Parasitology — MCQs

On this page
Risk of transplacental transmission of Toxoplasma gondii is maximum when the mother is infected:
A 7-year-old child presented with intermittent abdominal cramps and loose stools. Stool examination revealed eggs measuring 100µm. Which of the following is NOT a cause of these symptoms?
A double rise of temperature in 24 hours is characteristic of which of the following conditions?
Trypanosoma cruzi grows in which of the following media?
Which of the following statements about Entamoeba histolytica is true?
Which of the following is NOT true about Cryptosporidium?
What is the definitive host for Echinococcus granulosus?
Chromidial bars are absent in which stage of cysts in Entamoeba?
Stool examination in a patient reveals a specific finding. What is the likely route of infection of this parasite?
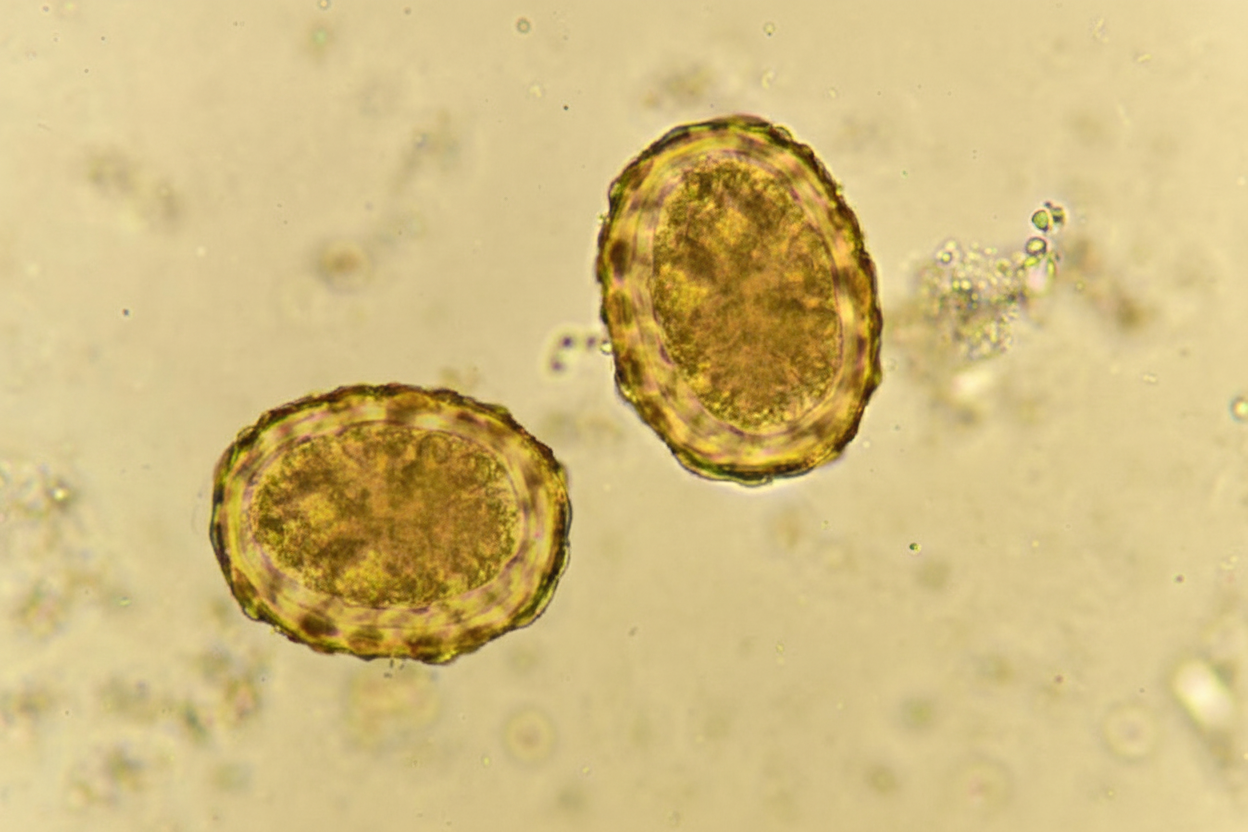
Which of the following leads to colonic ulcers?
Practice by Chapter
Classification of Parasites
Practice Questions
Intestinal Protozoa
Practice Questions
Blood and Tissue Protozoa
Practice Questions
Malaria Parasites
Practice Questions
Leishmaniasis
Practice Questions
Intestinal Helminths: Nematodes
Practice Questions
Tissue Nematodes
Practice Questions
Trematodes
Practice Questions
Cestodes
Practice Questions
Ectoparasites
Practice Questions
Antiparasitic Drugs
Practice Questions
Laboratory Diagnosis of Parasitic Infections
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
