Clinical Manifestations and Presentation of Diseases — MCQs

On this page
What is the level of serum potassium at which paralysis is a possible complication of hypokalemia?
Which of the following statements about syncope is false?
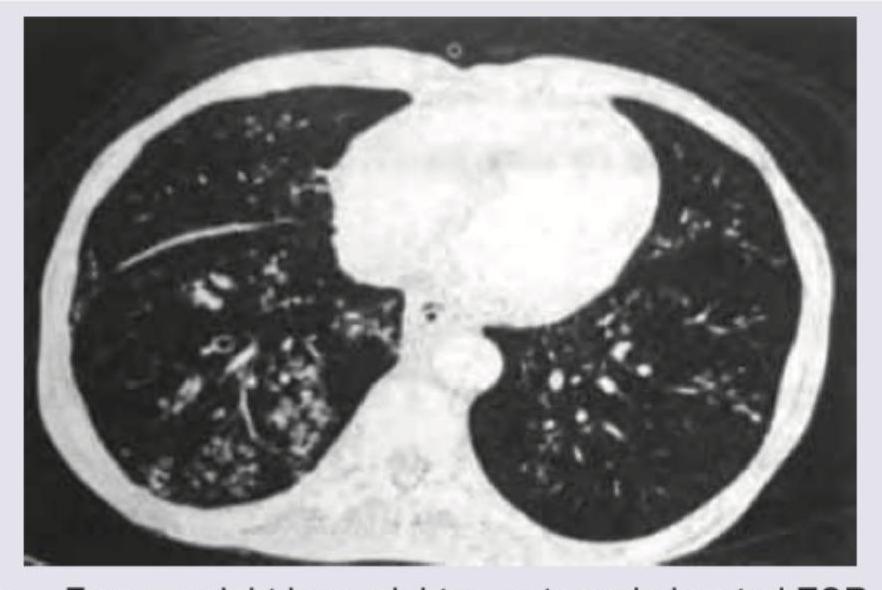
What is the most likely diagnosis in this 50-year-old woman?
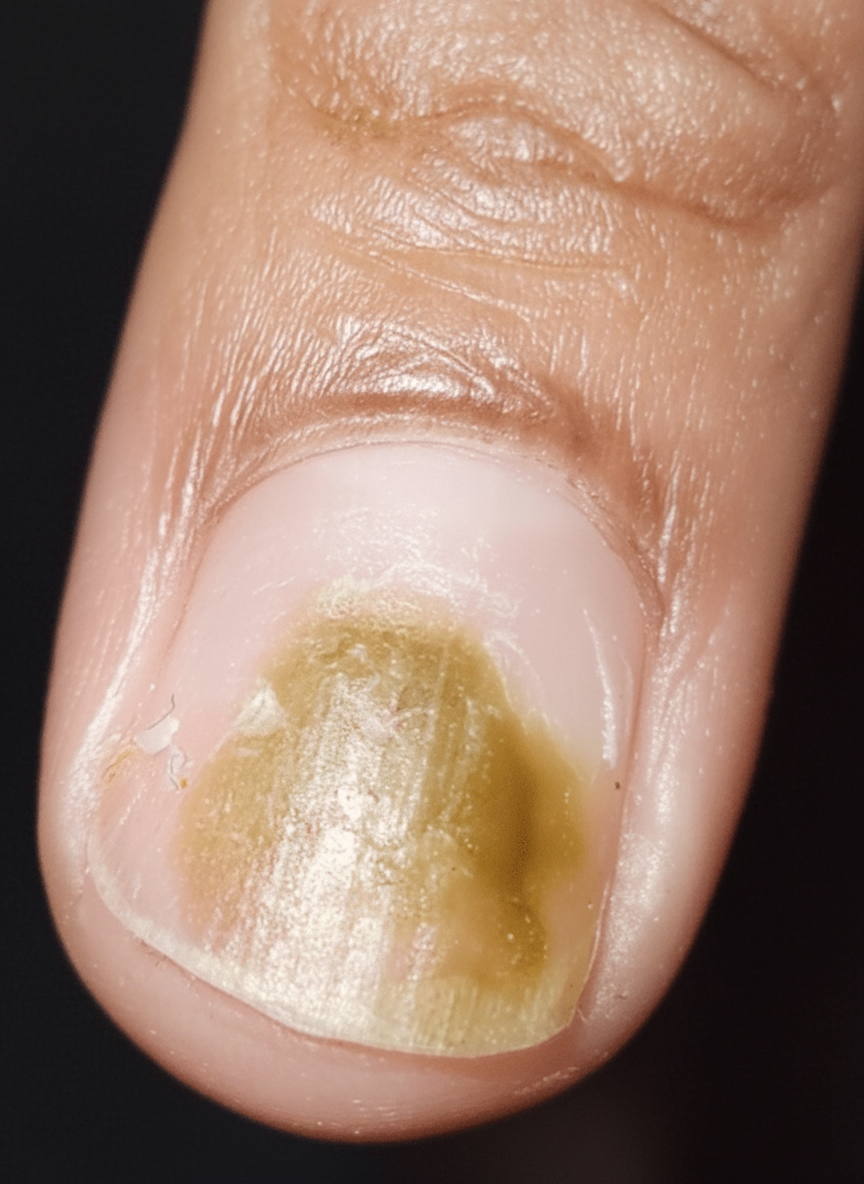
What is the most likely diagnosis in this 50-year-old woman?
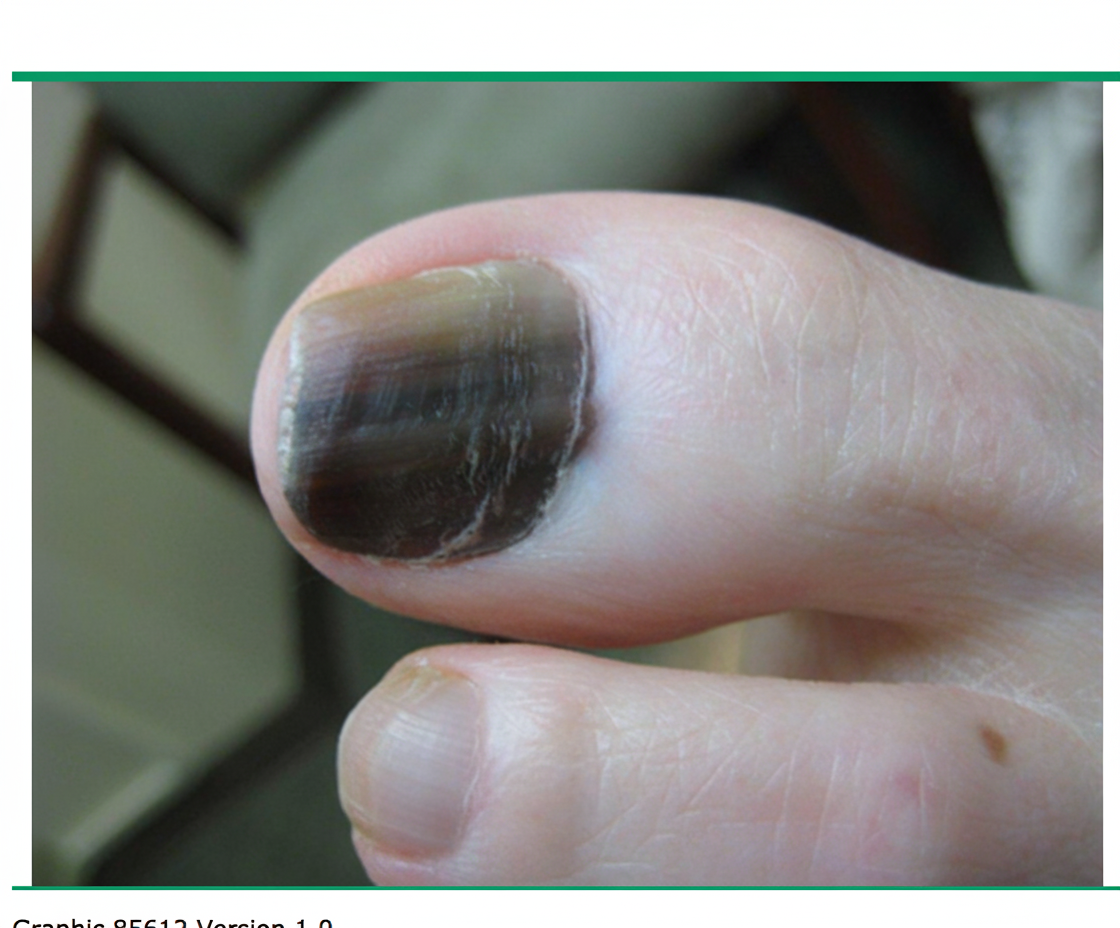
What nutritional deficiency is commonly associated with a chronic alcoholic presenting with a pruritic, eczematous rash on the neck and dorsum of the hands?
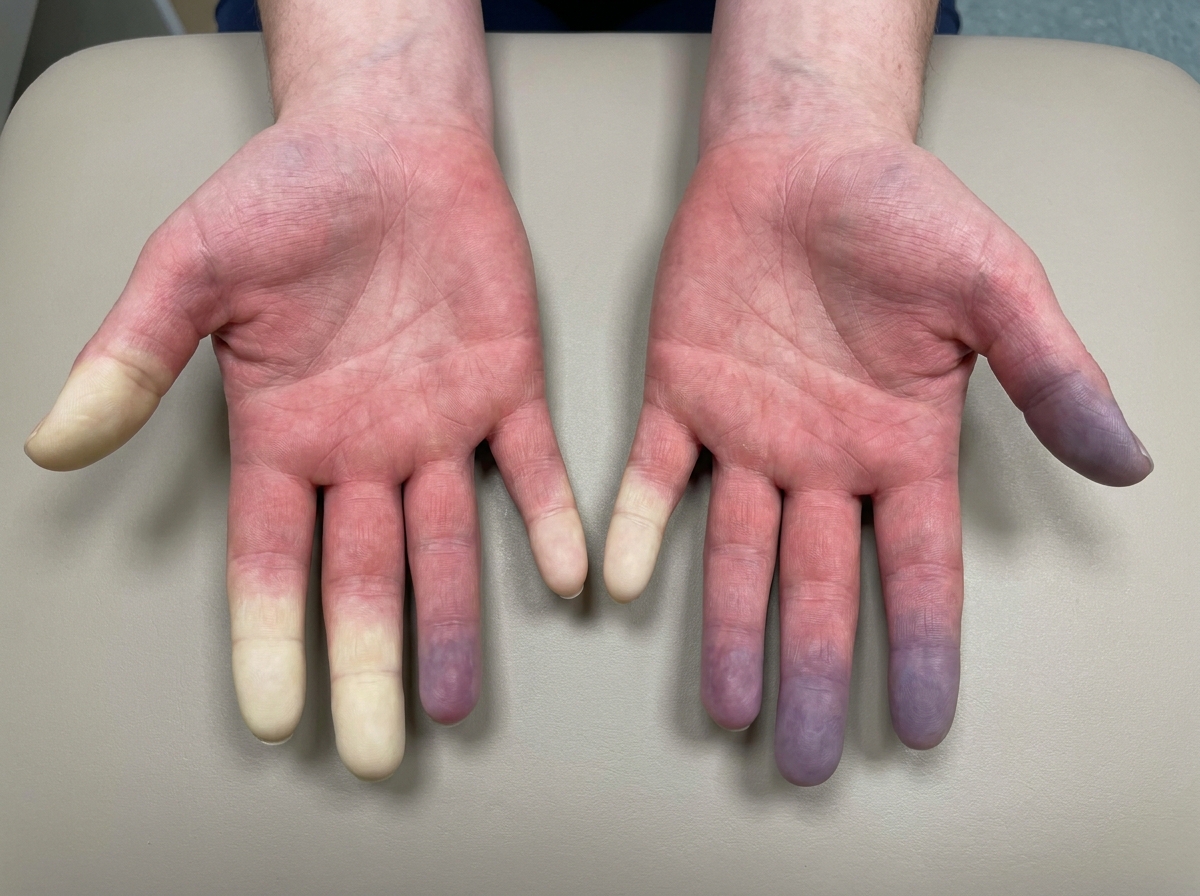
A 17-year-old woman with no comorbidities presents with numbness and paraesthesia of the fingers along with the characteristic finding as shown in the image below. She has no history of smoking or history of other illnesses. She mentions the episodes occur when she is under excess stress or during cold temperatures. What is the most likely diagnosis?
A patient on long-term hydrochlorothiazide therapy presents with features of neuropathy, heart failure, and symmetrical tingling sensations. Which of the following nutrient deficiencies is most likely responsible?
Which is correct about the sign shown?
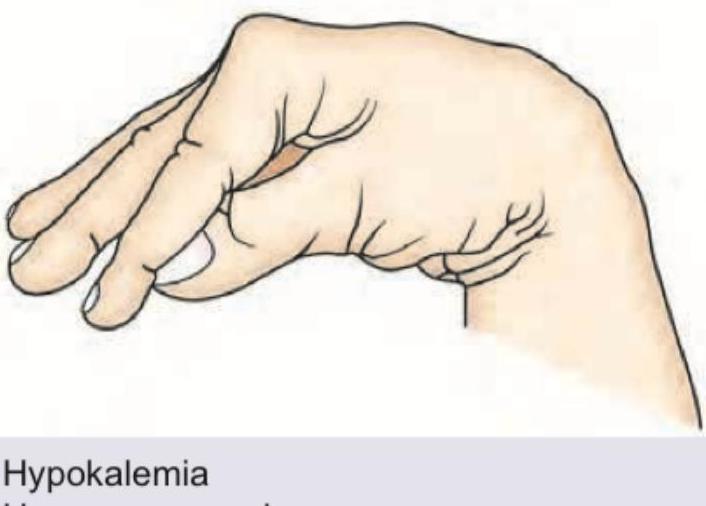
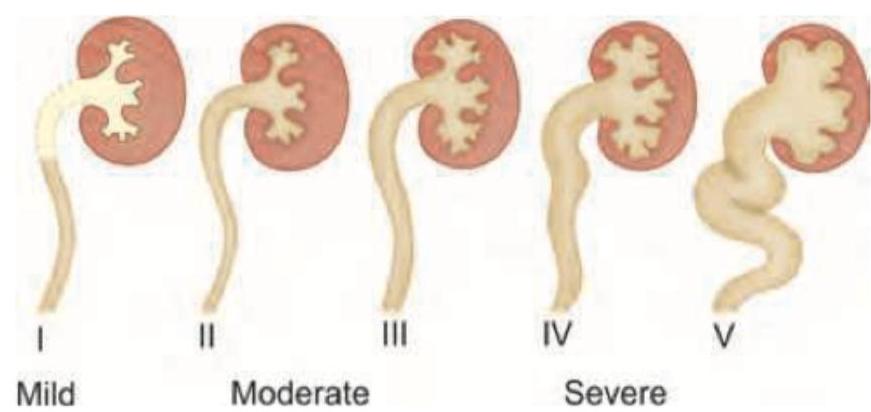
Which of the following will best describe this patient?
A specific clinical sign is characterized by spasm of hand muscles upon inflating a blood pressure cuff. What is this sign called?
Practice by Chapter
Approach to Common Symptoms (Fever, Pain, Fatigue)
Practice Questions
Constitutional Symptoms and Their Differential Diagnosis
Practice Questions
Syncope and Presyncope
Practice Questions
Dizziness and Vertigo
Practice Questions
Dyspnea and Respiratory Distress
Practice Questions
Chest Pain Evaluation
Practice Questions
Abdominal Pain Assessment
Practice Questions
Headache Classification and Management
Practice Questions
Weight Loss and Cachexia
Practice Questions
Edema and Fluid Retention
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
