Infectious Diseases — MCQs

On this page
What is the standard treatment therapy for Pneumocystis jirovecii pneumonia (PCP)?
A 30-year-old male presented with complaints of sudden onset of fever, chills, severe headache, backache, and retro-orbital pain for 3 days. On the 3rd day, a rash appeared on the face, thorax, and flexor surfaces. The rash was macular and confluent. The tourniquet test was positive. Lab findings revealed a low platelet count, low WBC count, increased SGOT and SGPT levels, and a hematocrit increase by >20%. The above disease is transmitted by which of the following vectors?
Which of the following is NOT a cause of community-acquired pneumonia?
Which of the following causes tropical spastic paraplegia?
Infection with which organism during pregnancy can cause congenital hydrocephalus?
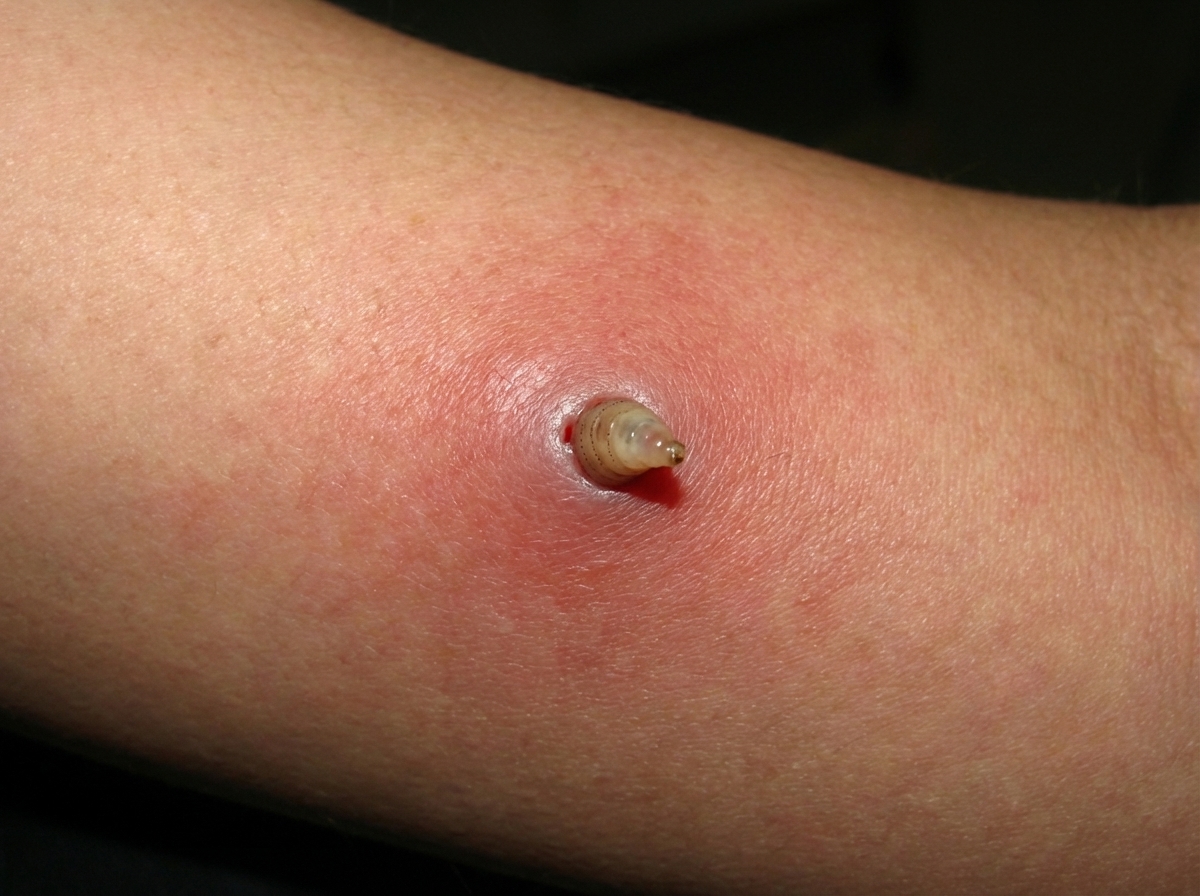
A 65-year-old man presented with skin lesions six weeks after returning from a vacation in Belize, which included time spent at the beach and in the rainforest. What is the diagnosis?
What is the most common route of transmission for hepatitis C?
Thermophilus actinomycetes is NOT a causative agent for which of the following conditions?
Rasmussen's aneurysm is seen in which of the following arteries?
A 38-year-old male presents with swelling in the inguinal region. On examination, inguinal nodes are enlarged along with multiple discharging sinuses from the enlarged lymph nodes. What is the most probable diagnosis?
Practice by Chapter
Principles of Antimicrobial Therapy
Practice Questions
Fever of Unknown Origin
Practice Questions
HIV/AIDS and Related Infections
Practice Questions
Tuberculosis and Mycobacterial Diseases
Practice Questions
Tropical and Parasitic Infections
Practice Questions
Viral Infections (Hepatitis, Herpes, etc.)
Practice Questions
Healthcare-Associated Infections
Practice Questions
Fungal Infections
Practice Questions
Sepsis and Septic Shock
Practice Questions
Infection in Immunocompromised Hosts
Practice Questions
Emerging and Re-emerging Infections
Practice Questions
Antimicrobial Resistance
Practice Questions
Vaccination Principles
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
