Candidiasis — MCQs

Which infection commonly spreads to newborns through caregivers?
Which drug should not be given with ketoconazole?
Most common catheter-related bloodstream infection is due to:
In an HIV-infected individual, the Gram stain of lung aspirate shows yeast-like morphology. Which of the following is the least likely diagnosis?
A 25 year old lady presented with curdy white discharge from the vagina is likely to be suffering from:-
A 65-year-old diabetic man presents with black necrotic tissue on his palate. What is the most likely causative organism?
Broad-based budding yeasts are seen in:
Brain abscess in immunodeficient person is due to :
Which statement is false regarding Cryptococcus neoformans?
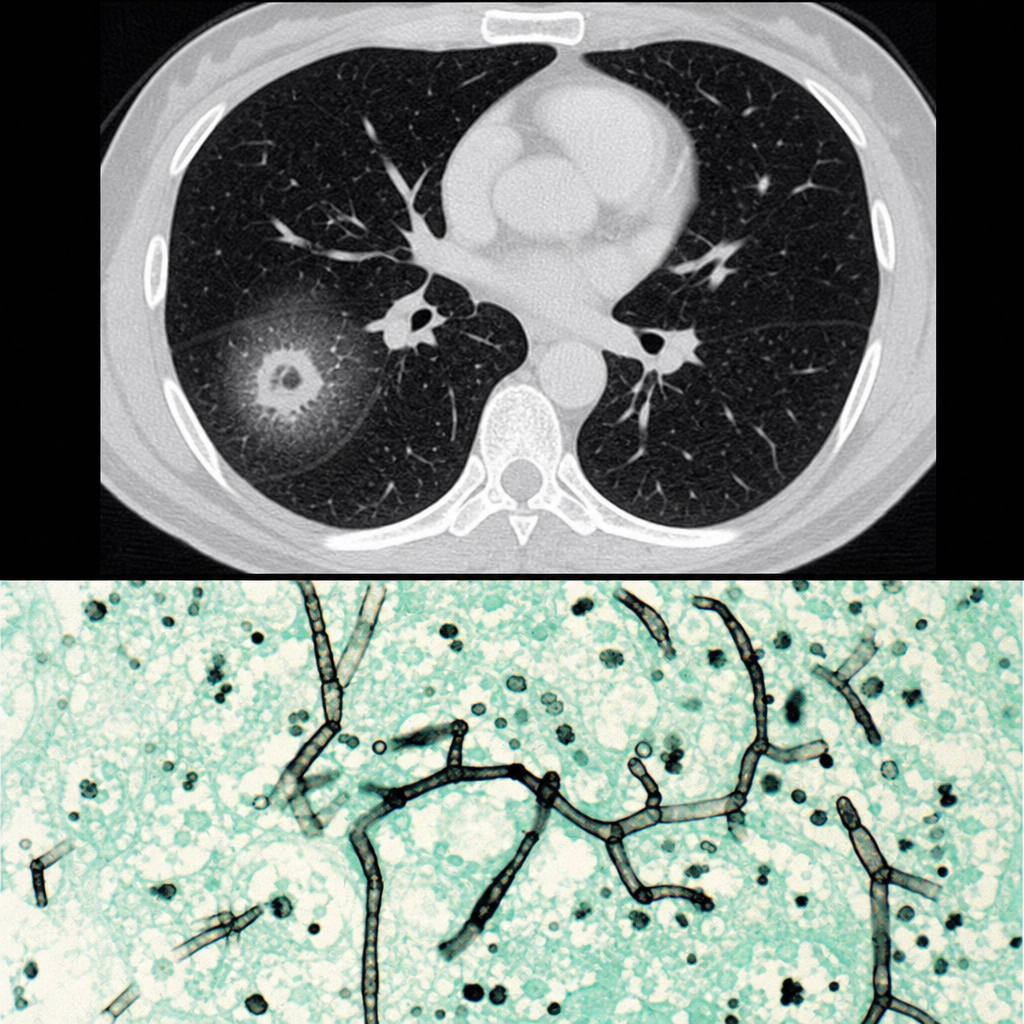
About 90 days post-bone marrow transplant, a 55-year-old white woman began to complain of dry cough, shortness of breath, and chest pain. She was started on antibiotics and blood culture obtained at the time was negative and there was not improvement. A computed tomography (CT) scan of the lungs showed a halo of low attenuation around a nodular lesion. Analysis of lung biopsy was similar to methenamine silver-stained section below. What is the most likely diagnosis for this patient?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
