Infectious Diseases — MCQs

On this page
What is the most common pulmonary manifestation in AIDS?
Which of the following laboratory markers characterizes the recumbent stage of Hepatitis B?
Fever, clubbing, and Osler's nodes are characteristic findings in which of the following conditions?
Which of the following diseases does not typically present as shock?
Genital herpes is caused by which virus?
Which of the following statements is NOT true about Legionnaire's pneumonia?
A young patient presented with fever (100 extdegree F), nausea, and vomiting. The patient also complained of vague abdominal discomfort. On general examination, icterus and hepatic tenderness were present. A family member had similar symptoms and was diagnosed with hepatitis E. Which of the following is the most likely route of transmission for the hepatitis E virus in this patient?
A 35-year-old male patient with a known case of HIV on Antiretroviral Therapy complains of fever, dyspnea, dry cough, and weight loss for the past 3 months. The chest X-ray of the patient is as below. What is your diagnosis?
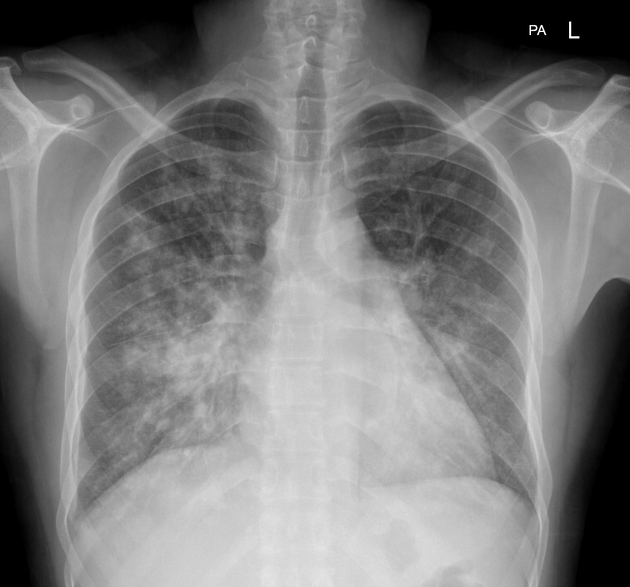
All the following are used in the treatment of Pneumocystis jirovecii pneumonia except?
A 22-year-old male military recruit complains of a headache and stiff neck. He is examined, blood is drawn, and a lumbar puncture is performed. The glucose in the CSF is 100 mg/dL and the serum glucose is 120 mg/dL. The CSF shows 3 lymphocytes and 0 neutrophils/microliter. Which of the following conclusions concerning the interpretation of these findings is most accurate?
Practice by Chapter
Principles of Antimicrobial Therapy
Practice Questions
Fever of Unknown Origin
Practice Questions
HIV/AIDS and Related Infections
Practice Questions
Tuberculosis and Mycobacterial Diseases
Practice Questions
Tropical and Parasitic Infections
Practice Questions
Viral Infections (Hepatitis, Herpes, etc.)
Practice Questions
Healthcare-Associated Infections
Practice Questions
Fungal Infections
Practice Questions
Sepsis and Septic Shock
Practice Questions
Infection in Immunocompromised Hosts
Practice Questions
Emerging and Re-emerging Infections
Practice Questions
Antimicrobial Resistance
Practice Questions
Vaccination Principles
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
