Infectious Diseases — MCQs

On this page
Tuberculosis in HIV positive individuals is characterized by which of the following? 1. More frequent negative sputum smears. 2. More false–negative tuberculin test results. 3. More extra–pulmonary tuberculosis. 4. More cavitating lesions in lungs as shown by chest X-ray. Select the correct answer using the code given below:
Which of the following is not a clinical feature of tetanus?
At present, treatment is recommended for H. pylori in association with the following except:
Consider the following statements regarding Opportunistic post-splenectomy infections (OPSI): 1. Haemophilus influenzae, Neisseria meningitidis and Streptococcus pneumoniae are the most common causative agents 2. Risk is greatest in the patients who have undergone splenectomy for trauma 3. Risk is greatest within the first 2–3 years following splenectomy 4. Prophylactic vaccination should be done 2 weeks prior to elective splenectomy Which of the statements given above are correct?
Which one of the following statements is NOT correct regarding Pyogenic Liver Abscess?
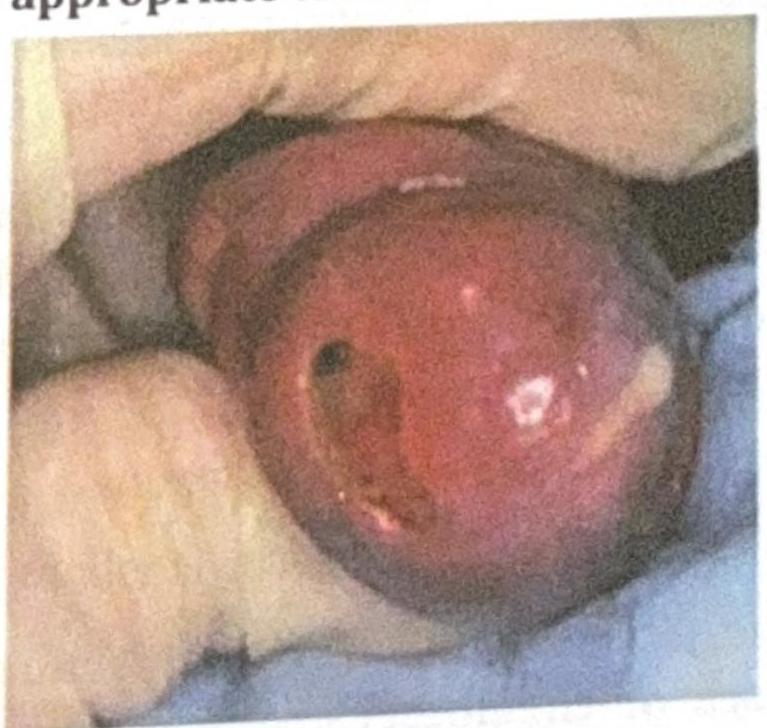
An adult man presents with the clinical condition shown in the image, and a Gram stain reveals Gram-negative diplococci. What is the most appropriate treatment?
A 25-year-old woman with HIV (CD4 count 320/μL) presents with vulvar ulceration for 3 weeks. Initial testing for HSV, syphilis, and chancroid is negative. Empiric treatment for these conditions does not improve the lesion. Biopsy shows a dense lymphoplasmacytic infiltrate with CMV inclusions. What is the most appropriate management?
Which factor most strongly influences vertical transmission risk of hepatitis B from mother to infant?
A 28-year-old man presents with recurrent urethritis despite appropriate treatment for gonorrhea and chlamydia. NAAT tests for both are negative. He reports adherence to therapy and denies reexposure. What is the most appropriate next step?
A 38-year-old man with HIV (CD4 count 150/μL) presents with progressive perianal ulceration for 3 months. Multiple biopsies show granulomatous inflammation without organisms. PCR for HSV, dark field microscopy, and serological tests for syphilis are negative. He has received empiric treatment for HSV and syphilis without improvement. What is the most likely diagnosis?
Practice by Chapter
Principles of Antimicrobial Therapy
Practice Questions
Fever of Unknown Origin
Practice Questions
HIV/AIDS and Related Infections
Practice Questions
Tuberculosis and Mycobacterial Diseases
Practice Questions
Tropical and Parasitic Infections
Practice Questions
Viral Infections (Hepatitis, Herpes, etc.)
Practice Questions
Healthcare-Associated Infections
Practice Questions
Fungal Infections
Practice Questions
Sepsis and Septic Shock
Practice Questions
Infection in Immunocompromised Hosts
Practice Questions
Emerging and Re-emerging Infections
Practice Questions
Antimicrobial Resistance
Practice Questions
Vaccination Principles
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
