Renal Pathology — MCQs

On this page
What is the diagnosis for pulmonary hypoplasia associated with uropathy?
Distal and collecting duct cysts are seen in which condition?
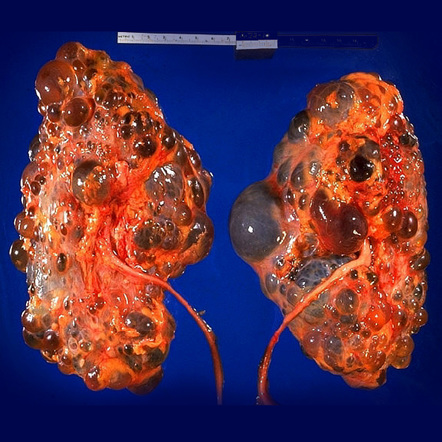
Which of the following is NOT true about the condition shown?
What is the characteristic pathological finding in the kidney in malignant hypertension?
What is the most common viral infection in the kidney?
The characteristic feature of benign nephrosclerosis is
Papillary necrosis is seen in all the following conditions except:
Diabetic glomerulosclerosis is characterized by all of the following EXCEPT:
Which of the following is NOT a typical electron microscopic feature of Alport syndrome?
Which glomerular lesion is seen in cases of reflux nephropathy?
Practice by Chapter
Congenital Anomalies of the Kidney
Practice Questions
Glomerular Diseases
Practice Questions
Tubular and Interstitial Diseases
Practice Questions
Vascular Diseases of the Kidney
Practice Questions
Cystic Diseases of the Kidney
Practice Questions
Urinary Tract Obstruction and Stones
Practice Questions
Renal Tumors
Practice Questions
Kidney in Systemic Diseases
Practice Questions
Renal Transplantation Pathology
Practice Questions
Urinary Tract Infections
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
