Renal Pathology — MCQs

On this page
A 45-year-old man presents with hematuria. Renal biopsy demonstrates a focal necrotizing glomerulitis with crescent formation. The patient has a history of intermittent hemoptysis and intermittent chest pain of moderate intensity. A previous chest x-ray had demonstrated multiple opacities, some of which were cavitated. The patient also has chronic cold-like nasal symptoms. Which of the following is the most likely diagnosis?
Which of the following statements about Xanthogranulomatous pyelonephritis is not true?
Which of the following is a characteristic histological finding in Alport syndrome?
The important light microscopical features in Alport syndrome are all, EXCEPT:
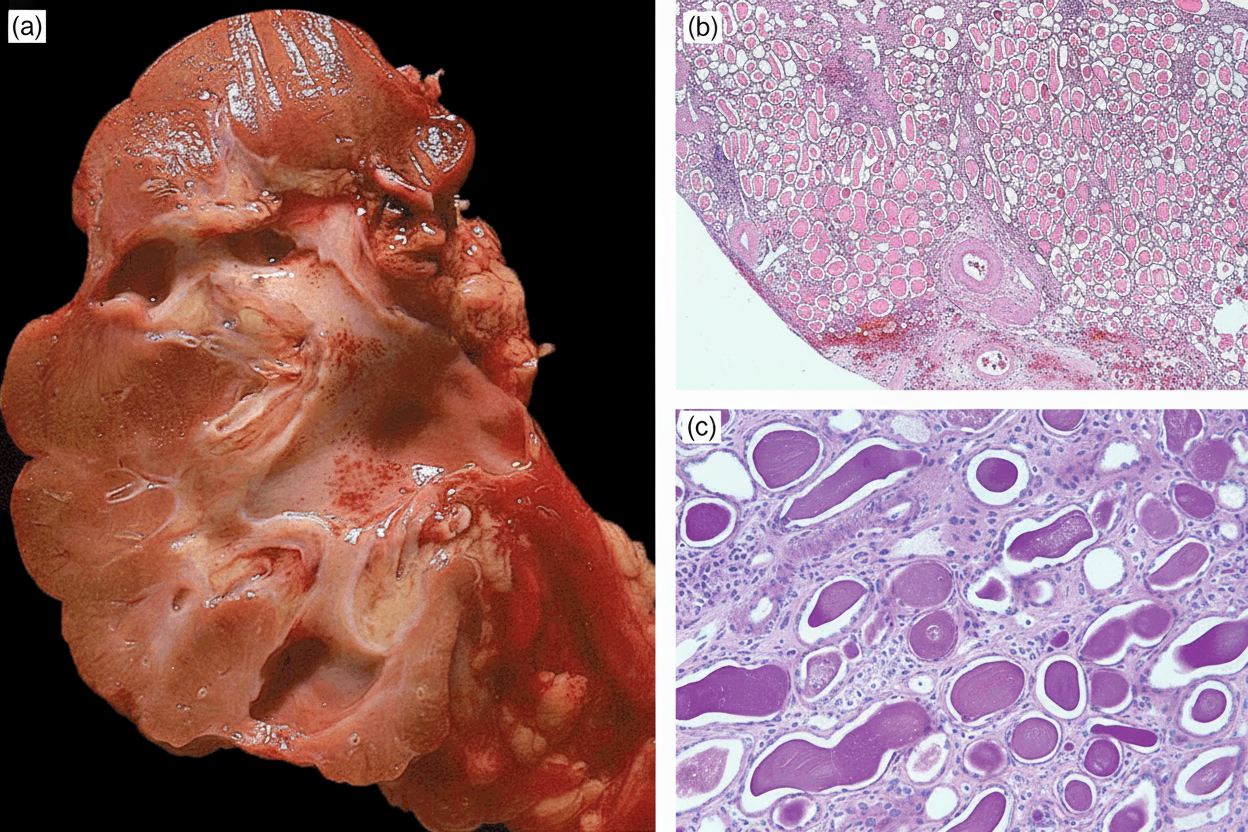
A 45-year-old male with a history of recurrent ureteric calculi presented with fever. Following right-sided nephrectomy, gross and histological views were obtained. What is your diagnosis?
Which condition is characterized by effacement of the foot processes of the podocytes?
Post-streptococcal glomerulonephritis (PSGN) is associated with which of the following?
Post-infective glomerulonephritis typically presents as:
SUPAR is a blood marker for which of the following conditions?
Which protein defect causes Finnish nephrotic syndrome?
Practice by Chapter
Congenital Anomalies of the Kidney
Practice Questions
Glomerular Diseases
Practice Questions
Tubular and Interstitial Diseases
Practice Questions
Vascular Diseases of the Kidney
Practice Questions
Cystic Diseases of the Kidney
Practice Questions
Urinary Tract Obstruction and Stones
Practice Questions
Renal Tumors
Practice Questions
Kidney in Systemic Diseases
Practice Questions
Renal Transplantation Pathology
Practice Questions
Urinary Tract Infections
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
