Neuropathology — MCQs

On this page
Which of the following statements is true about medulloblastoma?
All of the following are true about Primary CNS Lymphoma except:
What is the most common central nervous system (CNS) manifestation of HIV infection?
What is the most common site of brain metastasis?
Which of the following is NOT seen in HIV involvement of the CNS?
A 10-year-old boy presents with persistent headaches for 3 months. He has an ataxic gait and dysdiadochokinesia. A CT scan reveals a 4-cm cystic mass in the right cerebellar hemisphere with enlarged lateral ventricles. CSF analysis shows elevated protein and normal glucose. Intraoperative gross examination of the resected mass shows a cyst filled with gelatinous material, a thin wall, and a 1-cm mural nodule. Microscopic examination reveals cells positive for glial fibrillary acidic protein (GFAP) with long, hair-like processes. What is the most likely diagnosis?
What is the most common type of secondary brain tumor?
The marked area in the image of a Schwannoma represents which of the following?
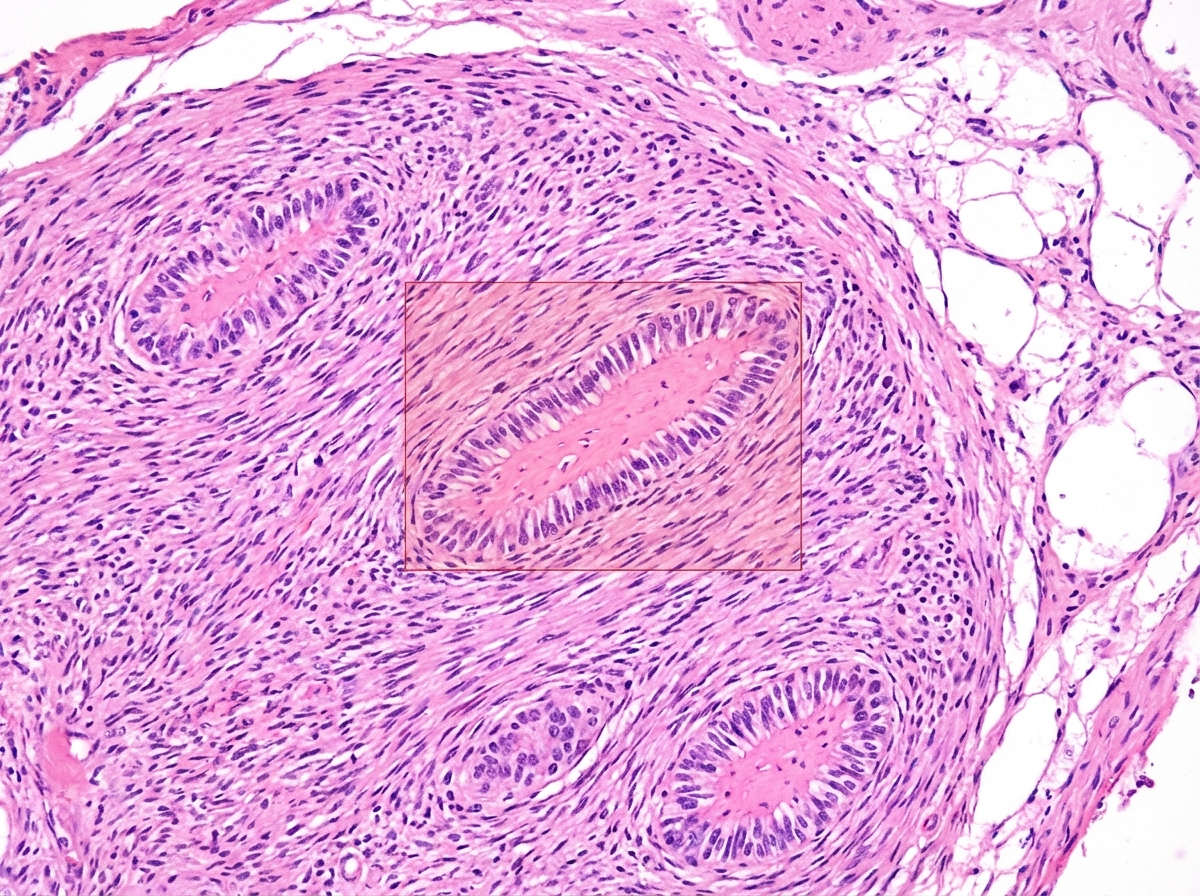
Multiple schwannomas are seen with which condition?
A young child presents with a mass in the posterior cranial fossa exhibiting a mural nodule. What is the most likely diagnosis?
Practice by Chapter
Cellular Pathology of the Nervous System
Practice Questions
Cerebrovascular Diseases
Practice Questions
Trauma to the Central Nervous System
Practice Questions
Infections of the Nervous System
Practice Questions
Demyelinating Diseases
Practice Questions
Neurodegenerative Diseases
Practice Questions
CNS Tumors
Practice Questions
Peripheral Nerve Disorders
Practice Questions
Neuromuscular Junction Diseases
Practice Questions
Congenital and Developmental Disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
