Infectious Diseases — MCQs

On this page
Which is the most common manifestation of recurrent HSVl infection:
All of the following cause hemolytic uremic syndrome except
A 35-year-old patient presents with white plaques on the tongue and inner cheeks, which can be scraped off, leaving a red base. The patient also complains of a sore throat. What is the most appropriate management for this condition?
Rose spot is associated with
Dharmendra's index and Jopling's classification deals with -
True about diphtheria is -
The most common cause of menstrual toxic shock syndrome is -
Most common site of gastrointestinal TB:
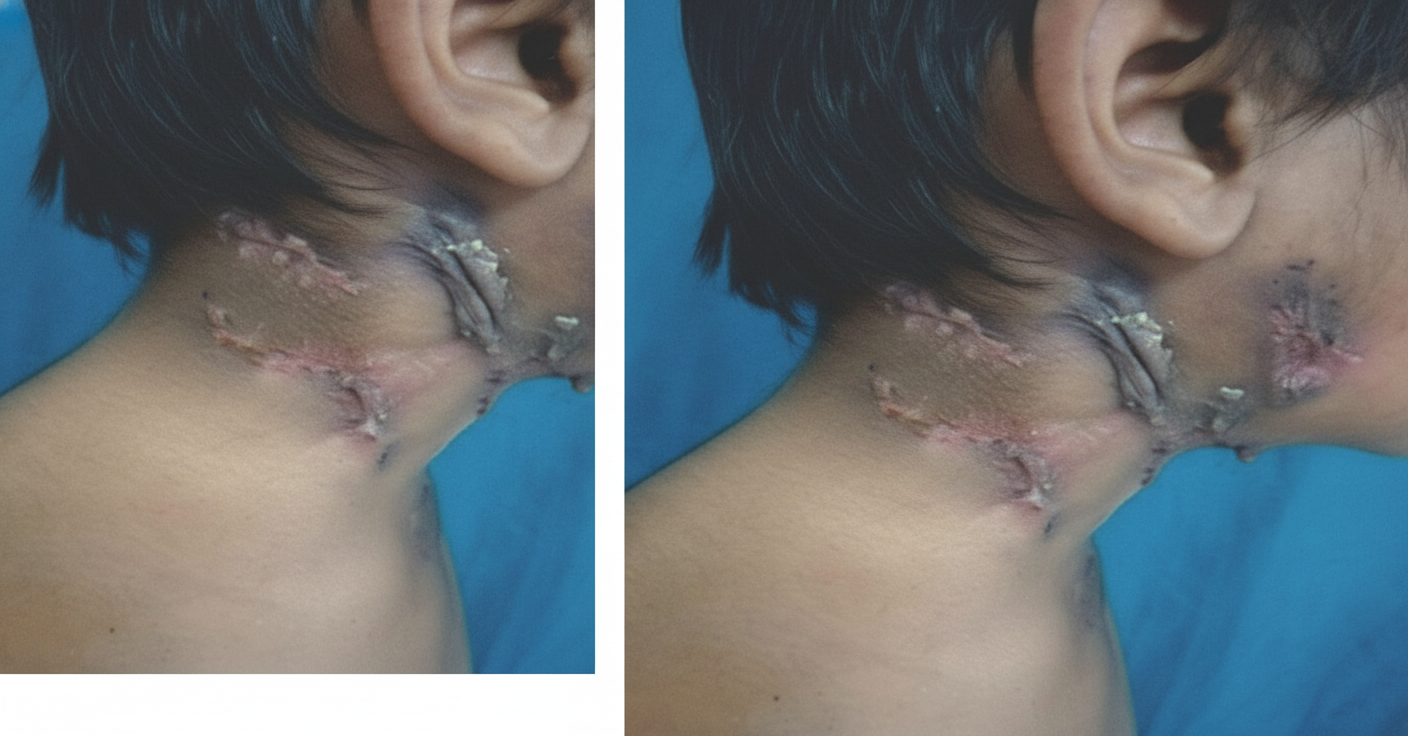
A lesion was seen on the face of a 42 year old patient as shown below. Which of the following would be ideal management for this condition?
HIV patient presented with diarrhea. On stool examination, acid-fast organisms (Isospora belli) were seen. What is the drug of choice in this patient?
Practice by Chapter
Principles of Antimicrobial Therapy
Practice Questions
Fever of Unknown Origin
Practice Questions
HIV/AIDS and Related Infections
Practice Questions
Tuberculosis and Mycobacterial Diseases
Practice Questions
Tropical and Parasitic Infections
Practice Questions
Viral Infections (Hepatitis, Herpes, etc.)
Practice Questions
Healthcare-Associated Infections
Practice Questions
Fungal Infections
Practice Questions
Sepsis and Septic Shock
Practice Questions
Infection in Immunocompromised Hosts
Practice Questions
Emerging and Re-emerging Infections
Practice Questions
Antimicrobial Resistance
Practice Questions
Vaccination Principles
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
