Neurology — MCQs

On this page
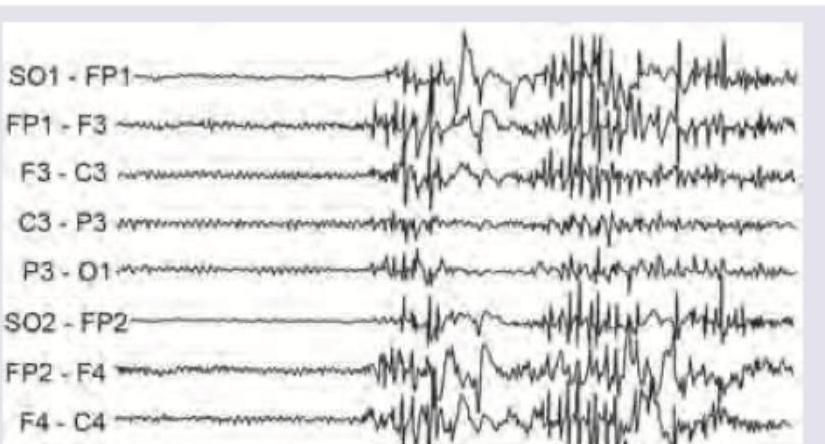
The EEG shows presence of:
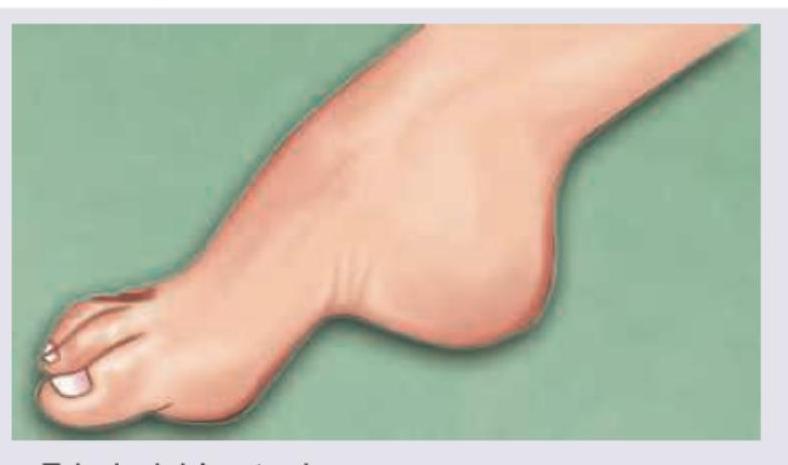
A 14-year-old boy presents with bilateral foot contractures. On examination, thickened peripheral nerves are noted. On biopsy of the nerve, a typical onion bulb appearance is noted. What is the probable diagnosis? (Recent NEET Pattern 2016-17)
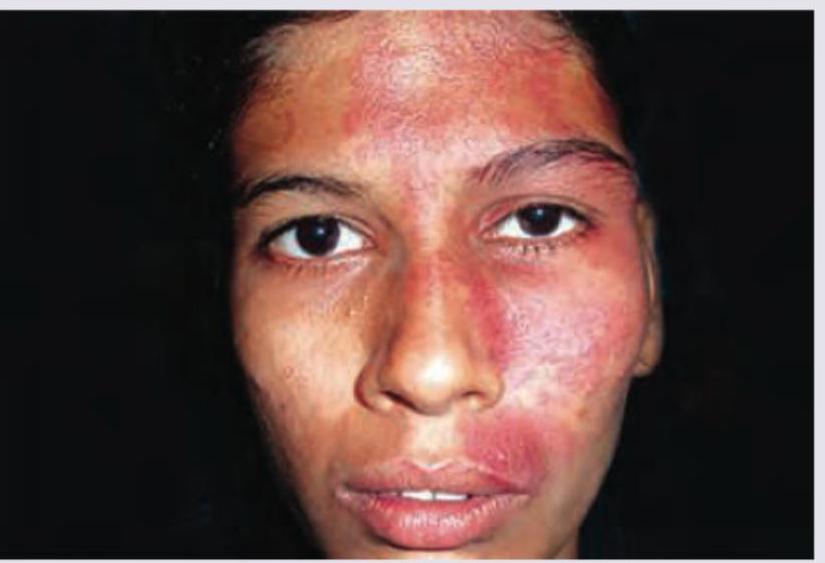
An 18-year-old patient presents with port wine stain, mental retardation and recurrent focal seizures. All are true about the condition except:
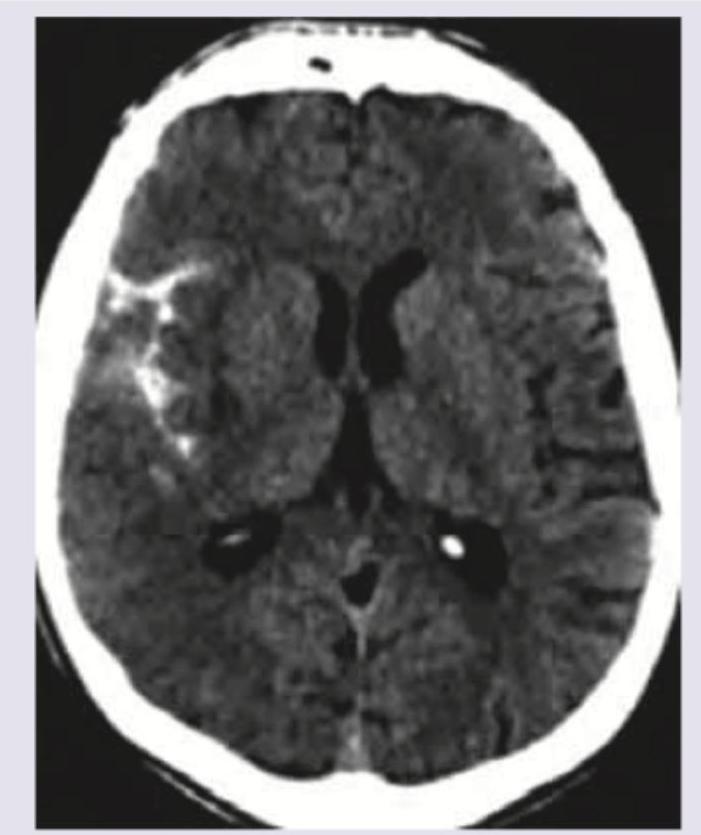
A 35-year-old woman presents with thunderclap headache. NCCT was done. All are true about the condition except:
A 60-year-old man presents with history of memory loss and fatigue. On examination, he has bradykinesia with axial rigidity. Resting tremor is absent and patient has broad-based gait with tendency to fall. MRI was done. All are true about the condition except:
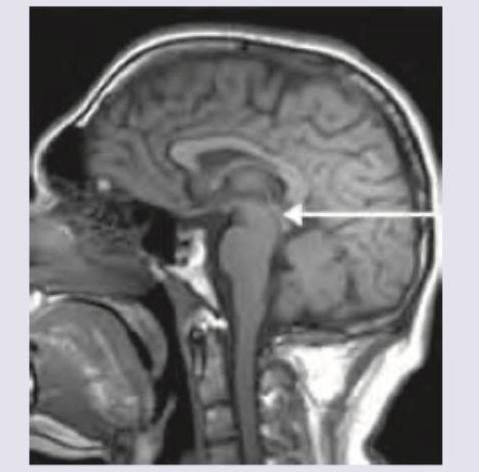
MRI was performed on a 35-year-old man with progressive myoclonus and apathy. What is the diagnosis? (Recent NEET Pattern 2016-17)
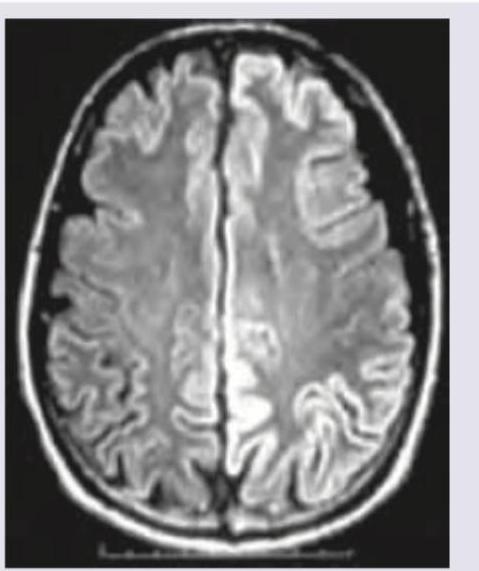
A 30-year-old patient has suffered from multiple episodes of GTCS for the last one week. MRI was performed. All are true about the condition except:
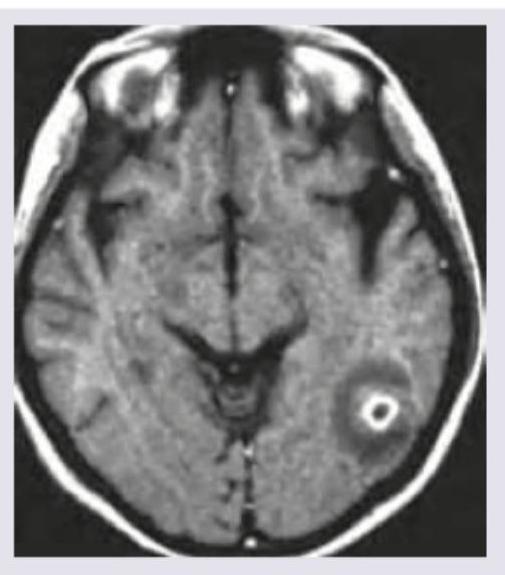
A middle-aged patient presents with history of left sided weakness for 2 days. Currently the patient is extremely drowsy and underwent a NCCT brain. Which of the following is the best treatment for this patient? (AIIMS Nov 2017)
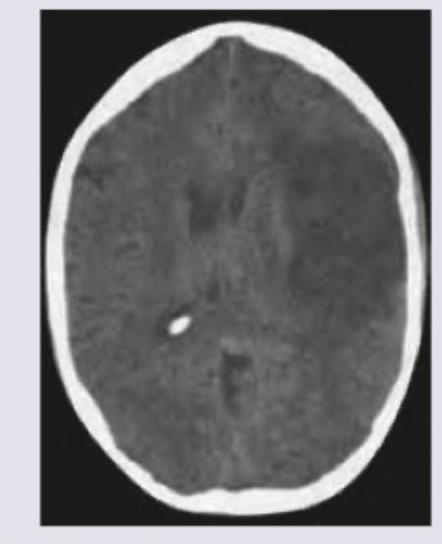
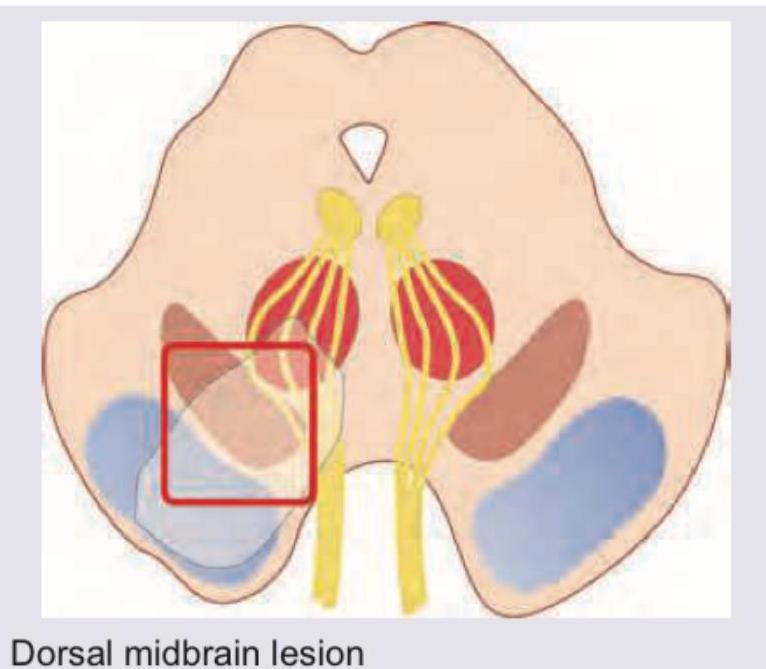
All are true about the mid brain stroke syndrome shown except:
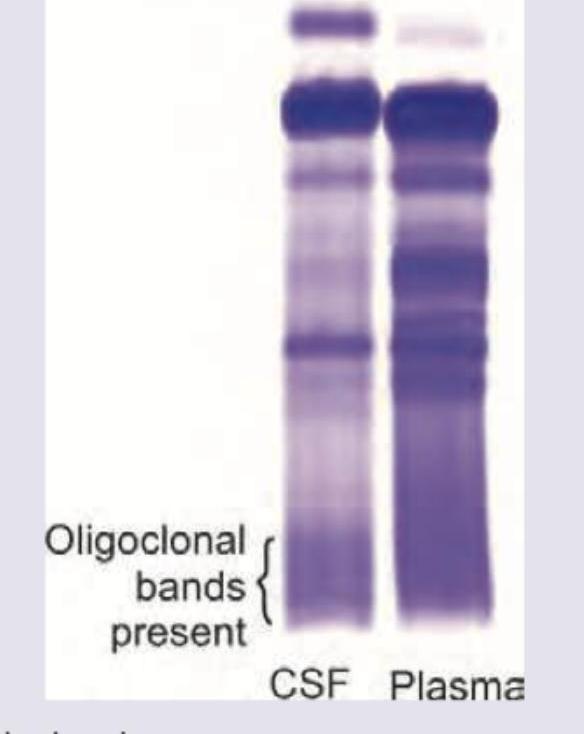
The CSF electrophoresis of patient shows oligoclonal bands. Which of the following is associated.
Practice by Chapter
Cerebrovascular Diseases
Practice Questions
Seizure Disorders and Epilepsy
Practice Questions
Headache Disorders
Practice Questions
Movement Disorders
Practice Questions
Demyelinating Diseases
Practice Questions
Neurodegenerative Disorders
Practice Questions
Neuromuscular Junction Disorders
Practice Questions
Peripheral Neuropathies
Practice Questions
CNS Infections
Practice Questions
Neuro-oncology
Practice Questions
Dementia and Cognitive Disorders
Practice Questions
Neurological Emergencies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
