Infectious Diseases — MCQs

On this page
Waterhouse-Friderichsen syndrome is caused by which organism?
A 19-year-old male presents with a 1-week history of malaise and anorexia followed by fever and sore throat. On physical examination, the throat is inflamed without exudate, and there are a few palatal petechiae. Cervical adenopathy is present. The liver is percussed at 12 cm and the spleen is palpable. Throat cultures are negative for group A streptococci, and peripheral blood smears show atypical lymphocytosis. Laboratory findings include: Hb: 12 g/dL, Reticulocytes: 4%, WBC: 14,000/uL with 60% Lymphocytes, Total Bilirubin: 2.0 mg/dL, LDH: 260 IU/L, AST: 40 U/L, and ALT: 35 U/L. What is the next best investigation?
Which of the following is NOT a characteristic feature of Kala-azar?
Occurrence of diplopia, dysphagia, dysarthria, blurring of vision, and muscle weakness could be due to which of the following?
A 35-year-old woman presents with a 2-day history of burning on urination. Urinalysis shows marked positivity for leukocyte esterase but no reactivity for nitrite. Urine culture grows a large number of organisms. Which of the following bacteria is most likely responsible for this patient's infection?
Pulmonary tuberculosis is more common in the following associated diseases, except:
A 20-year-old woman presents with a 2-week history of fever, malaise, and brown-colored urine. She recently visited Mexico. Physical examination reveals jaundice, mild hepatomegaly, and tenderness in the right upper quadrant. The serum bilirubin is 7.8 mg/dL, with 60% in the conjugated form. Serum levels of AST and ALT are markedly elevated (400 and 392 U/L, respectively). Serum albumin and immunoglobulin levels are normal. Serum IgM anti-hepatitis A virus (anti-HAV) is positive. IgG anti-hepatitis B surface antigen (anti-HBsAg) antibodies are positive. Anti-hepatitis C virus antibodies are negative. What is the most likely diagnosis?
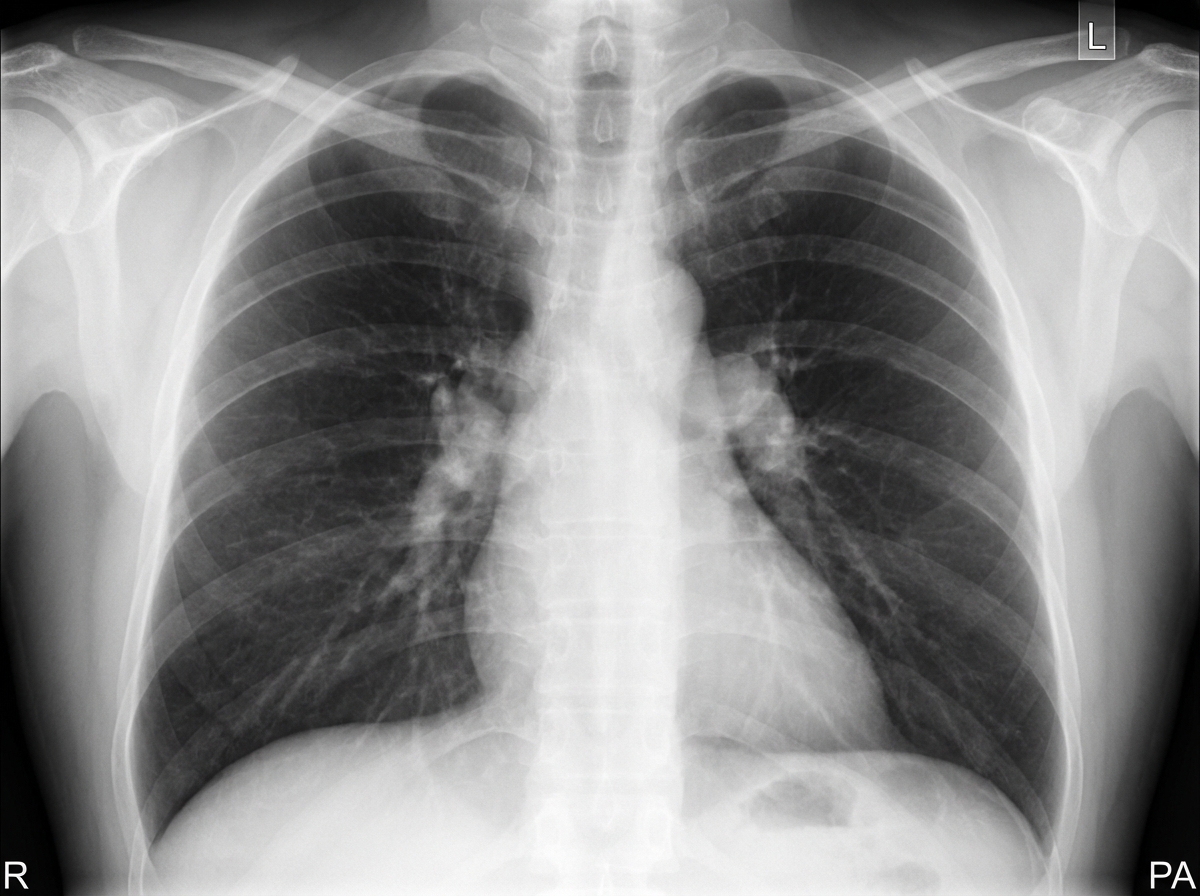
What is the most likely diagnosis in this patient with cough?
What is the treatment of choice for a patient with meningococcal meningitis who is allergic to penicillin?
The definition of FUO (fever of unknown origin) requires fever lasting for more than how many weeks?
Practice by Chapter
Principles of Antimicrobial Therapy
Practice Questions
Fever of Unknown Origin
Practice Questions
HIV/AIDS and Related Infections
Practice Questions
Tuberculosis and Mycobacterial Diseases
Practice Questions
Tropical and Parasitic Infections
Practice Questions
Viral Infections (Hepatitis, Herpes, etc.)
Practice Questions
Healthcare-Associated Infections
Practice Questions
Fungal Infections
Practice Questions
Sepsis and Septic Shock
Practice Questions
Infection in Immunocompromised Hosts
Practice Questions
Emerging and Re-emerging Infections
Practice Questions
Antimicrobial Resistance
Practice Questions
Vaccination Principles
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
