
Urinary Tract Infections
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
