Parasitology — MCQs

On this page
Flame cells are seen in which of the following groups of organisms?
What is the name of the test involving an intradermal injection of sterilised fluid from an infectious cyst?
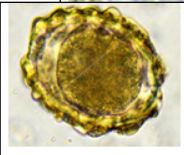
A stool sample from a patient shows ova. How do humans typically acquire this parasitic infection?
In giardiasis, malabsorption is due to all of the following except:
The man-snail-crab life cycle is characteristic of which parasite?
Which of the following helminths has a larval form that is typically found in stool?
Which of the following is NOT true about Plasmodium falciparum?
What is the lifespan of microfilaria in human blood?
Multiple infection of red blood cells is seen with which Plasmodium species?
Babesiosis is transmitted by the bite of which arthropod?
Practice by Chapter
Classification of Parasites
Practice Questions
Intestinal Protozoa
Practice Questions
Blood and Tissue Protozoa
Practice Questions
Malaria Parasites
Practice Questions
Leishmaniasis
Practice Questions
Intestinal Helminths: Nematodes
Practice Questions
Tissue Nematodes
Practice Questions
Trematodes
Practice Questions
Cestodes
Practice Questions
Ectoparasites
Practice Questions
Antiparasitic Drugs
Practice Questions
Laboratory Diagnosis of Parasitic Infections
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
