Parasitology — MCQs

On this page
Maximum density of microfilariae in blood is reported to be between -
What is the infective form of Trypanosoma brucei?
Which of the following amoebae does not have a neuropathogenic effect?
Which of the following is the only ovoviviparous parasite among the options provided?
In malaria, pre-erythrocytic schizogony occurs in -
Trophozoites in stool are characteristically seen in which of the following conditions?
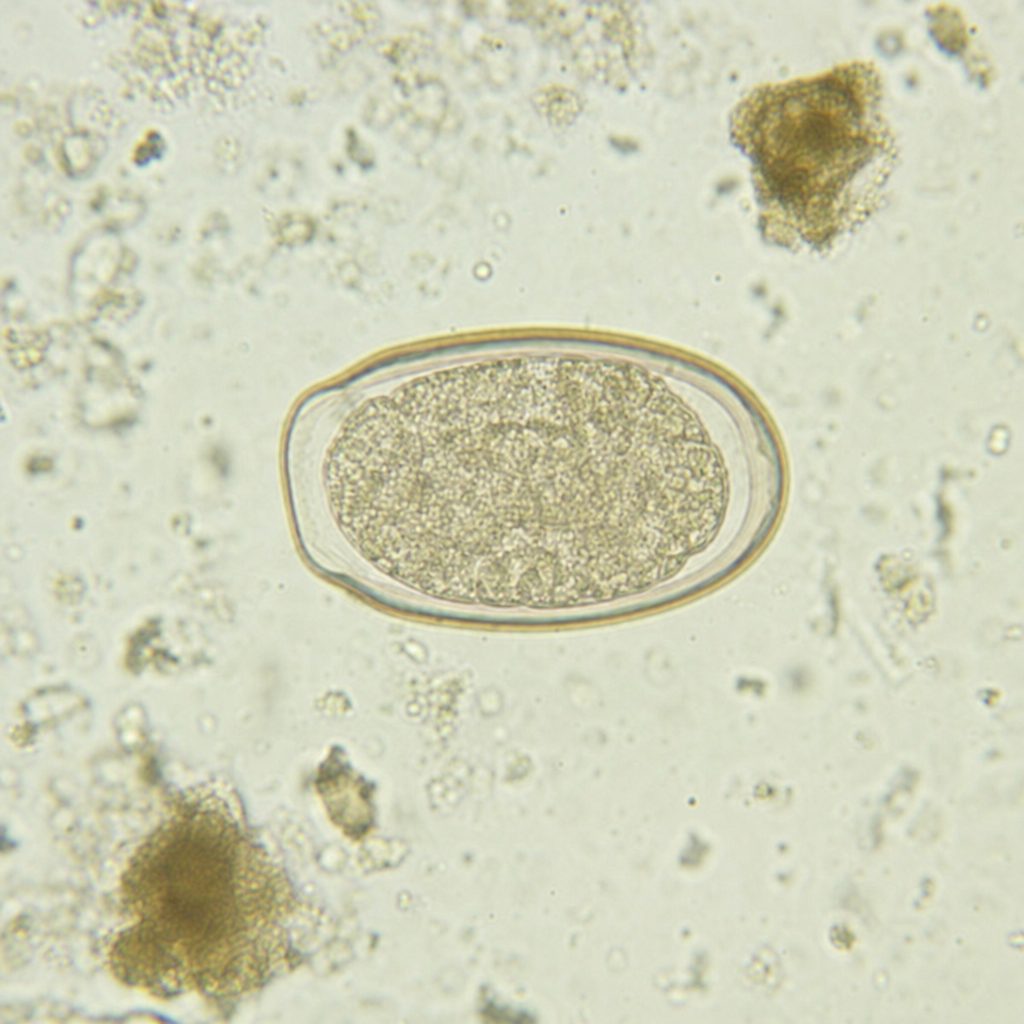
Child having perianal pruritus with the following eggs is due to -
Most common site for hydatid cyst
Cercariae are the infective form of which of the following parasites?
Which organism can be isolated from stool & sputum?
Practice by Chapter
Classification of Parasites
Practice Questions
Intestinal Protozoa
Practice Questions
Blood and Tissue Protozoa
Practice Questions
Malaria Parasites
Practice Questions
Leishmaniasis
Practice Questions
Intestinal Helminths: Nematodes
Practice Questions
Tissue Nematodes
Practice Questions
Trematodes
Practice Questions
Cestodes
Practice Questions
Ectoparasites
Practice Questions
Antiparasitic Drugs
Practice Questions
Laboratory Diagnosis of Parasitic Infections
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
