Critical Care — MCQs

On this page
Which of the following is not a component of qSOFA score?
Which of the following is seen in all kinds of shock?
Which of the following is the class of shock where urine output is first decreased?
A 20-year-old female diagnosed with septic shock presents with a blood pressure of 58/30 mmHg. After receiving 3 liters of crystalloid fluid, her mean arterial pressure (MAP) remains 58 mmHg. What is the next best step in management?
A 56-year-old diabetic male presents with a complicated urinary tract infection and is found to be hypotensive. His blood pressure does not respond to intravenous fluids. Which of the following is the most appropriate antibiotic to manage his condition?
In a septic shock patient who remains hypotensive despite adequate fluid resuscitation, what would be the next drug of choice?
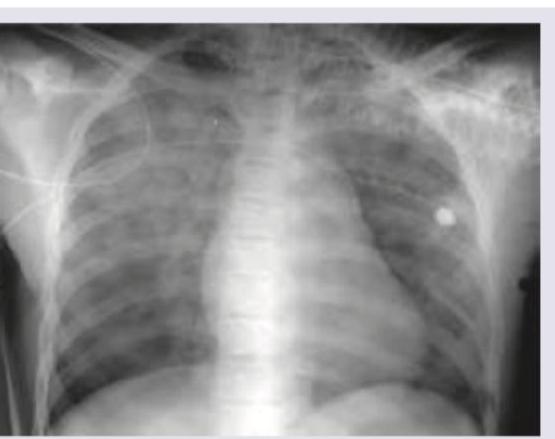
A 30-year-old patient on respiratory support has a SpO2 of 80% and bilateral crepitations in all lung fields. CXR shows presence of:
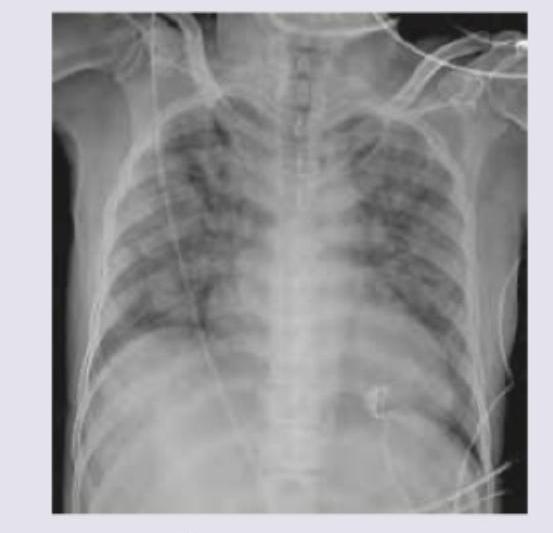
A patient in ICU was given blood transfusion. 3 hours later SpO2 is reduced to 75% with respiratory difficulty. CVP is 15 cm water and PCWP is 25 mm Hg . CXR is shown below. What is the diagnosis?
Which of the following are components of SOFA scoring system? I. PaO_2 / FiO_2 ratio II. Mean arterial pressure III. Glasgow coma scale IV. Prothrombin Time with INR Select the correct answer using the code given below :
The best measure of organ perfusion and the best monitor of adequacy of shock therapy is
Practice by Chapter
Shock Syndromes and Management
Practice Questions
Acute Respiratory Distress Syndrome
Practice Questions
Mechanical Ventilation Principles
Practice Questions
Hemodynamic Monitoring
Practice Questions
Nutrition in Critical Illness
Practice Questions
Sedation and Analgesia in ICU
Practice Questions
Multi-organ Dysfunction Syndrome
Practice Questions
Acid-Base and Electrolyte Disturbances
Practice Questions
Toxicologic Emergencies
Practice Questions
Neurological Emergencies in ICU
Practice Questions
Renal Replacement Therapy
Practice Questions
End-of-Life Care in ICU
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
