Infectious Diseases — MCQs

On this page
Which of the following infections does NOT typically cause acute hepatic and renal failure?
A person presents with difficulty of breathing and a CD-4 count of 200. What is the most probable diagnosis?
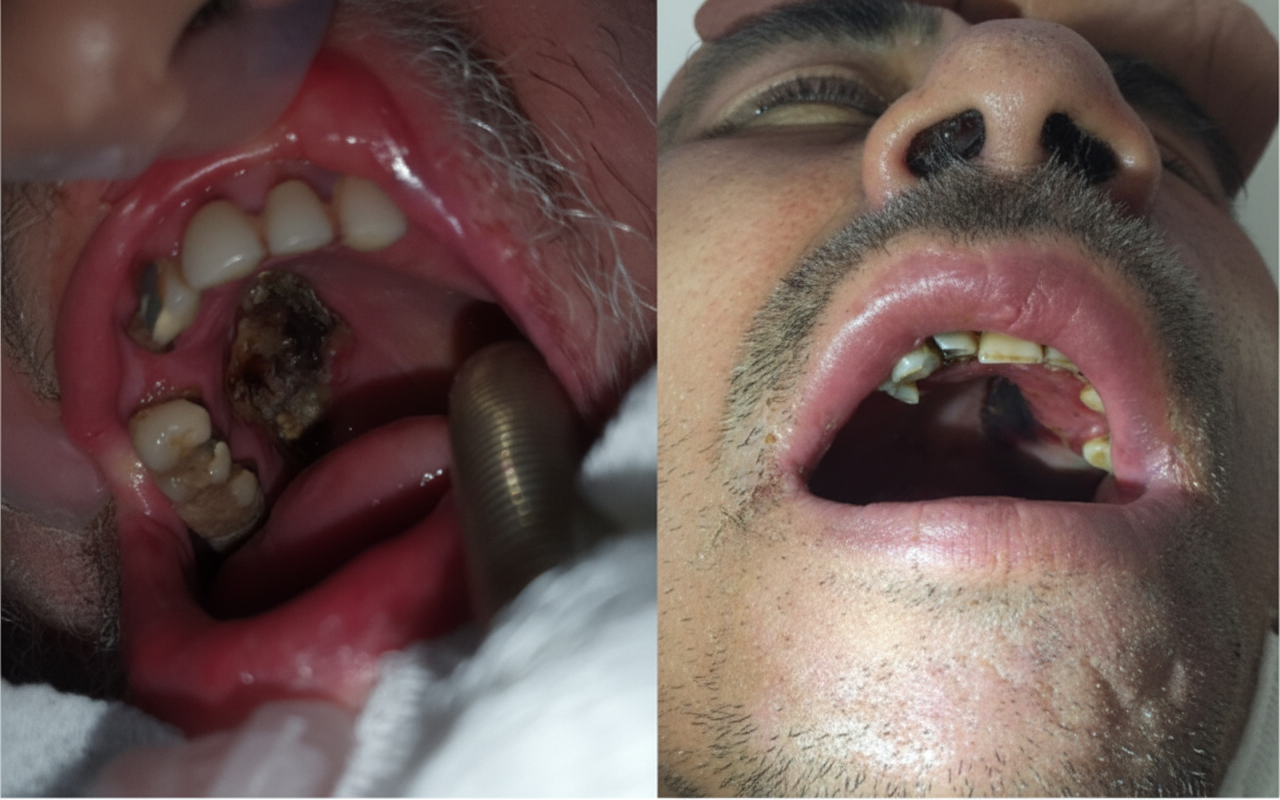
Following extraction of an upper central incisor, a patient develops ophthalmoplegia, meningitis, and lateral rectus paralysis. What is the most likely diagnosis?
All are risk factors for antituberculosis treatment related hepatotoxicity, EXCEPT?
What is the most common hematologic finding associated with pulmonary tuberculosis?
A 35-year-old man developed a lesion on his chest during treatment for a respiratory tract infection. What is the diagnosis?
Which of the following is not used in post-exposure prophylaxis for HIV?
Which of the following drugs is NOT used in the treatment of candidiasis?
Which one of the following is typically associated with the given clinical finding?
What is the common presenting symptom of Pneumocystis jirovecii pneumonia?
Practice by Chapter
Principles of Antimicrobial Therapy
Practice Questions
Fever of Unknown Origin
Practice Questions
HIV/AIDS and Related Infections
Practice Questions
Tuberculosis and Mycobacterial Diseases
Practice Questions
Tropical and Parasitic Infections
Practice Questions
Viral Infections (Hepatitis, Herpes, etc.)
Practice Questions
Healthcare-Associated Infections
Practice Questions
Fungal Infections
Practice Questions
Sepsis and Septic Shock
Practice Questions
Infection in Immunocompromised Hosts
Practice Questions
Emerging and Re-emerging Infections
Practice Questions
Antimicrobial Resistance
Practice Questions
Vaccination Principles
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
