Parasitology — MCQs

On this page
In which location does Schistosoma japonicum reside?
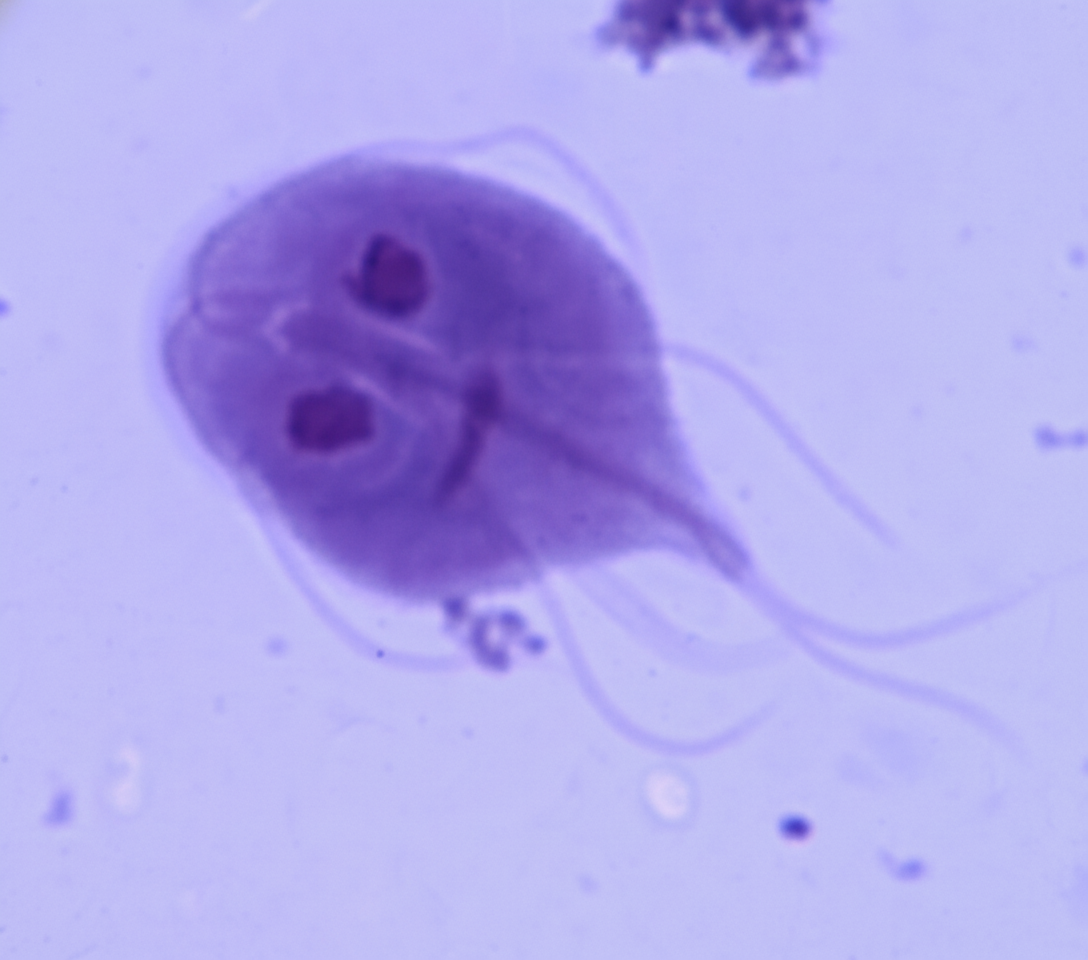
The number of pairs of flagella in the depicted organism is:
A biology graduate student who recently visited a tropical region of Africa presents with new visual impairment and the sensation that something is moving in her eye. She is concerned because she was warned about an eye disease transmitted by black flies. While in Africa, she was in a river area and received numerous black fly bites. She also has some subcutaneous nodules. If her infection was acquired by black fly bite, what is the most likely causative agent?
A 30-year-old farmer, treated initially with chloroquine for uncomplicated malaria, now has an episode of relapse. What could be the reason for relapse?
All of the following are true about Trichinella spiralis EXCEPT?
What is the vector for plague?
Which of the following eggs does not float on a saturated salt solution?
In occult filariasis, where are microfilariae typically found?
All of the following are true regarding Toxoplasmosis, except?
Visceral larva migrans is caused by which of the following organisms?
Practice by Chapter
Classification of Parasites
Practice Questions
Intestinal Protozoa
Practice Questions
Blood and Tissue Protozoa
Practice Questions
Malaria Parasites
Practice Questions
Leishmaniasis
Practice Questions
Intestinal Helminths: Nematodes
Practice Questions
Tissue Nematodes
Practice Questions
Trematodes
Practice Questions
Cestodes
Practice Questions
Ectoparasites
Practice Questions
Antiparasitic Drugs
Practice Questions
Laboratory Diagnosis of Parasitic Infections
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
