Infectious Diseases — MCQs

On this page
What is the drug of choice for the treatment of neurosyphilis?
A girl complained of abdominal pain with the passage of foul-smelling stool that does not wash away easily. There is a history of swimming in contaminated water. What is the likely causative organism?
All of the following are associated with primary tuberculosis EXCEPT:
The appearance of this foot is most consistent with which one of the following diagnoses?
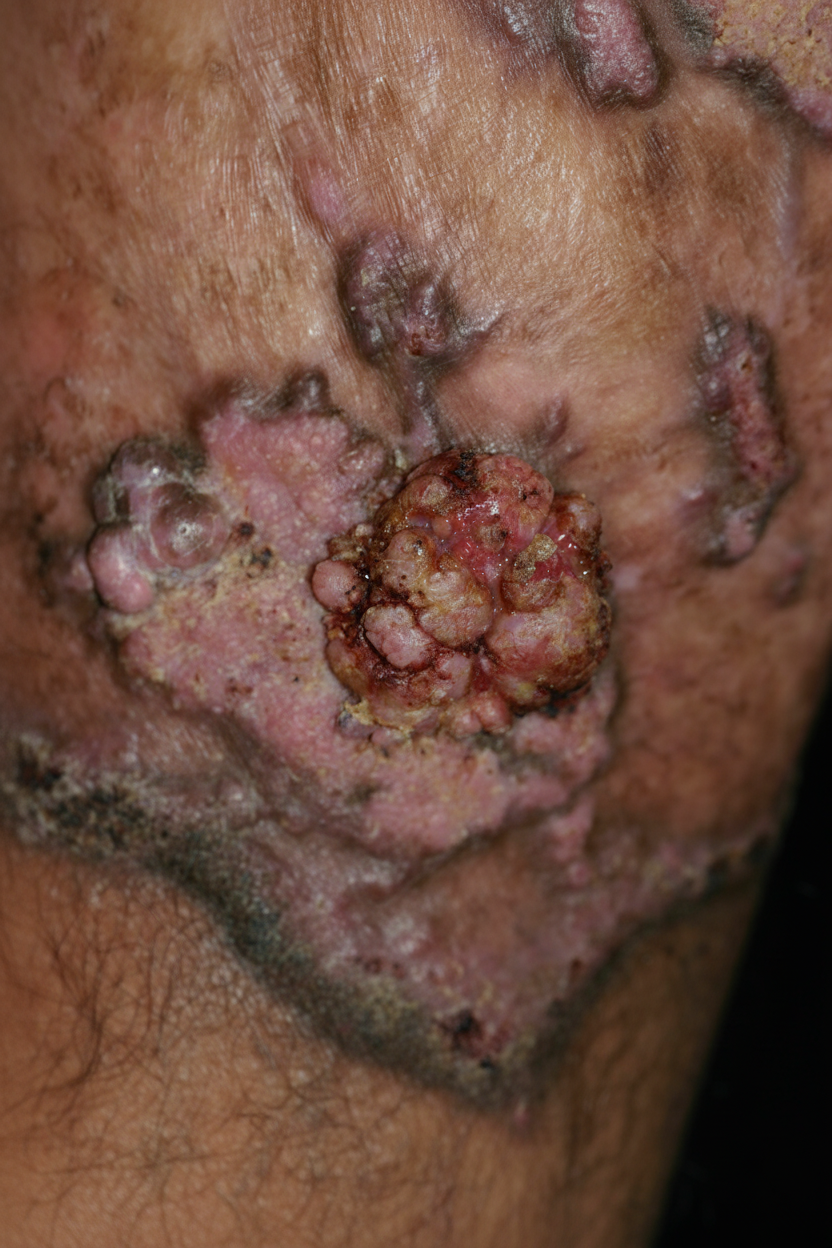
Which statement is FALSE regarding Tuberculosis in an HIV-positive individual?
A patient with HIV and a CD4 count of 160 cells/µL presents with fever, cough, and shortness of breath for 3 weeks. Chest X-ray and silver staining of bronchoalveolar lavage are shown. What is the drug of choice for the causative organism?
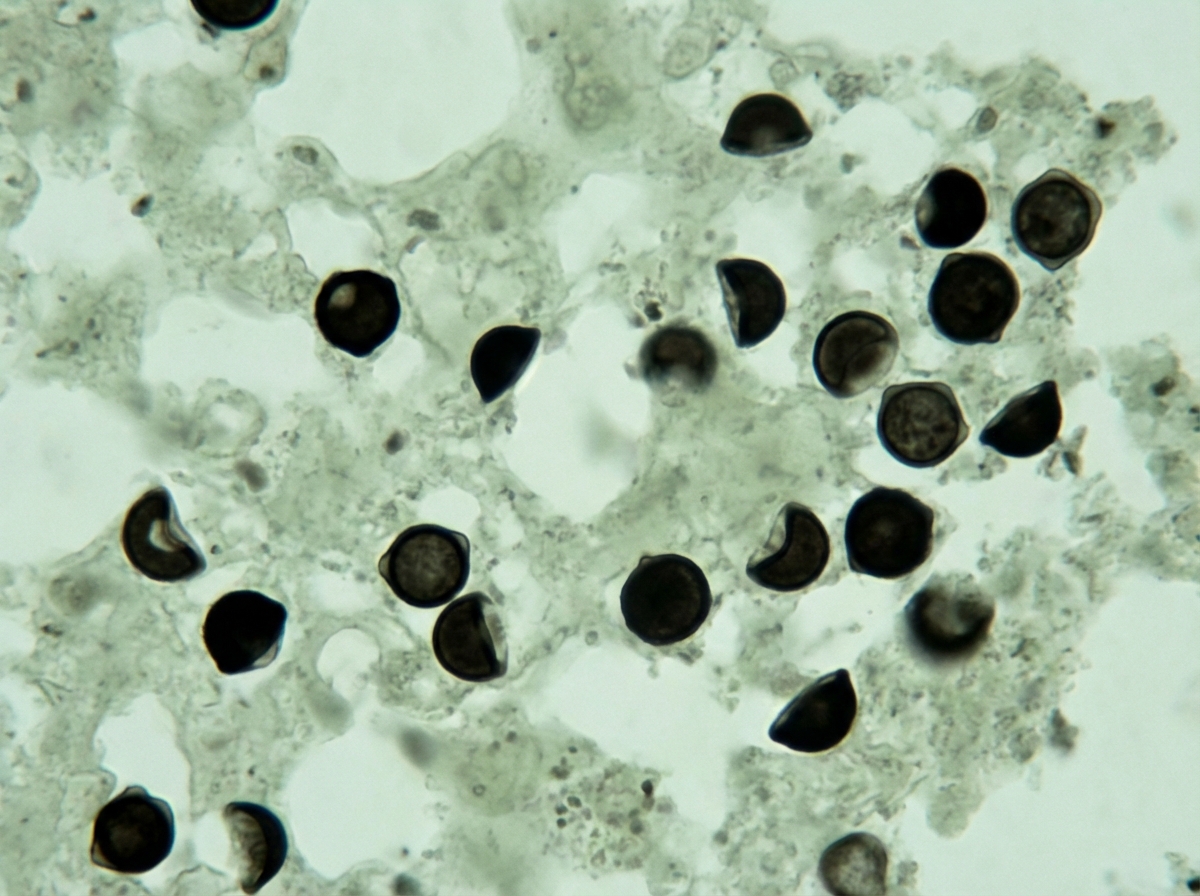
Sardonic grin is associated with which condition?
In a neutropenic patient, which of the following would be most commonly encountered as a cause of bacterial meningitis and brain abscess?
Salmonellosis is most commonly associated with which of the following conditions?
Leukopenia is characteristic of which of the following conditions?
Practice by Chapter
Principles of Antimicrobial Therapy
Practice Questions
Fever of Unknown Origin
Practice Questions
HIV/AIDS and Related Infections
Practice Questions
Tuberculosis and Mycobacterial Diseases
Practice Questions
Tropical and Parasitic Infections
Practice Questions
Viral Infections (Hepatitis, Herpes, etc.)
Practice Questions
Healthcare-Associated Infections
Practice Questions
Fungal Infections
Practice Questions
Sepsis and Septic Shock
Practice Questions
Infection in Immunocompromised Hosts
Practice Questions
Emerging and Re-emerging Infections
Practice Questions
Antimicrobial Resistance
Practice Questions
Vaccination Principles
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
