Infectious Diseases — MCQs

On this page
What is the drug of choice for the treatment of Taenia solium and Taenia saginata infestation?
Which of the following diseases presents with pea-soup stools?
All are useful for the management of severe Clostridium difficile infection except?
Which of the following is the most common site for syphilitic aneurysm?
What drug is used for the chemoprophylaxis of leptospirosis?
A 6-year-old boy develops symptoms of cough, fever, and malaise followed by a generalized maculopapular rash that has spread from the head downward. A clinical diagnosis of measles is made. A few days after the onset of the rash he is drowsy, lethargic, and complaining of headache. Lumbar puncture, electroencephalogram (EEG), and computerized tomography (CT) of the brain exclude other etiologies and confirm the diagnosis of encephalitis. Which of the following is the most likely delayed neurologic complication of measles virus encephalitis?
What is the most likely diagnosis in a patient from Mauritania whose foot developed these abnormalities over several years?
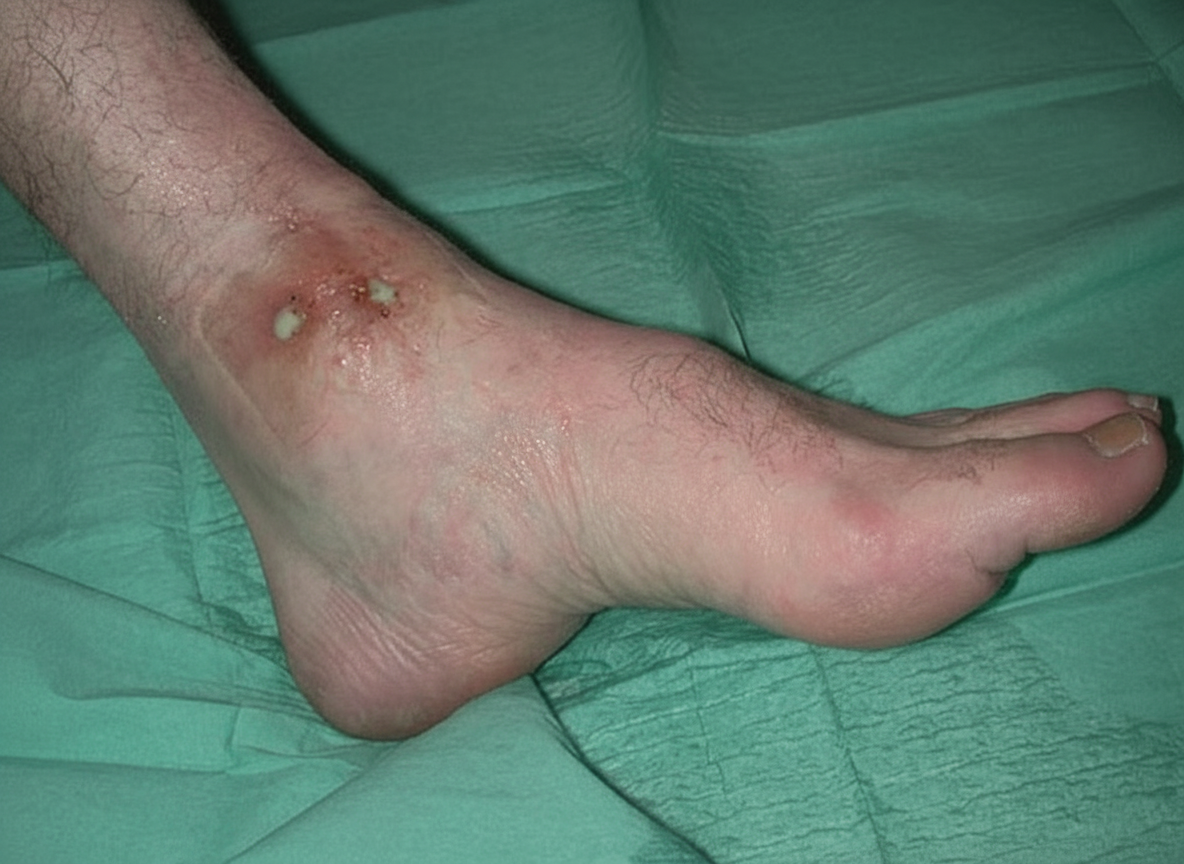
The differential diagnosis of botulism includes all of the following except?
Which of the following is an initial presentation of HIV infection?
A lung biopsy of an HIV-positive patient shows intra-nuclear basophilic inclusion bodies with a perinuclear halo. The patient's CD4 count was less than 100 at the time of diagnosis. What is the probable cause?
Practice by Chapter
Principles of Antimicrobial Therapy
Practice Questions
Fever of Unknown Origin
Practice Questions
HIV/AIDS and Related Infections
Practice Questions
Tuberculosis and Mycobacterial Diseases
Practice Questions
Tropical and Parasitic Infections
Practice Questions
Viral Infections (Hepatitis, Herpes, etc.)
Practice Questions
Healthcare-Associated Infections
Practice Questions
Fungal Infections
Practice Questions
Sepsis and Septic Shock
Practice Questions
Infection in Immunocompromised Hosts
Practice Questions
Emerging and Re-emerging Infections
Practice Questions
Antimicrobial Resistance
Practice Questions
Vaccination Principles
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
