Infectious Diseases — MCQs

On this page
A patient with HIV is newly diagnosed with multidrug-resistant tuberculosis. Which of the following is the appropriate regimen, and what should the patient be monitored for?
According to WHO, which of the following is the recommended diagnostic test for spinal tuberculosis?
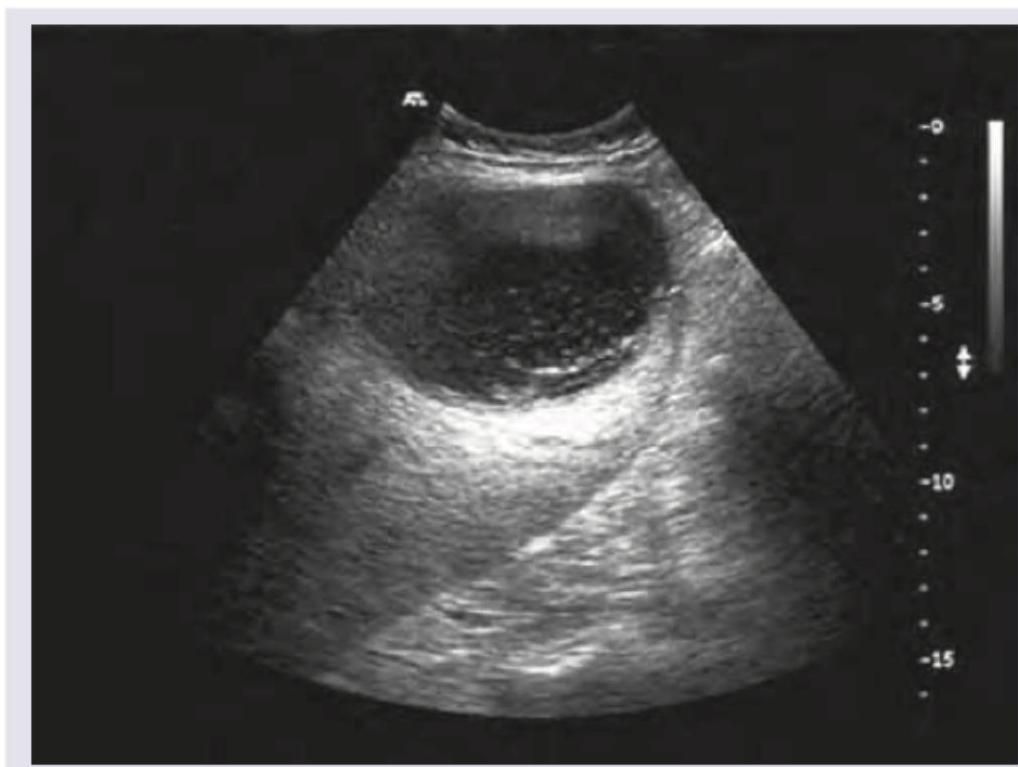
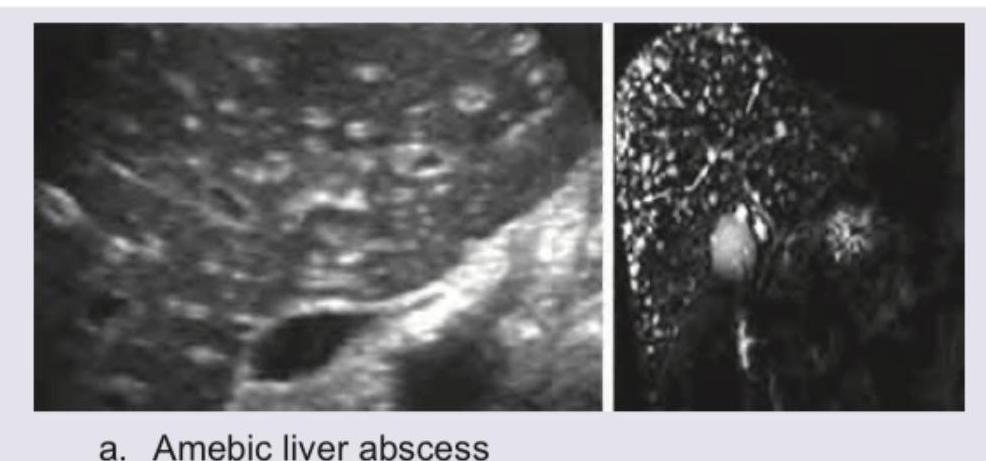
A 28-year-old female patient presents with abdominal pain, fever, night sweats, malaise, and intercostal tenderness. Past history of bloody diarrhea is present. USG liver of the patient is given. Which among the following statements is false?
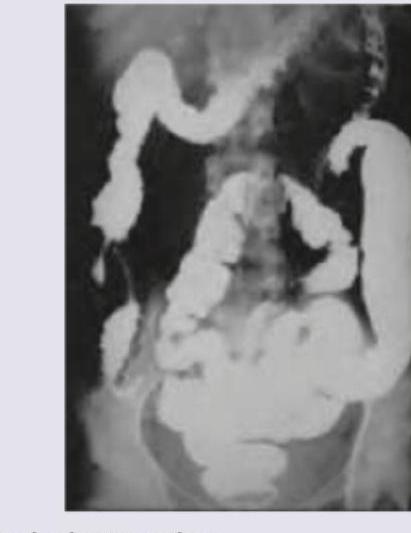
A patient presents with abdominal pain, diarrhea and weight loss. He gives past history of pulmonary TB. Barium film of the patient indicates which of the following condition?
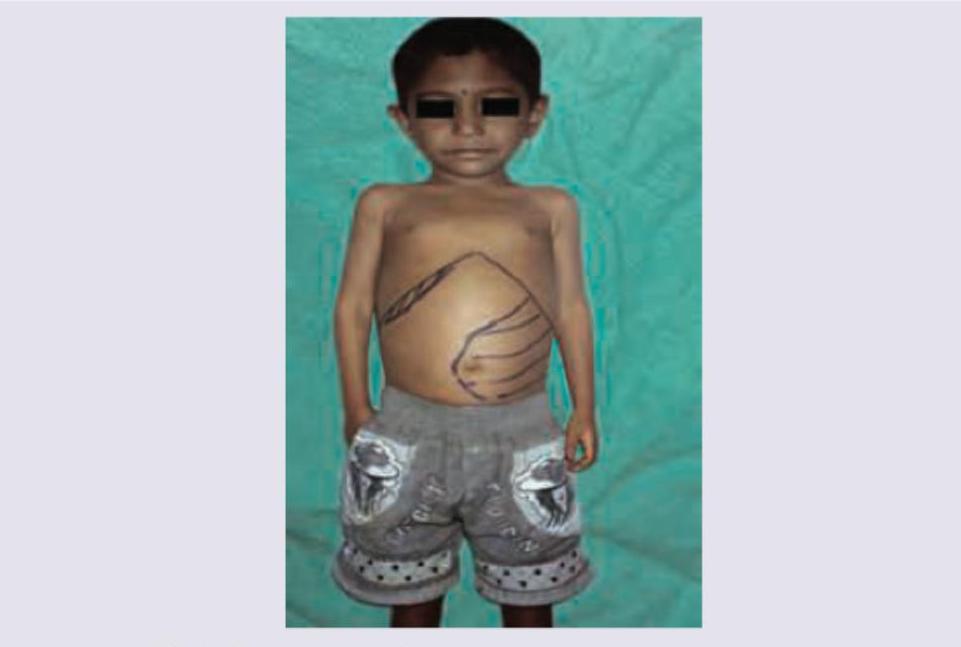
Which of the following infections in most commonly seen in this transfusion dependant child shown below?
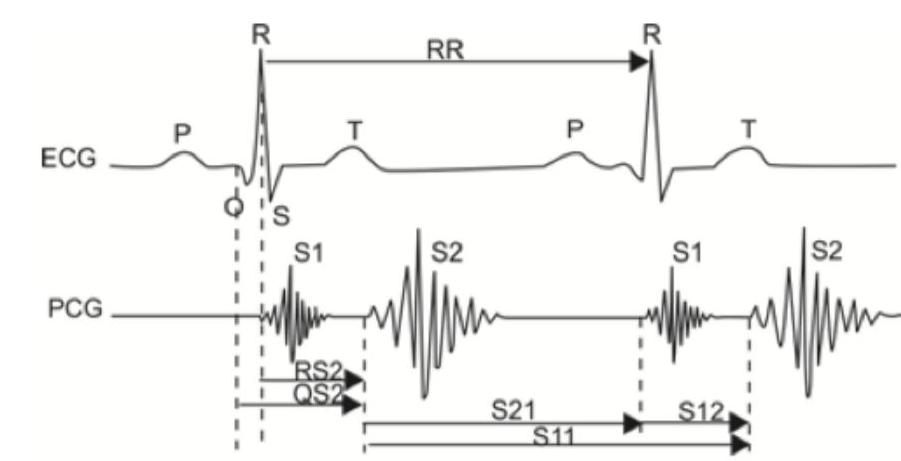
The image shows cigar-shaped soft tissue calcification/rice grain calcification in muscles, which is characteristic of cysticercosis. This finding in a patient with neurocysticercosis is categorized as:
Patients who have undergone S.O.T (Solid organ transplant) are highly susceptible to development of Kaposi sarcoma. The image shows features consistent with Kaposi Sarcoma etiologically linked with which of the following?
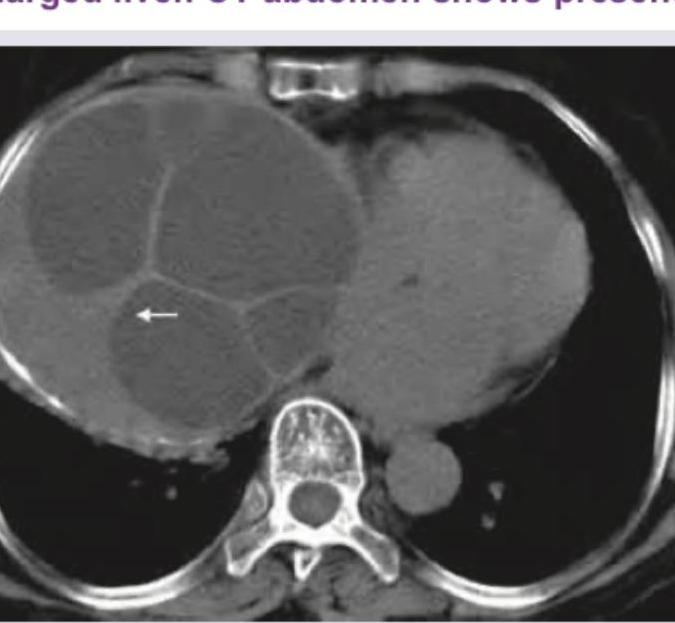
A 35-year-old shepherd presents with painless enlarged liver. CT abdomen shows presence of:
A 48-year-old intravenous drug abuser presents with vomiting, jaundice and right hypochondrium pain. USG abdomen shows presence of:
A patient of swine flu has developed severe respiratory distress. Which of the following findings confirm the diagnosis of ARDS in this patient?
Practice by Chapter
Principles of Antimicrobial Therapy
Practice Questions
Fever of Unknown Origin
Practice Questions
HIV/AIDS and Related Infections
Practice Questions
Tuberculosis and Mycobacterial Diseases
Practice Questions
Tropical and Parasitic Infections
Practice Questions
Viral Infections (Hepatitis, Herpes, etc.)
Practice Questions
Healthcare-Associated Infections
Practice Questions
Fungal Infections
Practice Questions
Sepsis and Septic Shock
Practice Questions
Infection in Immunocompromised Hosts
Practice Questions
Emerging and Re-emerging Infections
Practice Questions
Antimicrobial Resistance
Practice Questions
Vaccination Principles
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
