Neuropathology — MCQs

On this page
Which one of the following brain tumors is highly vascular in nature?
All of the following are true regarding primary CNS lymphoma, except:
Multiple cystic lesions are seen in the muscle and brain of a 16-year-old boy who died of status epilepticus. What is the most likely diagnosis?
Lewy bodies contain which of the following?
Aggregates of 'tau protein' seen in the Hippocampus of an elderly man are indicative of which of the following?
Which of the following tumors is associated with drop metastasis?
Foix-Alajouanine disease of the spinal cord is a:
Which of the following statements about metastases of malignant tumors of the brain is TRUE?
Which among the following is the commonest type of intracranial tumour?
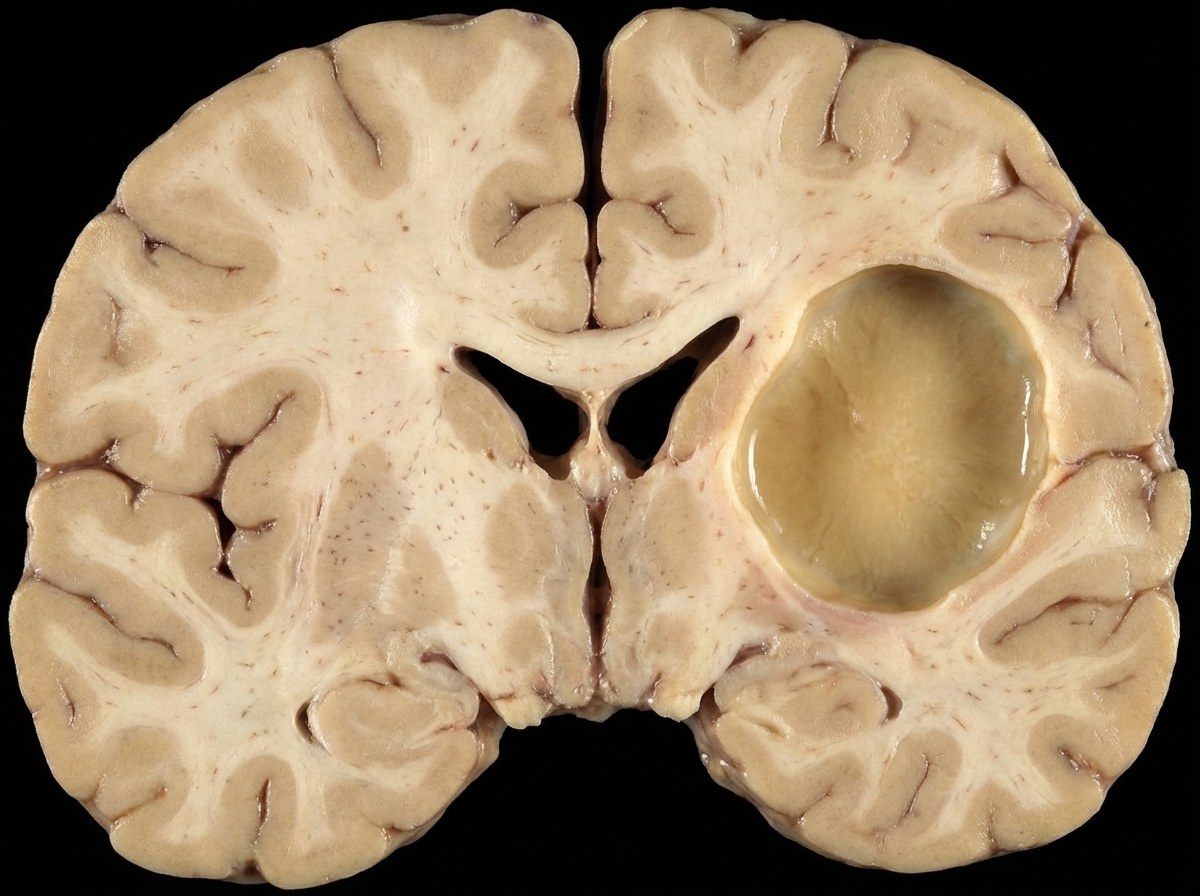
The given lesion is best associated with which of the following conditions?
Practice by Chapter
Cellular Pathology of the Nervous System
Practice Questions
Cerebrovascular Diseases
Practice Questions
Trauma to the Central Nervous System
Practice Questions
Infections of the Nervous System
Practice Questions
Demyelinating Diseases
Practice Questions
Neurodegenerative Diseases
Practice Questions
CNS Tumors
Practice Questions
Peripheral Nerve Disorders
Practice Questions
Neuromuscular Junction Diseases
Practice Questions
Congenital and Developmental Disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
