Renal Pathology — MCQs

On this page
Most common mutation in Alport syndrome is in COL4A5, which is transmitted as?
Alport syndrome is due to defective-
Which of the following conditions is characterized by Type III Rapidly Progressive Glomerulonephritis (RPGN)?
What is the most common lesion in diabetic nephropathy?
A 37-year-old man develops pulmonary hemorrhage and glomerulonephritis. Lung biopsy with immunofluorescence demonstrates IgG deposition along the basement membrane. These antibodies are most likely directed against which of the following types of collagen?
Hemodialysis-associated amyloid is deposited in which of the following?
Which of the following conditions is characterized by highly selective proteinuria?
Immune complex-mediated glomerular damage is seen in all except?
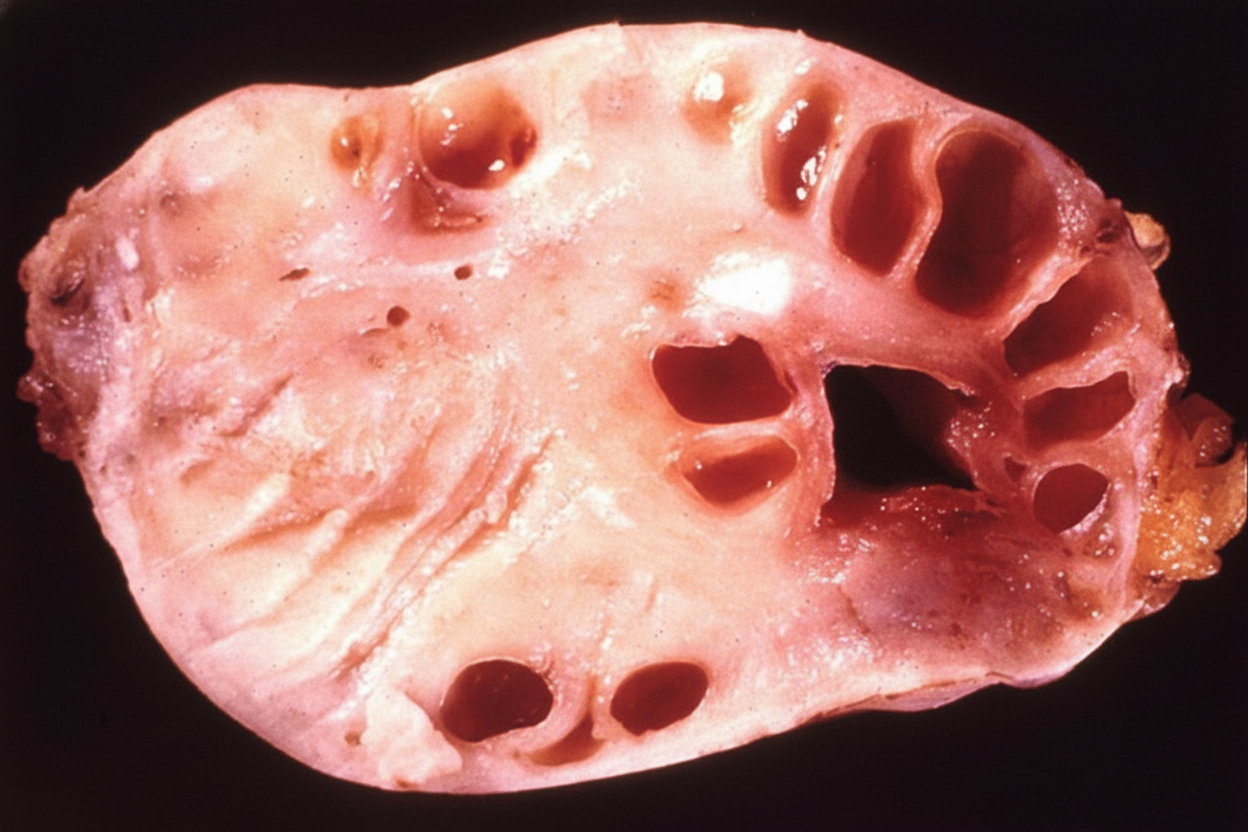
The gross specimen section of kidney depicts which of the following?
Complement level is reduced in which of the following conditions?
Practice by Chapter
Congenital Anomalies of the Kidney
Practice Questions
Glomerular Diseases
Practice Questions
Tubular and Interstitial Diseases
Practice Questions
Vascular Diseases of the Kidney
Practice Questions
Cystic Diseases of the Kidney
Practice Questions
Urinary Tract Obstruction and Stones
Practice Questions
Renal Tumors
Practice Questions
Kidney in Systemic Diseases
Practice Questions
Renal Transplantation Pathology
Practice Questions
Urinary Tract Infections
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
