Parasitology — MCQs

On this page
Suramin is the drug of choice for which of the following conditions?
Vitamin B12 deficiency is seen in which tapeworm infestation?
The 'cyclops' stage is part of the life cycle of which of the following?
Autoinfection is seen with which of the following parasites?
What is the intermediate host for the parasite that causes hydatid disease?
Flask shaped ulcers are characteristically seen in which of the following conditions?
Eosinophilic meningoencephalitis is caused by which of the following?
Cysticercus cellulosae is seen in which of the following?
What is the most common site of abscess formation due to amoeba?
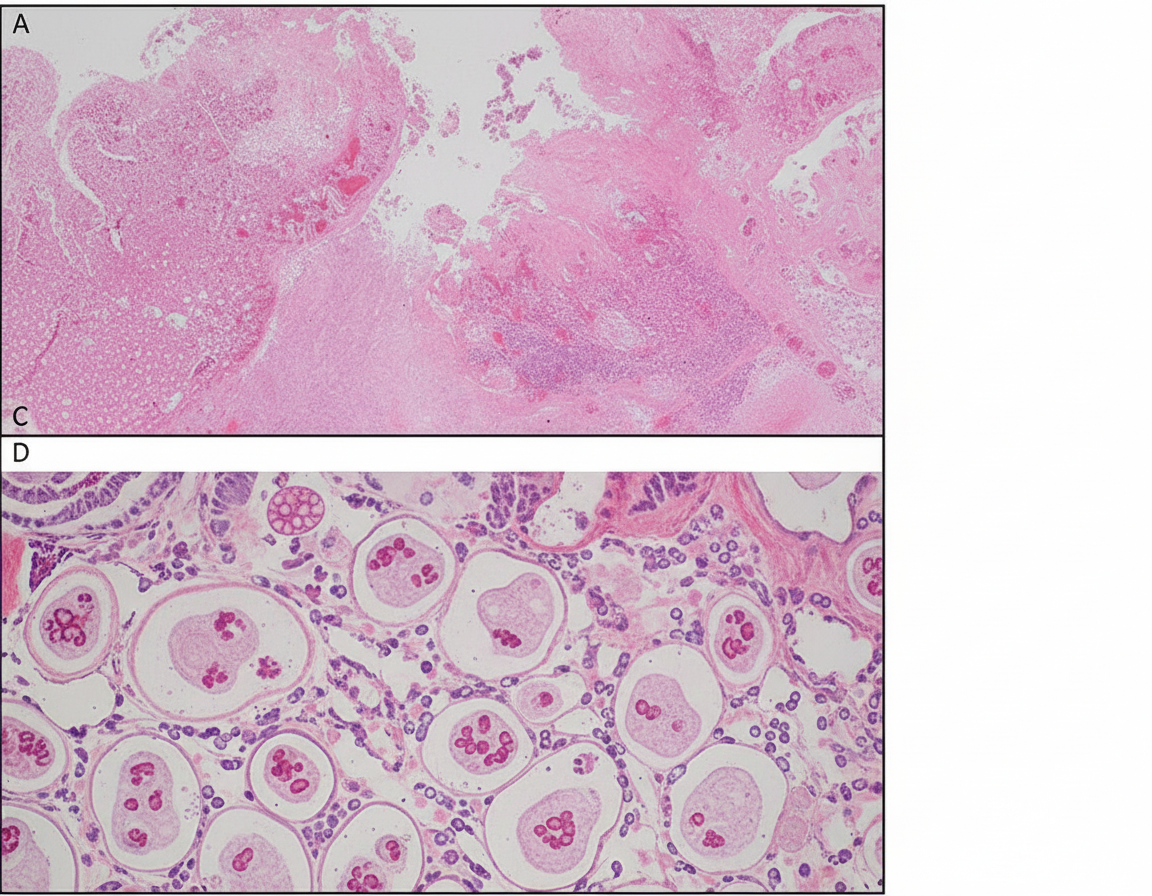
A 23-year-old male presented with abdominal pain and bloody diarrhea of one-week duration. What is the diagnosis based on the following rectal mucosa biopsy?
Practice by Chapter
Classification of Parasites
Practice Questions
Intestinal Protozoa
Practice Questions
Blood and Tissue Protozoa
Practice Questions
Malaria Parasites
Practice Questions
Leishmaniasis
Practice Questions
Intestinal Helminths: Nematodes
Practice Questions
Tissue Nematodes
Practice Questions
Trematodes
Practice Questions
Cestodes
Practice Questions
Ectoparasites
Practice Questions
Antiparasitic Drugs
Practice Questions
Laboratory Diagnosis of Parasitic Infections
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
