Neurology — MCQs

On this page
The EEG of the patient shows which of the following? (Recent NEET Pattern 2016-17)
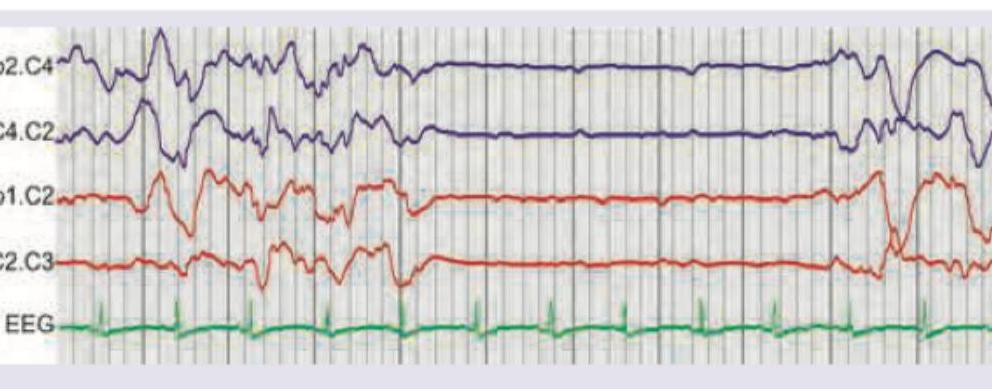
A 65-year-old man with dementia and poor hygiene due to urinary incontinence was evaluated. On examination: Deep tendon reflexes are brisk and gait apraxia with start hesitation is noted. CT scan was performed. What is the diagnosis?
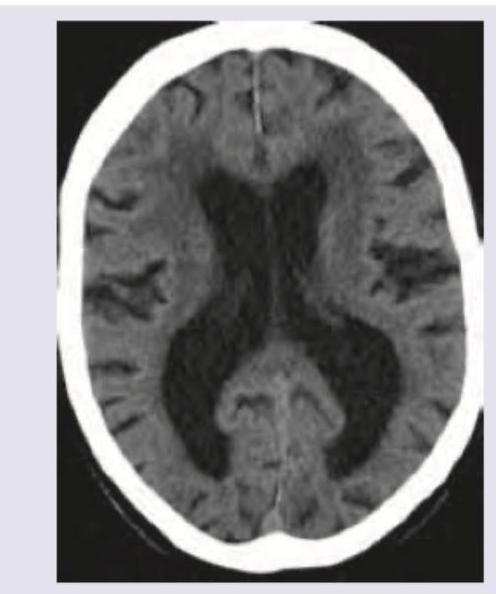
Identify the neurocutaneous disorder.
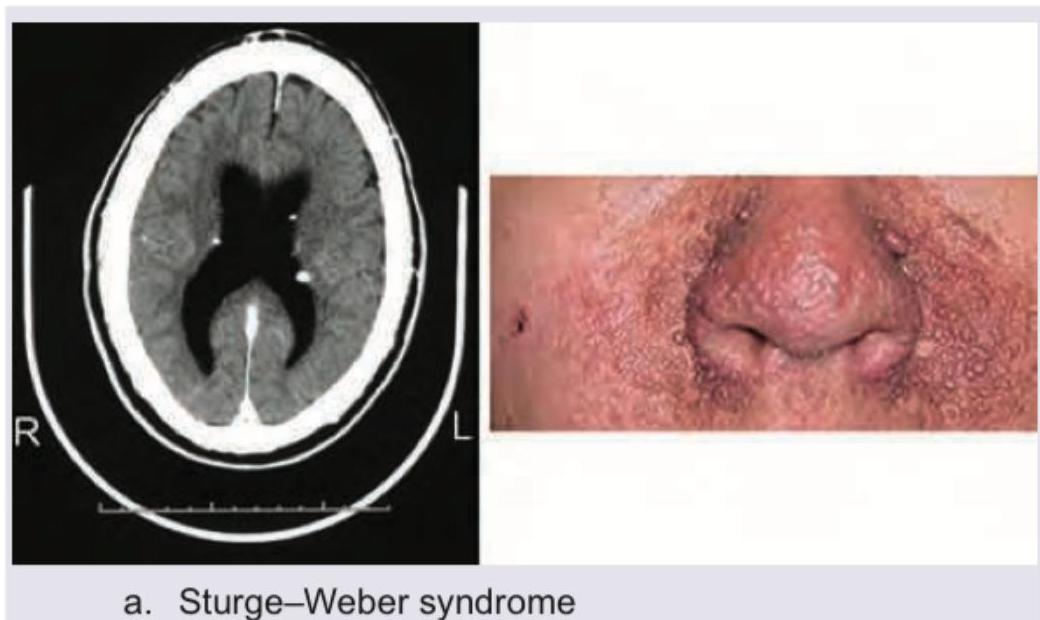
A patient presents with GCS of 7 with nuchal rigidity and bloody CSF. Which is incorrect regarding this condition? (Recent NEET Pattern 2016-17)
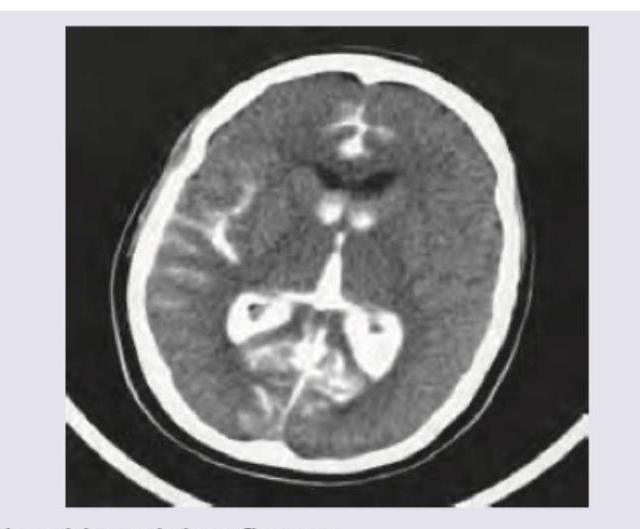
A 50-year-old hypertensive patient develops sudden onset drooping of right face and hemiplegia. What is the diagnosis?
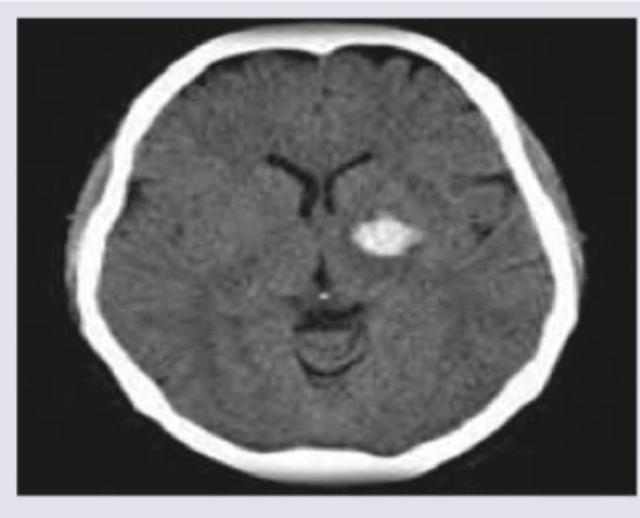
Which is correct for the image shown below?
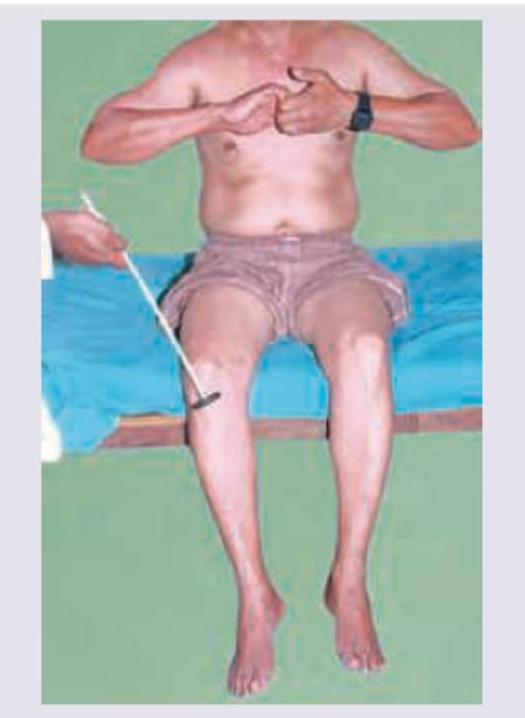
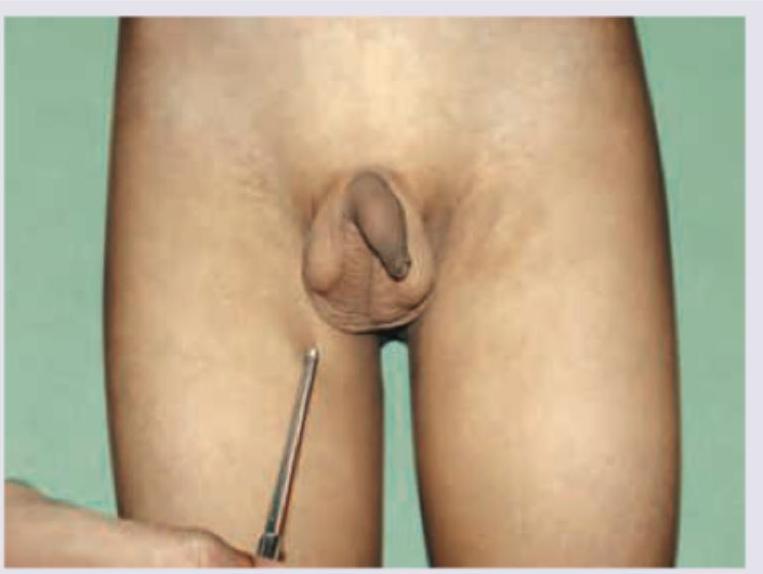
Which reflex is being elicited in the patient?
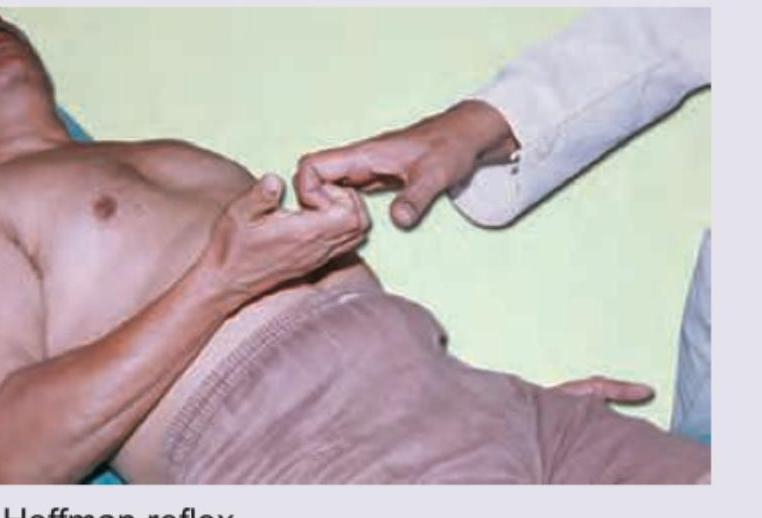
All are correct about the reflex being elicited except:
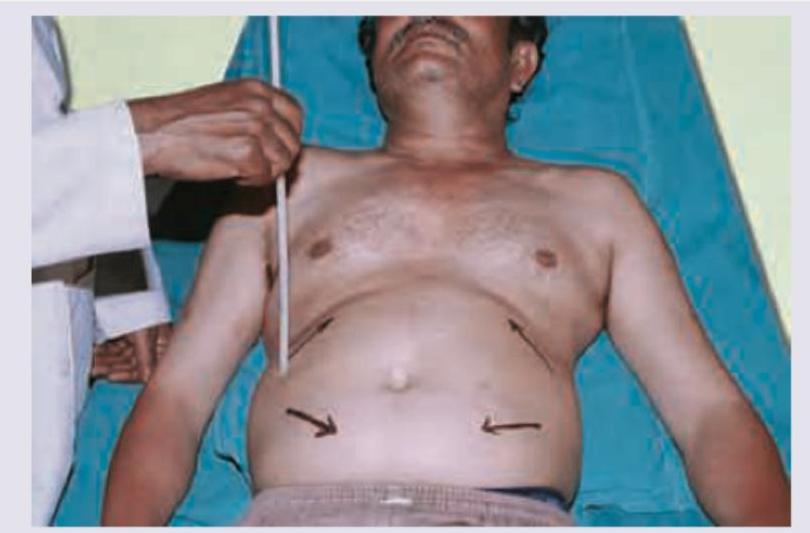
All are true about the reflex being elicited except?
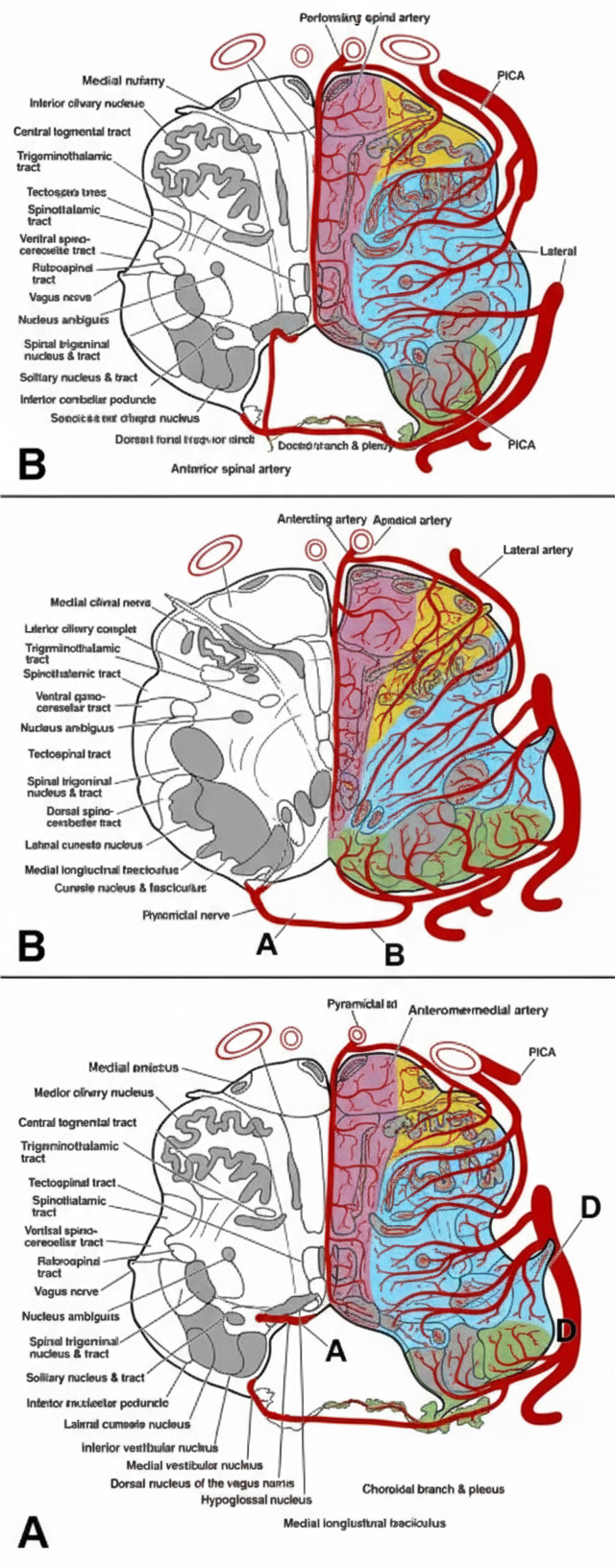
Medial medullary syndrome occurs due to blockage of which of the following blood vessel?
Practice by Chapter
Cerebrovascular Diseases
Practice Questions
Seizure Disorders and Epilepsy
Practice Questions
Headache Disorders
Practice Questions
Movement Disorders
Practice Questions
Demyelinating Diseases
Practice Questions
Neurodegenerative Disorders
Practice Questions
Neuromuscular Junction Disorders
Practice Questions
Peripheral Neuropathies
Practice Questions
CNS Infections
Practice Questions
Neuro-oncology
Practice Questions
Dementia and Cognitive Disorders
Practice Questions
Neurological Emergencies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
