Infectious Diseases — MCQs

On this page
What is the causative agent responsible for the chronic carrier state in liver disease?
A nurse has been found to be seropositive for both HbsAg and HBeAg. She is suffering from which of the following conditions?
A 19-year-old male tests positive for hepatitis C infection. He was arrested twice for stealing and belongs to a gang of friends. Which of the following is the most likely method of transmission?
Treatment with what antibiotic is most likely to have resulted in this patient's skin changes?
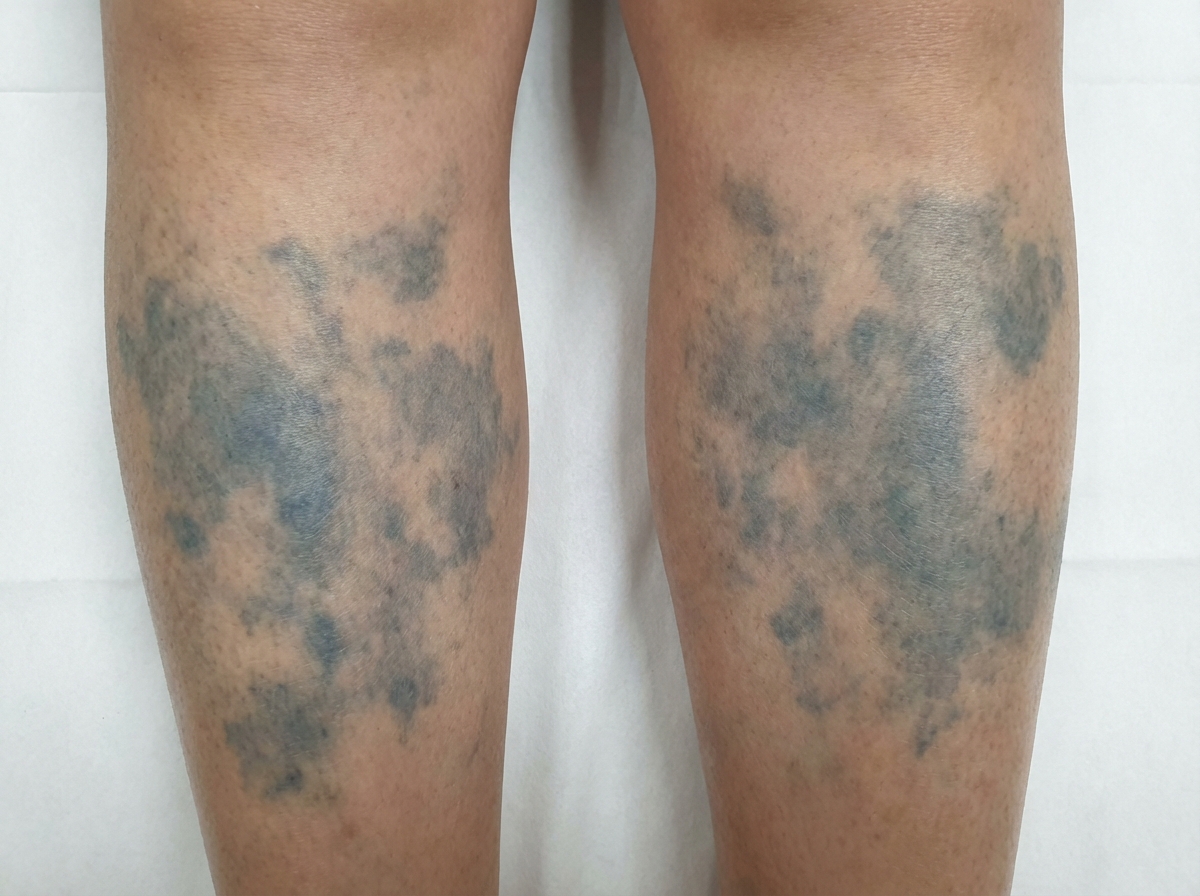
A 59-year-old man undergoes coronary bypass surgery and receives vancomycin prophylactically for 24 hours. On the ninth postoperative day, he develops a fever of 39.8°C (103°F) with a heart rate of 115 beats/min and a blood pressure of 105/65 mm Hg. The surgical site is healing well with no redness or discharge. His white blood cell count is 14,000/mm³ and urinalysis reveals many white blood cells per high-power field. Blood and urine cultures grow a non-lactose-fermenting oxidase-positive gram-negative rod. Which of the following antibiotics is most appropriate to treat this infection?
Inflammation of nerve is seen in which of the following conditions?
A farmer who handles goats and sheep is presenting with fever, muscle and joint pain, and rash. What is the most likely diagnosis?
Which of the following statements is true about measles?
What is the best treatment for a diabetic patient with the condition described below?
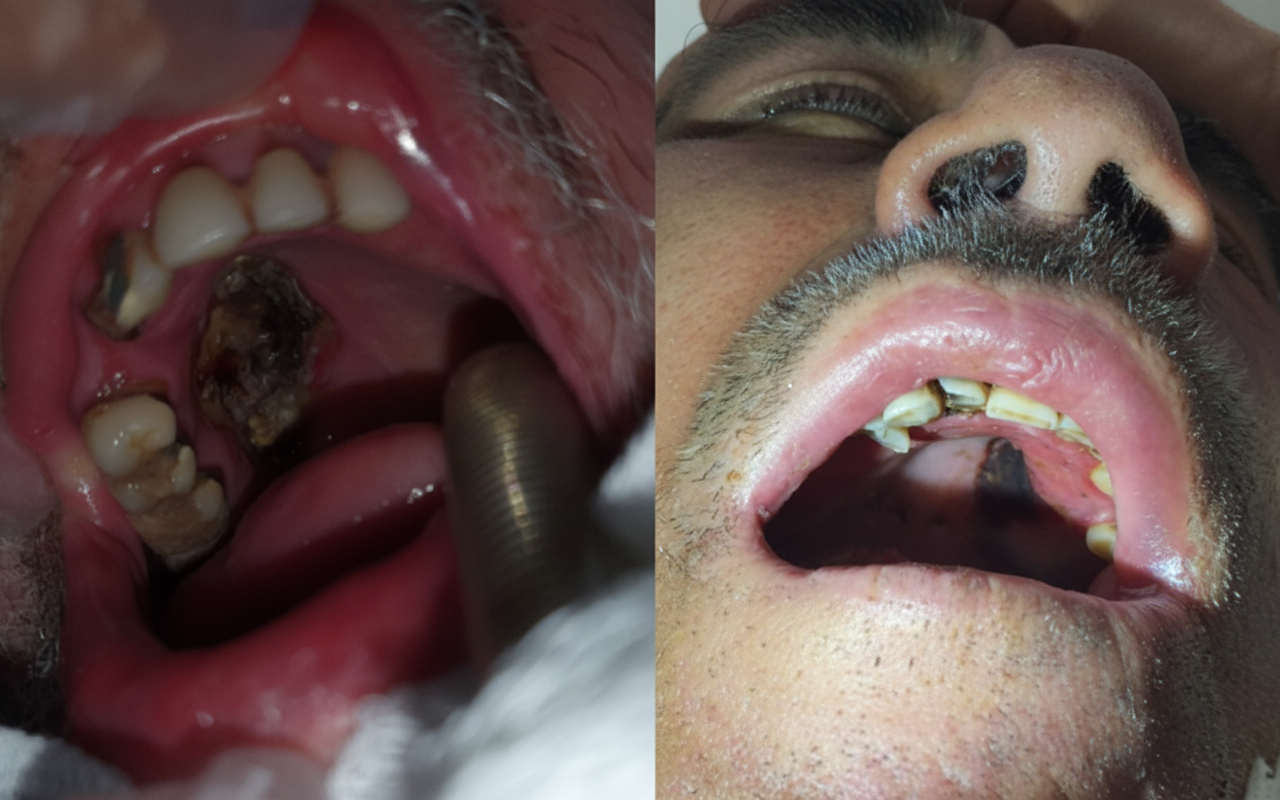
What is the drug of choice in Bacteroides infections?
Practice by Chapter
Principles of Antimicrobial Therapy
Practice Questions
Fever of Unknown Origin
Practice Questions
HIV/AIDS and Related Infections
Practice Questions
Tuberculosis and Mycobacterial Diseases
Practice Questions
Tropical and Parasitic Infections
Practice Questions
Viral Infections (Hepatitis, Herpes, etc.)
Practice Questions
Healthcare-Associated Infections
Practice Questions
Fungal Infections
Practice Questions
Sepsis and Septic Shock
Practice Questions
Infection in Immunocompromised Hosts
Practice Questions
Emerging and Re-emerging Infections
Practice Questions
Antimicrobial Resistance
Practice Questions
Vaccination Principles
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
