Pulmonology — MCQs

On this page
Which of the following conditions is most commonly associated with a left-sided pleural effusion?
A 60-year-old obese male with a history of chronic smoking presents to the ICU with a pelvic fracture. On the 4th day of ICU stay, he develops sudden tachypnea, decreased SpO2, and hypotension. Echocardiography reveals right ventricular dilation and tricuspid regurgitation. What is the most appropriate next step in management?
Profuse expectoration of two months duration and clubbing may be seen in which of the following conditions?
A 50-year-old patient with long-standing chronic obstructive lung disease develops insidious onset of aching in the distal extremities, particularly the wrists bilaterally. There is a 9 kg weight loss. The skin over the wrists is warm and erythematous. There is bilateral clubbing. Plain film shows periosteal thickening, suggestive of osteomyelitis. What is the next best step in management?
A 25-year-old female presents with progressive dyspnea for one year. CXR shows interstitial opacities and spirometry shows an obstructive pattern. What is the diagnosis?
A 56-year-old man presents with a non-productive cough for 4 weeks. The most noticeable signs were grade III clubbing and a lesion in the apical lobe on X-ray. What is the most likely diagnosis?
Comment on the diagnosis based on spirometry findings: TLC = 75% of predicted, FRC = 100% of predicted, RV = 120% of predicted, FEV1 = 60% of predicted, DLco = 80% of predicted.
Which of the following statements is NOT true about chronic obstructive pulmonary disease?
A 70-year-old male smoker presents with cough and sputum production, but is afebrile. Lung examination reveals left-sided crackles, rhonchi, and egophony in the left upper lobe. The patient is being treated for an acute exacerbation of chronic bronchitis, and sputum is negative for AFB. What is the most likely cause of the observed chest X-ray findings in the left upper lobe?
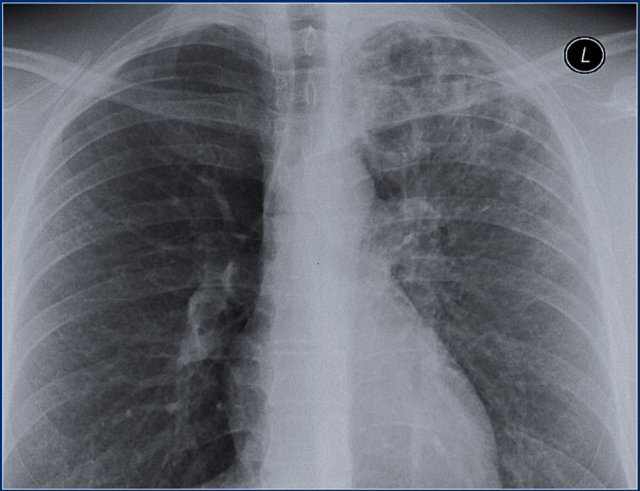
Cryptogenic organizing pneumonia is characterized by all of the following except?
Practice by Chapter
Obstructive Airway Diseases (Asthma, COPD)
Practice Questions
Interstitial Lung Diseases
Practice Questions
Pulmonary Infections
Practice Questions
Pulmonary Vascular Diseases
Practice Questions
Pleural Diseases
Practice Questions
Sleep-Disordered Breathing
Practice Questions
Respiratory Failure
Practice Questions
Mediastinal Disorders
Practice Questions
Occupational Lung Diseases
Practice Questions
Pulmonary Function Testing
Practice Questions
Bronchiectasis and Cystic Fibrosis
Practice Questions
Lung Cancer Approach
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
