General Microbiology — MCQs

On this page
Formaldehyde gas sterilization is employed for which of the following?
A patient from a tribal area of Jharkhand presents with fever for the last 3 days. Peripheral blood is collected and stained with Giemsa. A diagnosis of malaria is made. The smear is shown in the figure. What is the likely causative species?
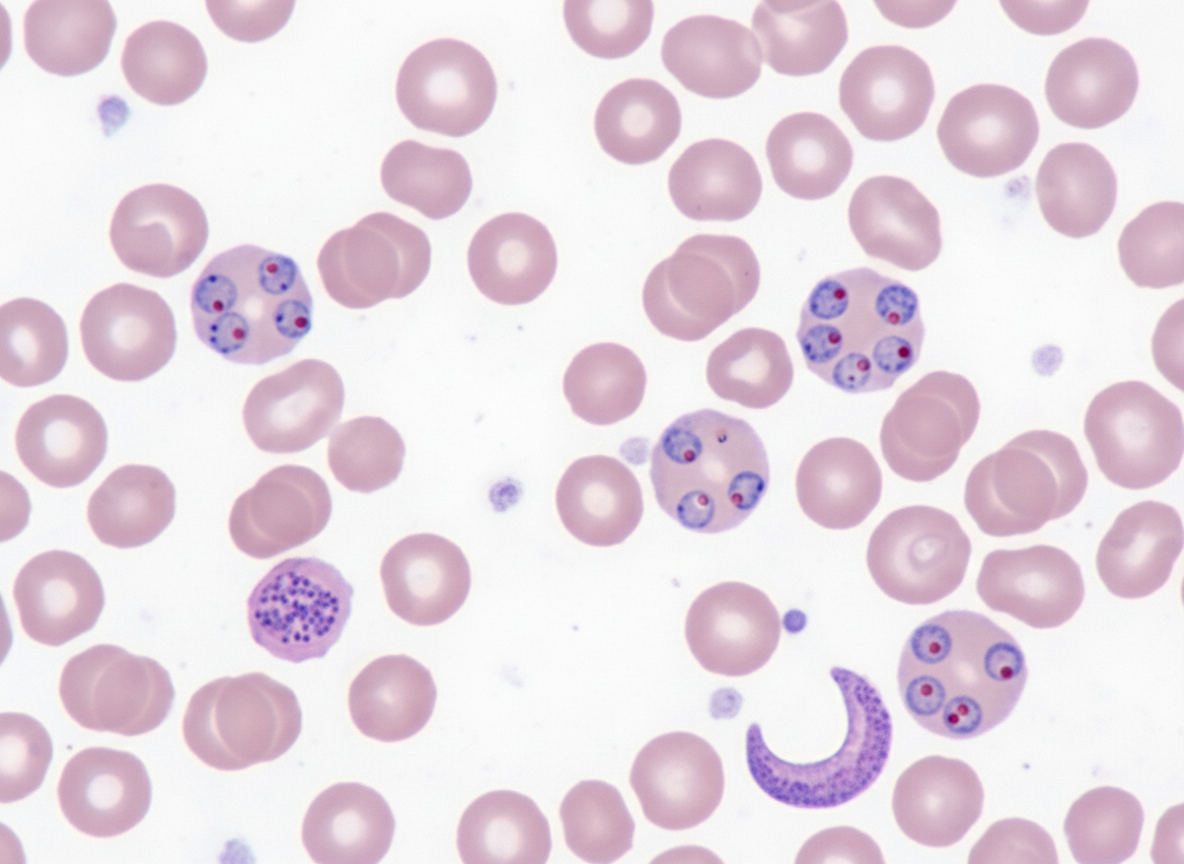
Which animal is primarily used for the production of monoclonal antibodies?
A bacterium divides every 20 minutes. If the population starts with a single bacterium and grows exponentially for 3 hours, how many bacteria will be present?
Pasteur developed vaccines for which of the following diseases?
Which method is used for sterilization by steam under pressure?
What is the approximate ratio of anaerobes to aerobes found in normal human stool?
NNN media is used for the culture of which organism?
Louis Pasteur is associated with all of the following except:
Which immunoglobulin acts as the B cell receptor?
Practice by Chapter
History and Scope of Microbiology
Practice Questions
Classification of Microorganisms
Practice Questions
Bacterial Morphology and Structure
Practice Questions
Bacterial Physiology and Metabolism
Practice Questions
Bacterial Genetics
Practice Questions
Microbial Growth and Nutrition
Practice Questions
Sterilization and Disinfection
Practice Questions
Bacterial Identification Methods
Practice Questions
Normal Microbiota and Pathogenicity
Practice Questions
Antimicrobial Susceptibility Testing
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
