Renal Pathology — MCQs

On this page
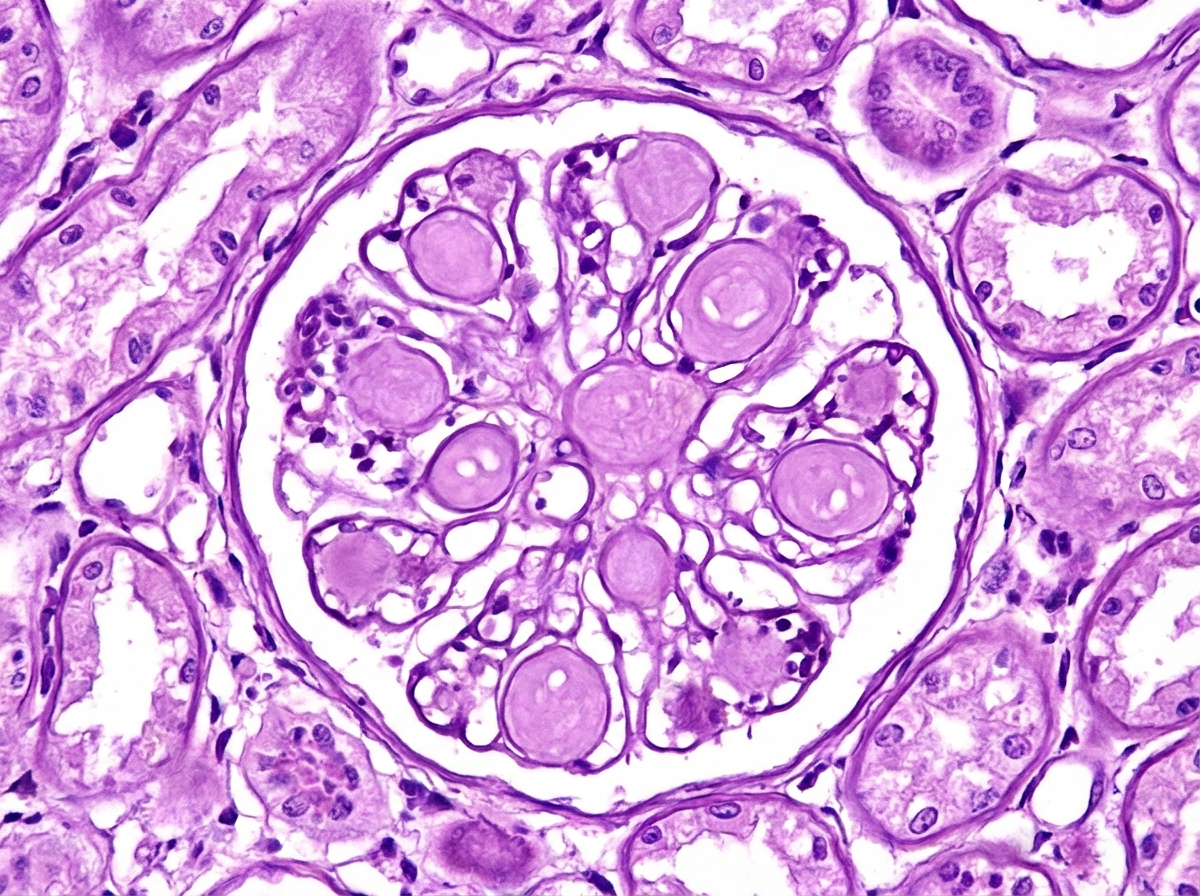
A 50-year-old male presented with blurring of vision. Urine examination showed proteinuria. Fundus examination showed dot-and-blot hemorrhages, microaneurysms, and cotton wool spots. What is the most probable diagnosis based on the provided histopathology?
Which of the following conditions can cause Rapidly Progressive Glomerulonephritis (RPGN)?
Anti-GBM antibodies are characteristically seen in which of the following conditions?
Hemolytic uremic syndrome is characterized by which of the following?
Necrotizing papillitis is seen in all of the following conditions except?
An elderly male patient presented with blurring of vision. Fundus examination revealed cotton wool spots on retina and systemic examination showed decreased peripheral sensations and increased urine output. What finding is shown on renal biopsy?
Which of the following shows crescent-shaped deposits under light microscopy?
Renal pathology in SLE includes all EXCEPT?
What is the most common gene associated with renal cell carcinoma?
Which of the following is NOT a characteristic of acute humoral renal transplant rejection?
Practice by Chapter
Congenital Anomalies of the Kidney
Practice Questions
Glomerular Diseases
Practice Questions
Tubular and Interstitial Diseases
Practice Questions
Vascular Diseases of the Kidney
Practice Questions
Cystic Diseases of the Kidney
Practice Questions
Urinary Tract Obstruction and Stones
Practice Questions
Renal Tumors
Practice Questions
Kidney in Systemic Diseases
Practice Questions
Renal Transplantation Pathology
Practice Questions
Urinary Tract Infections
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
