Renal Pathology — MCQs

On this page
A 49-year-old male who is a long-term smoker presents with frequency and hematuria. Histologic examination of sections taken from an exophytic lesion of the urinary bladder reveals groups of atypical cells with frequent mitoses forming finger-like projections that have thin, fibrovascular cores. These groups of atypical cells do not extend into the lamina propria and muscularis. No glands or keratin production are found. What is the most accurate diagnosis for this bladder tumor?
A 2 kg baby, born at 30 weeks gestation to an 18-year-old primigravida, died after 48 hours. The Apgar scores were 5 and 8 at 1 and 5 minutes, respectively. Autopsy revealed bilateral enlarged kidneys with multiple radially arranged cysts. Which of the following findings is expected to be associated with this condition?
All are true about infantile polycystic kidney disease except?
Immune complex-mediated glomerular damage is seen in all of the following except:
Which subtype of Renal Cell Carcinoma (RCC) has the best prognosis?
Casts are produced due to damage to which of the following structures?
What is the first manifestation of Alport syndrome?
Which of the following is NOT associated with Adult Polycystic Kidney Disease?
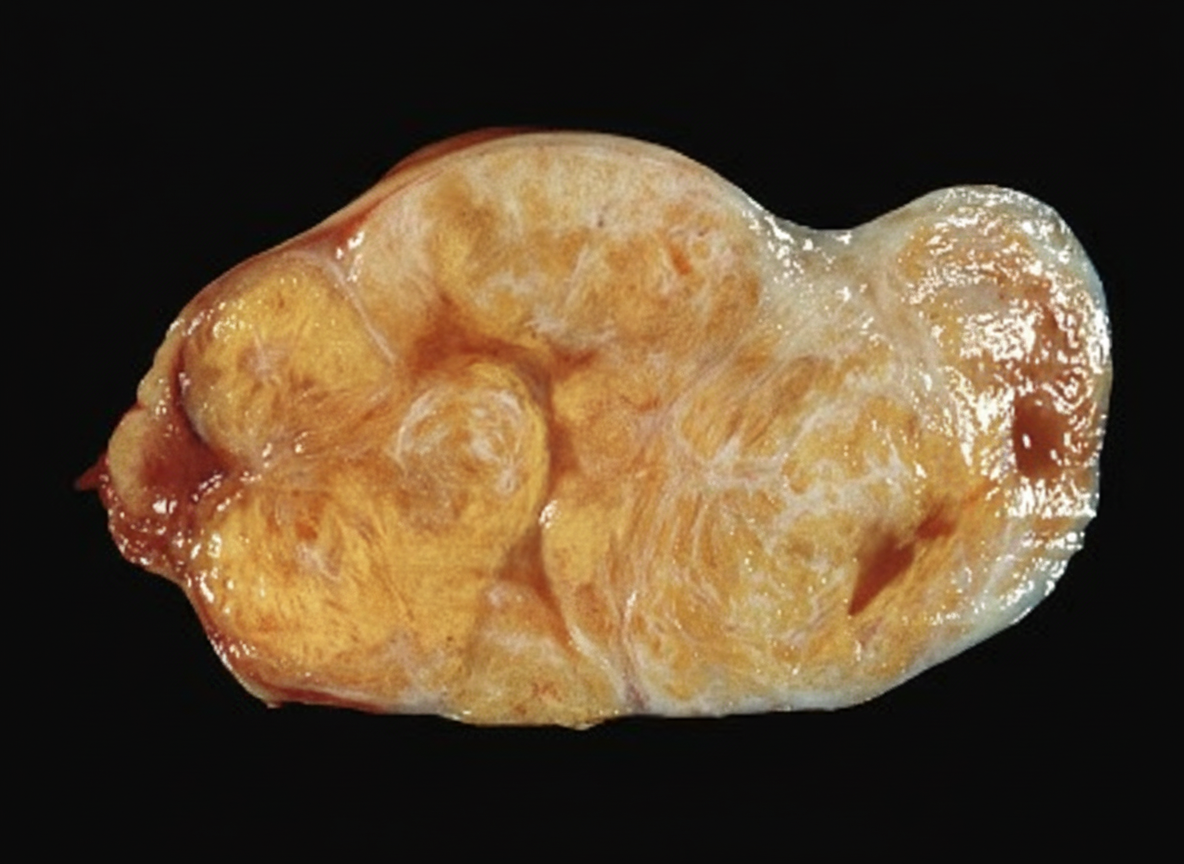
A specimen shows a nephrectomy. What is your diagnosis?
Which is the most characteristic glomerular nephritis (GN) in HIV patients?
Practice by Chapter
Congenital Anomalies of the Kidney
Practice Questions
Glomerular Diseases
Practice Questions
Tubular and Interstitial Diseases
Practice Questions
Vascular Diseases of the Kidney
Practice Questions
Cystic Diseases of the Kidney
Practice Questions
Urinary Tract Obstruction and Stones
Practice Questions
Renal Tumors
Practice Questions
Kidney in Systemic Diseases
Practice Questions
Renal Transplantation Pathology
Practice Questions
Urinary Tract Infections
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
