Renal Pathology — MCQs

On this page
A mutation in the alpha 5 chain of collagen 4 leads to which diagnosis?
Nephrotic syndrome is characterized by
In an adult, unilateral smooth contracted kidney with hypertension is seen in which condition?
What is true about Minimal change disease?
All are features of hemolytic uremic syndrome, EXCEPT?
Which of the following is a characteristic feature of collapsing glomerulopathy?
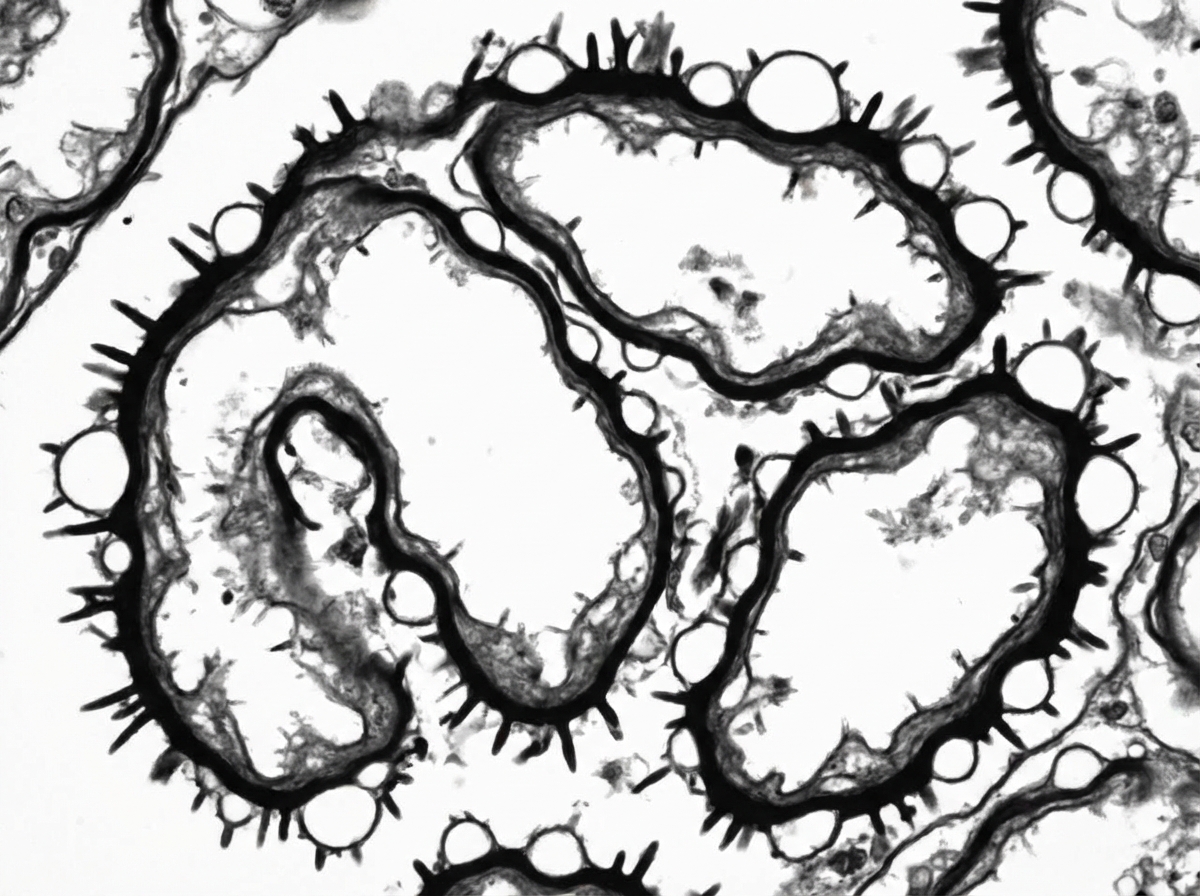
On electron microscopy, what characteristic splitting of the glomerular basement membrane (GBM) with subepithelial deposits is seen in most cases?
A 28-year-old man presents with a large amount of blood and protein in his urine. He has had sensorineural hearing loss since his teen years and anterior lenticonus. The physician suspects a genetic disorder that may lead to eventual kidney failure. If this is the case, the patient most likely has a mutation in which one of the following proteins?
Silver stain performed on renal biopsy shows characteristic findings. Immunostaining for Anti-PLA2R is positive. Based on the given findings, what is the likely diagnosis?
Dysmorphic RBCs are seen in which of the following conditions?
Practice by Chapter
Congenital Anomalies of the Kidney
Practice Questions
Glomerular Diseases
Practice Questions
Tubular and Interstitial Diseases
Practice Questions
Vascular Diseases of the Kidney
Practice Questions
Cystic Diseases of the Kidney
Practice Questions
Urinary Tract Obstruction and Stones
Practice Questions
Renal Tumors
Practice Questions
Kidney in Systemic Diseases
Practice Questions
Renal Transplantation Pathology
Practice Questions
Urinary Tract Infections
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
