Infectious Diseases — MCQs

On this page
A 27-year-old HIV-positive man (CD4 count 250/μL) presents with a 2-month history of perianal ulcer that is painless, clean-based, and indurated. Dark field microscopy and PCR for HSV are negative. VDRL is 1:64, and TPHA is positive. Lumbar puncture shows 30 WBCs (predominantly lymphocytes) and CSF-VDRL is reactive. Despite receiving standard benzathine penicillin therapy 2 weeks ago, the ulcer persists unchanged. What is the most appropriate next step?
A 22-year-old man presents with urethral discharge and dysuria for 3 days. Gram stain shows intracellular gram-negative diplococci. Two weeks after appropriate treatment, he returns with similar symptoms. Repeat testing shows no organisms on Gram stain but leukocytes are present. What is the most likely explanation?
How does HIV infection alter the natural history of syphilis?
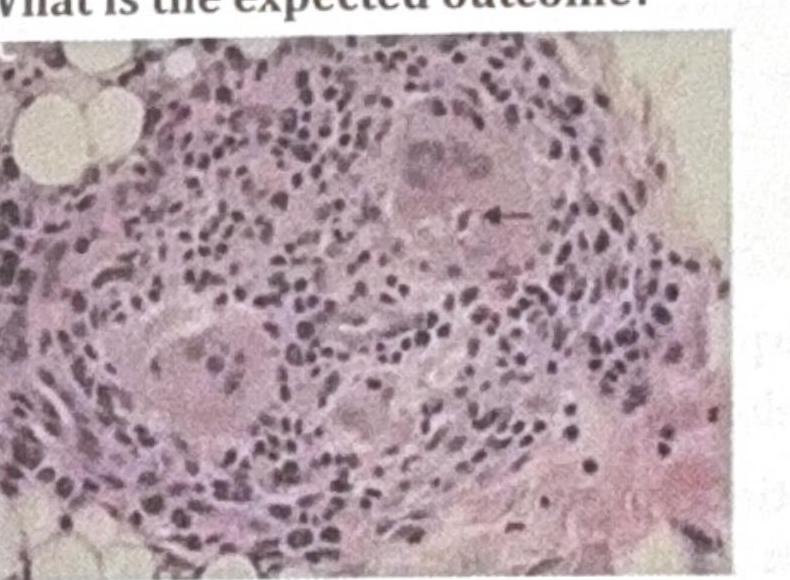
A patient presents with loss of sensation along the ulnar nerve path. The histology is shown in the image, and a Lepromin test was performed. What is the expected outcome?
A patient living with HIV presents with foulsmelling stools. Microscopic examination of the stool reveals no cysts or ova, but a 200-micrometer larva is observed. What is the most likely pathogen?
A farmer presents with severe leg pain, fever, chills, retro-orbital pain, and bilateral conjunctival suffusion. What is the most likely diagnosis?
A 15-year-old patient presents with joint swelling, a pan-systolic murmur, negative rheumatoid factor (RF), and elevated ESR. The patient also reports a recent history of sore throat and exhibits subcutaneous nodules and erythema marginatum on physical examination. What is the most likely diagnosis?
What is the most common site of abdominal tuberculosis?
A patient, who is a known case of HIV with a CD4 count of 200 cells/cu.mm, presents with 5 days of cough and high-grade fever without chills and rigors. There is no history of diarrhoea, vomiting, or nuchal rigidity. Chest x-ray is normal. What treatment will you give?
A person presents to the hospital with fever and chills. Fever profile is ordered and is found to be negative for malaria and dengue. Rk39 test is found to be positive. What is the treatment of choice?
Practice by Chapter
Principles of Antimicrobial Therapy
Practice Questions
Fever of Unknown Origin
Practice Questions
HIV/AIDS and Related Infections
Practice Questions
Tuberculosis and Mycobacterial Diseases
Practice Questions
Tropical and Parasitic Infections
Practice Questions
Viral Infections (Hepatitis, Herpes, etc.)
Practice Questions
Healthcare-Associated Infections
Practice Questions
Fungal Infections
Practice Questions
Sepsis and Septic Shock
Practice Questions
Infection in Immunocompromised Hosts
Practice Questions
Emerging and Re-emerging Infections
Practice Questions
Antimicrobial Resistance
Practice Questions
Vaccination Principles
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
