Neuropathology — MCQs

On this page
Cerebellar hemangioblastoma and retinal tumors are seen in which of the following conditions?
Which is the most common type of brain tumor?
Which tumor has the best prognosis?
Which of the following structures is most prone to hypoxic injury?
Elongated filaments in Pick's disease consist of?
Which of the following will manifest as pachymeningitis haemorrhagica interna?
Onion bulb appearance on nerve biopsy is seen in which of the following conditions?
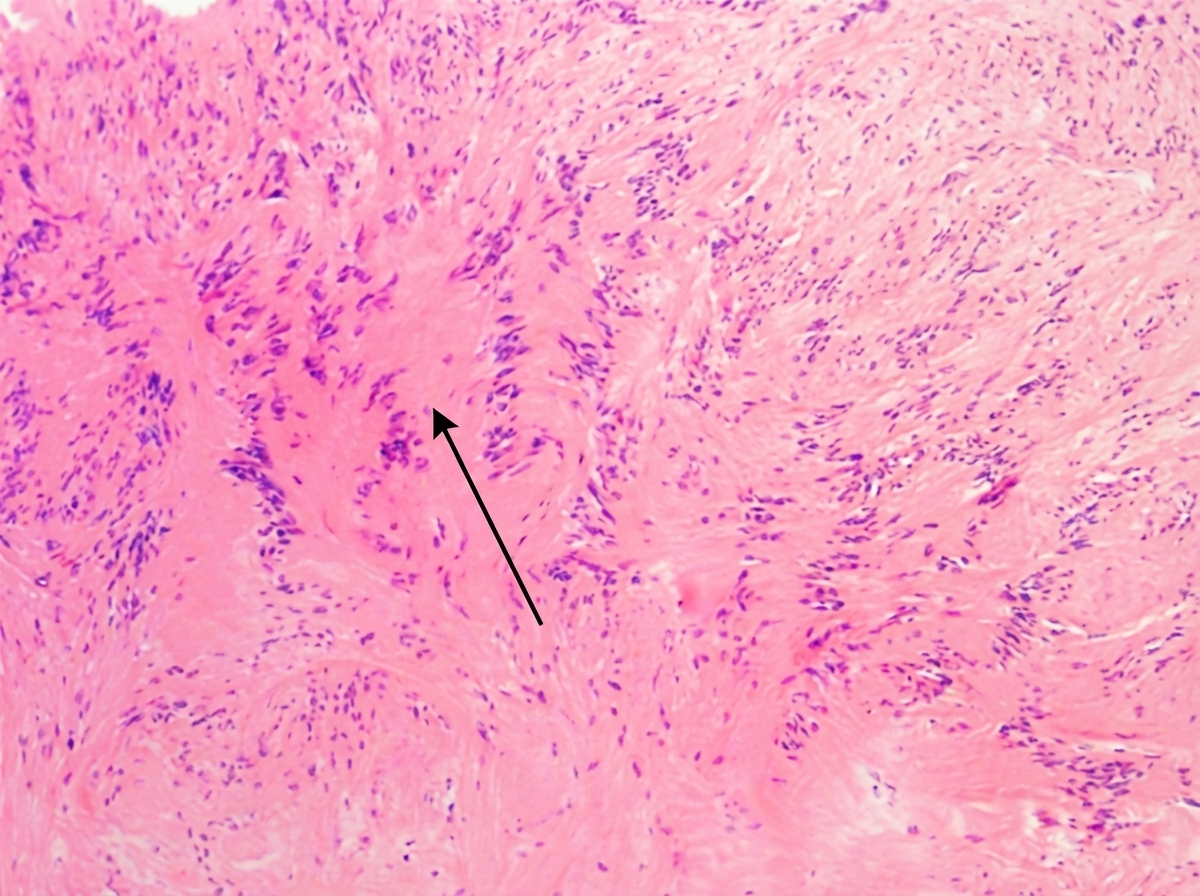
In the provided histopathology image of a schwannoma, what does the arrow-marked lesion represent?
Which is the most malignant primary brain tumor?
An 80-year-old female presents with progressive loss of memory, difficulty in recalling names, dysphasia, and irritability. Along with neurofibrillary tangles, what other pathological finding will be found in the brain?
Practice by Chapter
Cellular Pathology of the Nervous System
Practice Questions
Cerebrovascular Diseases
Practice Questions
Trauma to the Central Nervous System
Practice Questions
Infections of the Nervous System
Practice Questions
Demyelinating Diseases
Practice Questions
Neurodegenerative Diseases
Practice Questions
CNS Tumors
Practice Questions
Peripheral Nerve Disorders
Practice Questions
Neuromuscular Junction Diseases
Practice Questions
Congenital and Developmental Disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
