Neurology — MCQs

On this page
A 26-year-old male with a history of respiratory tract infection 4 weeks ago is unable to stand or walk for the past 2 weeks and the weakness is progressive, ascending, and symmetrical in nature. The lower limbs were involved before and gradually the upper limbs were also affected. On examination you note areflexia. Pain and proprioception are preserved. What is the probable diagnosis?
A young male patient presents with ptosis and muscle weakness, which reportedly worsens in the evening and improves in the morning. This is relieved by neostigmine. What is the likely diagnosis?
What is the drug of choice for this medical condition showing periventricular lesions?
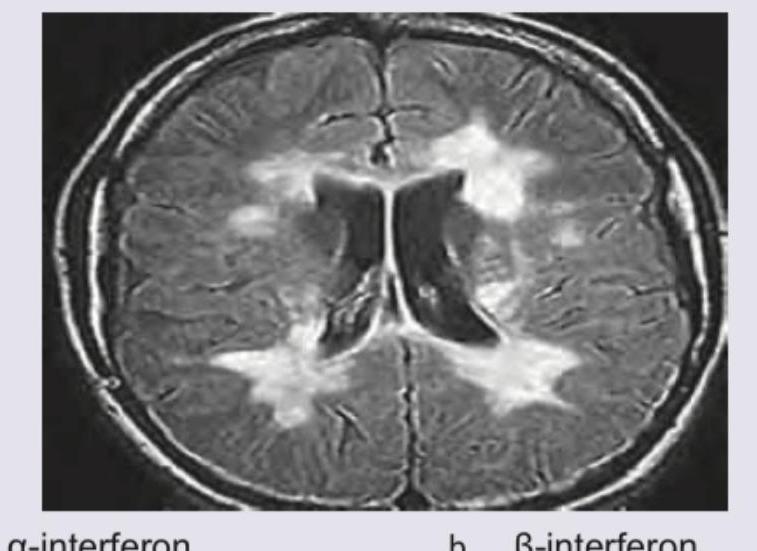
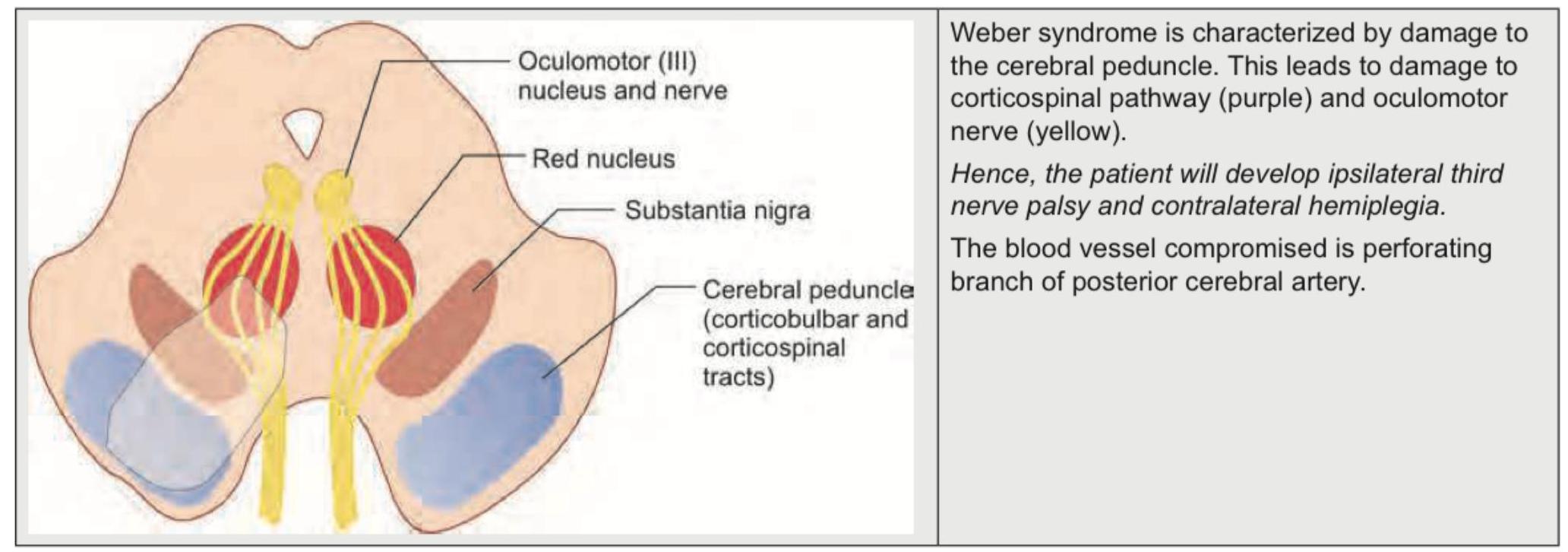
Which of the following is incorrect about the condition shown below?
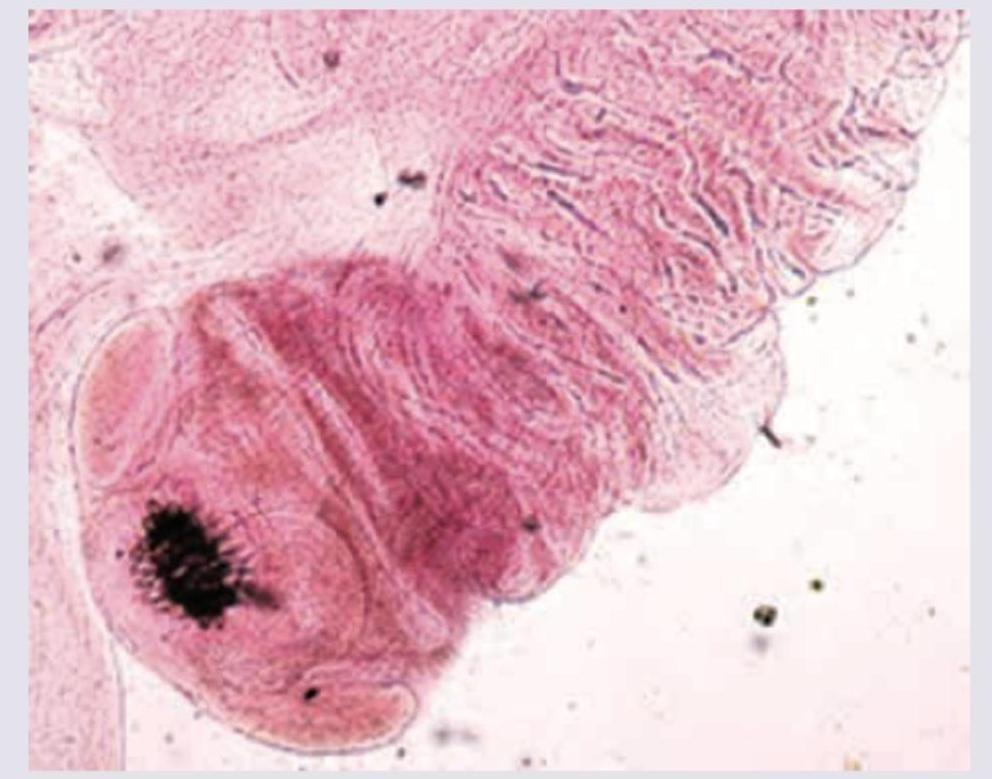
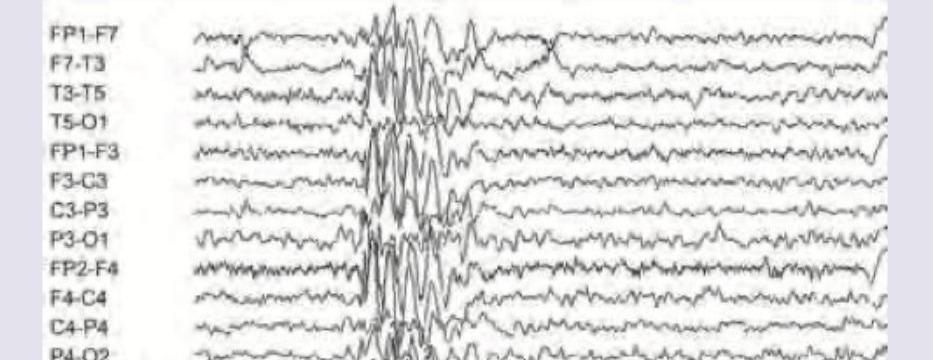
A 15-year-old boy presented with day dreaming and decline in school performance. EEG shows.
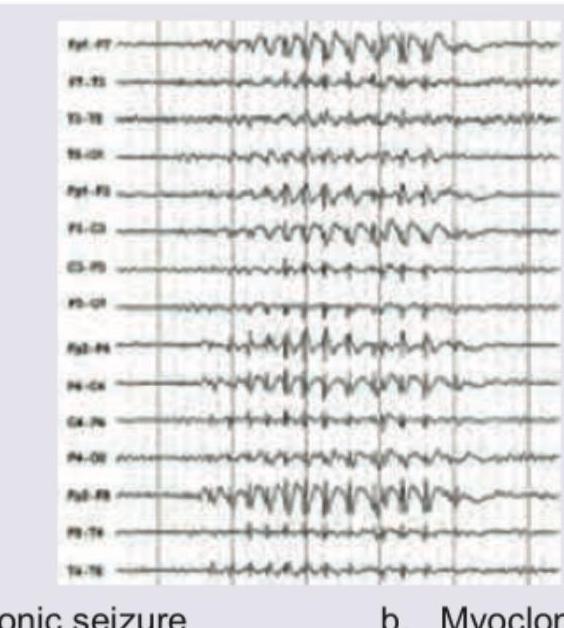
Which of the following is true regarding type of seizures shown in EEG?
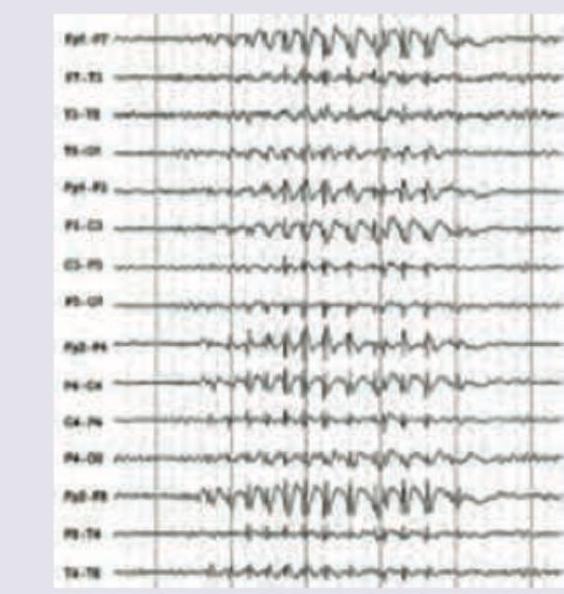
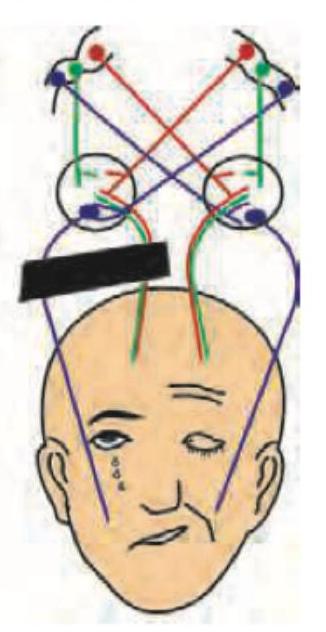
A patient presents with facial deviation to the right, inability to close the left eye with Bell's sign, and unclear ability to produce wrinkles on the forehead based on the image. What is the most likely diagnosis?
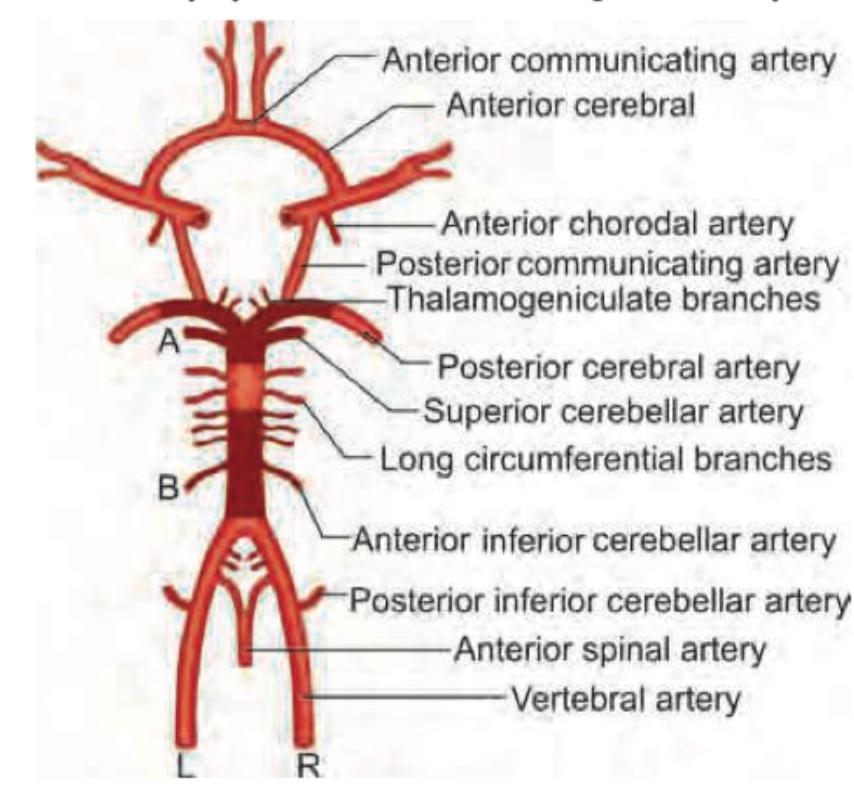
The following diagram and its branches should be remembered. The blood vessel involved in medial medullary syndrome is anterior spinal artery.
Which of the following is characteristic of Parinaud's syndrome?
The EEG of a 16-year-old boy with early morning involuntary movements of hands in his sleep noticed by parents, was performed. Immunization is complete. What does EEG show? (Recent NEET Pattern 2016-17)
Practice by Chapter
Cerebrovascular Diseases
Practice Questions
Seizure Disorders and Epilepsy
Practice Questions
Headache Disorders
Practice Questions
Movement Disorders
Practice Questions
Demyelinating Diseases
Practice Questions
Neurodegenerative Disorders
Practice Questions
Neuromuscular Junction Disorders
Practice Questions
Peripheral Neuropathies
Practice Questions
CNS Infections
Practice Questions
Neuro-oncology
Practice Questions
Dementia and Cognitive Disorders
Practice Questions
Neurological Emergencies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
