Renal Pathology — MCQs

On this page
Organized glomerular deposits are present in which of the following conditions?
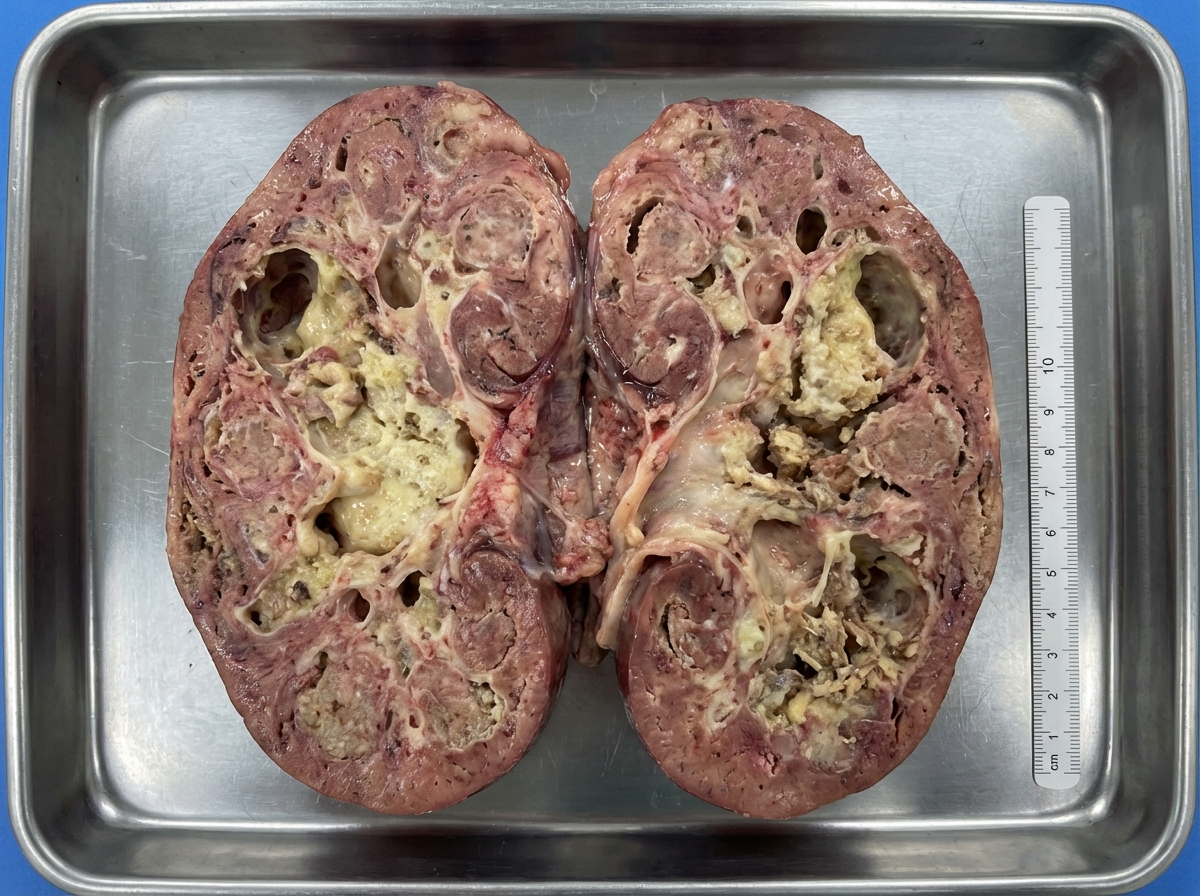
A patient presented with pus in urine. Urine culture was negative. Following a sudden onset of renal failure, the patient died. An autopsy revealed the following finding in the kidney. What is the most likely diagnosis?
Which of the following is NOT a feature of acute diffuse proliferative glomerulonephritis?
What is the most common malignant tumor of the kidney?
Which one of the following variants of renal cell carcinoma has the worst prognosis?
Renal calculi are commonly made up of which substance?
The prognosis is best in rapidly progressive (crescentic) glomerulonephritis associated with which of the following conditions?
Dysmorphic RBCs with acute renal failure (ARF) are typically seen in which condition?
Post-streptococcal glomerulonephritis (PSGN) is associated with which of the following findings?
A patient presents with hematuria of several days and dysmorphic RBC casts in urine. What is the most likely site of origin for these findings?
Practice by Chapter
Congenital Anomalies of the Kidney
Practice Questions
Glomerular Diseases
Practice Questions
Tubular and Interstitial Diseases
Practice Questions
Vascular Diseases of the Kidney
Practice Questions
Cystic Diseases of the Kidney
Practice Questions
Urinary Tract Obstruction and Stones
Practice Questions
Renal Tumors
Practice Questions
Kidney in Systemic Diseases
Practice Questions
Renal Transplantation Pathology
Practice Questions
Urinary Tract Infections
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
