Infectious Diseases — MCQs

On this page
What is the highest relative risk of developing active tuberculosis in patients already infected with Mycobacterium tuberculosis?
Which cells does the Human Immunodeficiency Virus (HIV) primarily infect?
In a patient with tuberculosis and AIDS, what is the typical appearance on a chest X-ray?
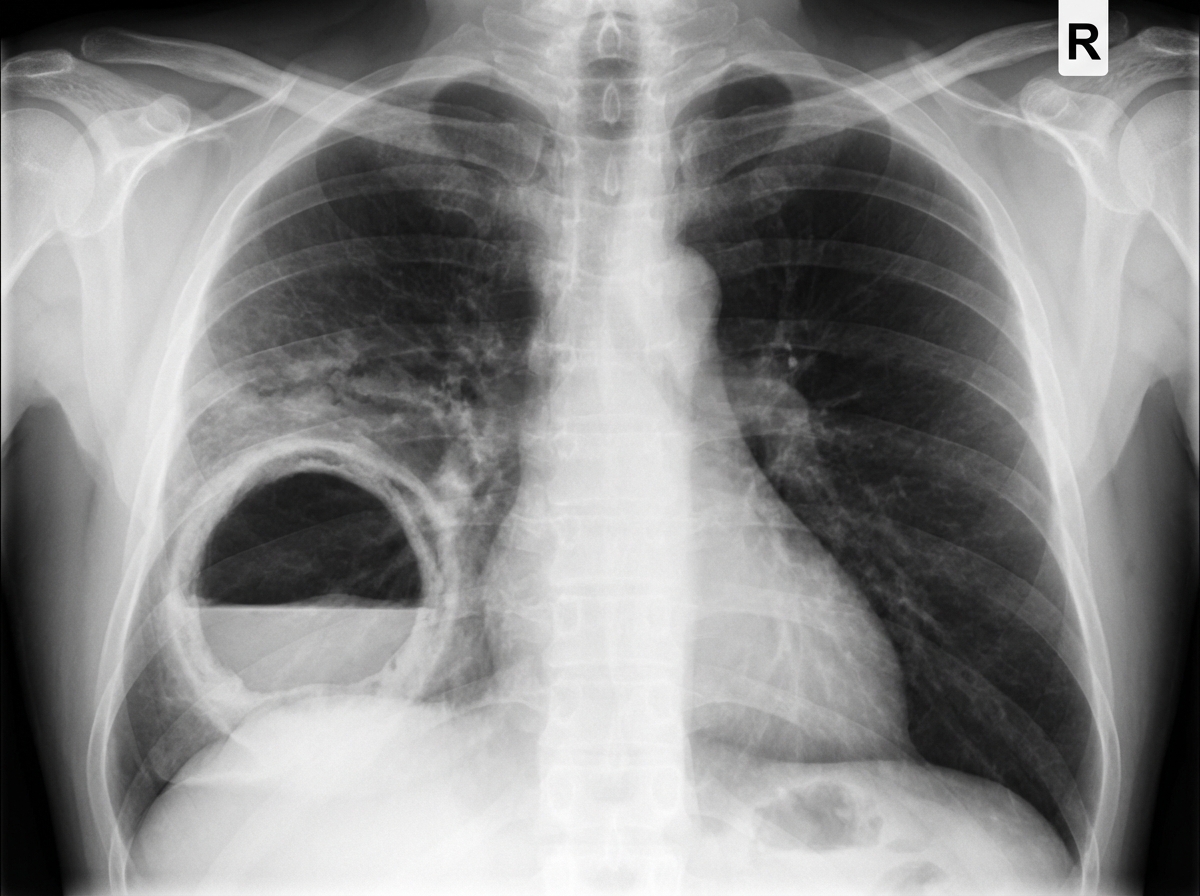
A 40-year-old man with a history of substance abuse and HIV infection presents with fever, weight loss, production of foul-smelling sputum, and shortness of breath for 2 weeks. Physical examination reveals tachypnea and clubbing of his digits. Lung auscultation demonstrates diffuse rhonchi and an area of egophony with whispering pectoriloquy in the right posterior chest. Arterial blood gases show a PaO2 of 59 mm Hg on room air. A chest X-ray is available. What is the most likely diagnosis?
A 36-year-old woman recently treated for leukemia is admitted to the hospital with malaise, chills, and high fever. Gram stain of blood reveals the presence of gram-negative bacilli. The initial diagnosis is bacteremia, and parenteral antibiotics are indicated. The patient's record reveals a severe urticarial rash, hypotension, and respiratory difficulty after oral penicillin V about 6 months ago. What is the most appropriate antibiotic to administer?
Kaposi sarcoma associated with the gut may be seen in which of the following conditions?
A 30-year-old male presents with a cough and fever of six weeks' duration. Sputum smears are negative, and chest X-ray shows no significant findings. Given a high clinical suspicion for tuberculosis, what is the next appropriate management step?
Which of the following is NOT part of the standard treatment for human brucellosis?
What is the most characteristic clinical finding in a patient with tetanus?
Which of the following is true about tuberculosis?
Practice by Chapter
Principles of Antimicrobial Therapy
Practice Questions
Fever of Unknown Origin
Practice Questions
HIV/AIDS and Related Infections
Practice Questions
Tuberculosis and Mycobacterial Diseases
Practice Questions
Tropical and Parasitic Infections
Practice Questions
Viral Infections (Hepatitis, Herpes, etc.)
Practice Questions
Healthcare-Associated Infections
Practice Questions
Fungal Infections
Practice Questions
Sepsis and Septic Shock
Practice Questions
Infection in Immunocompromised Hosts
Practice Questions
Emerging and Re-emerging Infections
Practice Questions
Antimicrobial Resistance
Practice Questions
Vaccination Principles
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
