Infectious Diseases — MCQs

On this page
The following are parvovirus - related disease - population pairs. Identify the incorrect pair. 1. Aplastic anemia - Patient with hereditary hemolytic anemia 2. Non - immune hydrops - pregnant women 3. Erythema infectiosum - infants 4. Non - erosive arthritis - Patients of SLE
An ICU patient is suffering from Rhinovirus infection. How do we treat the patient?
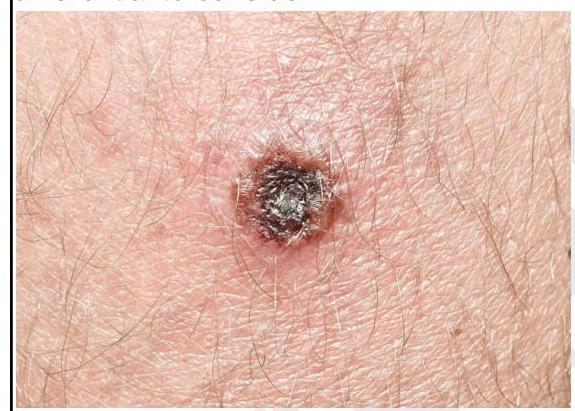
A forest officer develops the lesion as shown in the image. Which of the following is not a differential to consider?
A 45-year-old man presents with well-circumscribed, hypopigmented patches on his face and arms. The lesions are asymmetric and show decreased sensation to light touch. Microscopic examination of a skin biopsy stained with Fite stain shows acid-fast bacilli within macrophages in dermal nerve bundles. Which of the following is the most appropriate treatment?
In HIV-positive patients with gonorrhea, which of the following statements is TRUE regarding management?
A 42-year-old man with a history of gout and hypertension presents to his family physician with a complaint of increased left knee pain over the past 2 days. He also reports swelling and redness of the left knee and is unable to bear weight on that side. He denies any prior surgery or inciting trauma to the knee. His temperature is 97.0°F (36.1°C), blood pressure is 137/98 mm Hg, pulse is 80/min, respirations are 13/min, and oxygen saturation is 98% on room air. Physical examination reveals a left knee that is erythematous, swollen, warm-to-touch, and extremely tender to palpation and with attempted flexion/extension movement. His left knee range of motion is markedly reduced compared to the contralateral side. Joint aspiration of the left knee is performed with synovial fluid analysis showing turbid fluid with a leukocyte count of 95,000/mm^3, 88% neutrophils, and a low glucose. Gram stain of the synovial fluid is negative. Results from synovial fluid culture are pending. Which of the following is the best treatment regimen for this patient?
A 27-year-old woman who resides in an area endemic for chloroquine-resistant P. falciparum malaria presents to the physician with fatigue, malaise, and episodes of fever with chills over the last 5 days. She mentions that she has episodes of shivering and chills on alternate days that last for approximately 2 hours, followed by high-grade fevers; then she has profuse sweating and her body temperature returns to normal. She also mentions that she is currently in her 7th week of pregnancy. The physical examination reveals the presence of mild splenomegaly. A peripheral blood smear confirms the diagnosis of P. falciparum infection. Which of the following is the most appropriate anti-malarial treatment for the woman?
A 28-year-old man presents to the physician because of dizziness and palpitations for the past 12 hours and fever, malaise, headache, and myalgias for the past week. The patient traveled into the woods of Massachusetts 4 weeks ago. He has no known chronic medical conditions, and there is no history of substance use. His temperature is 38.3°C (100.9°F), pulse is 52/min, respirations are 16/min, and blood pressure is 126/84 mm Hg. His physical examination shows a single, 10-cm, round, erythematous lesion with a bull’s-eye pattern in the right popliteal fossa. His electrocardiogram shows Mobitz I second-degree atrioventricular (AV) block. The complete blood cell count and serum electrolyte levels are normal, but the erythrocyte sedimentation rate is 35 mm/hour. What is the most likely cause of the patient’s cardiac symptoms?
A 35-year-old lady who presented with a 6-month painless fluctuant, non-transilluminant swelling with a thin watery discharge. Clinical diagnosis is?
Subacute Sclerosing Panencephalitis is a rare and dangerous complication of;
Practice by Chapter
Principles of Antimicrobial Therapy
Practice Questions
Fever of Unknown Origin
Practice Questions
HIV/AIDS and Related Infections
Practice Questions
Tuberculosis and Mycobacterial Diseases
Practice Questions
Tropical and Parasitic Infections
Practice Questions
Viral Infections (Hepatitis, Herpes, etc.)
Practice Questions
Healthcare-Associated Infections
Practice Questions
Fungal Infections
Practice Questions
Sepsis and Septic Shock
Practice Questions
Infection in Immunocompromised Hosts
Practice Questions
Emerging and Re-emerging Infections
Practice Questions
Antimicrobial Resistance
Practice Questions
Vaccination Principles
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
