Infectious Diseases — MCQs

On this page
What is the drug of choice for cytomegalovirus retinitis in HIV patients?
Which of the following conditions is characterized by a double rise of temperature within a 24-hour period?
Kala azar is which of the following types of leishmaniasis?
Seizures may be the presenting feature in all of the following, except?
Kernig's sign is seen in which of the following conditions?
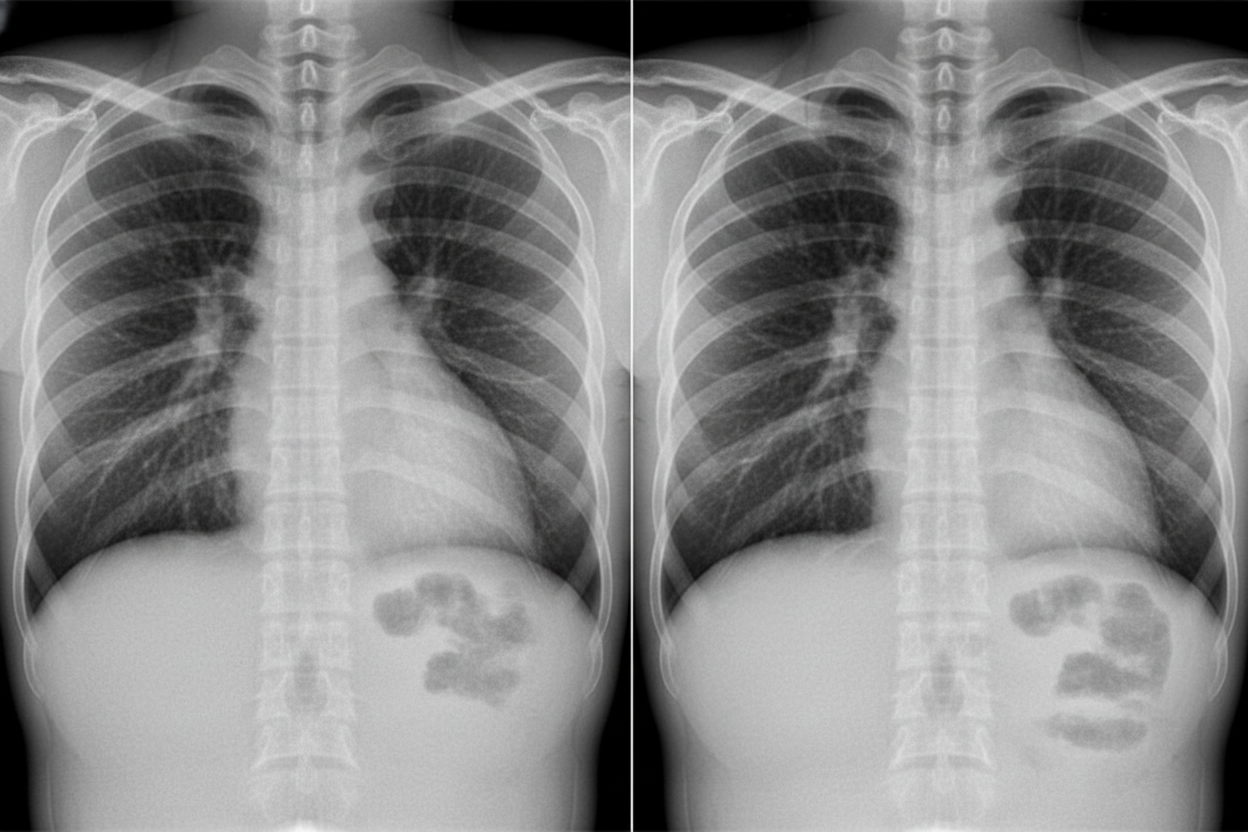
A patient presents with acute onset high-grade fever, chills, productive cough with rusty-colored sputum, and pleuritic chest pain. The chest X-ray is shown below. What is the most likely diagnosis?
What represents a medical emergency in an asplenic patient?
The oral lesion called mucous patches is usually multiple, grayish white plaques associated with what?
Which of the following pneumonias is caused by contaminated air conditioners?
Mulberry molars are characteristic features of which condition?
Practice by Chapter
Principles of Antimicrobial Therapy
Practice Questions
Fever of Unknown Origin
Practice Questions
HIV/AIDS and Related Infections
Practice Questions
Tuberculosis and Mycobacterial Diseases
Practice Questions
Tropical and Parasitic Infections
Practice Questions
Viral Infections (Hepatitis, Herpes, etc.)
Practice Questions
Healthcare-Associated Infections
Practice Questions
Fungal Infections
Practice Questions
Sepsis and Septic Shock
Practice Questions
Infection in Immunocompromised Hosts
Practice Questions
Emerging and Re-emerging Infections
Practice Questions
Antimicrobial Resistance
Practice Questions
Vaccination Principles
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
