Clinical Manifestations and Presentation of Diseases — MCQs

On this page
Which of the following is NOT a feature of Superior Vena Cava (SVC) syndrome?
Which ECG finding is characteristic of hypokalemia?
Palmar erythema in liver failure is due to:
Causes of unilateral clubbing include all of the following, EXCEPT?
Postural hypotension is not seen in which of the following conditions?
Which among the following is not a cause for cyanosis?
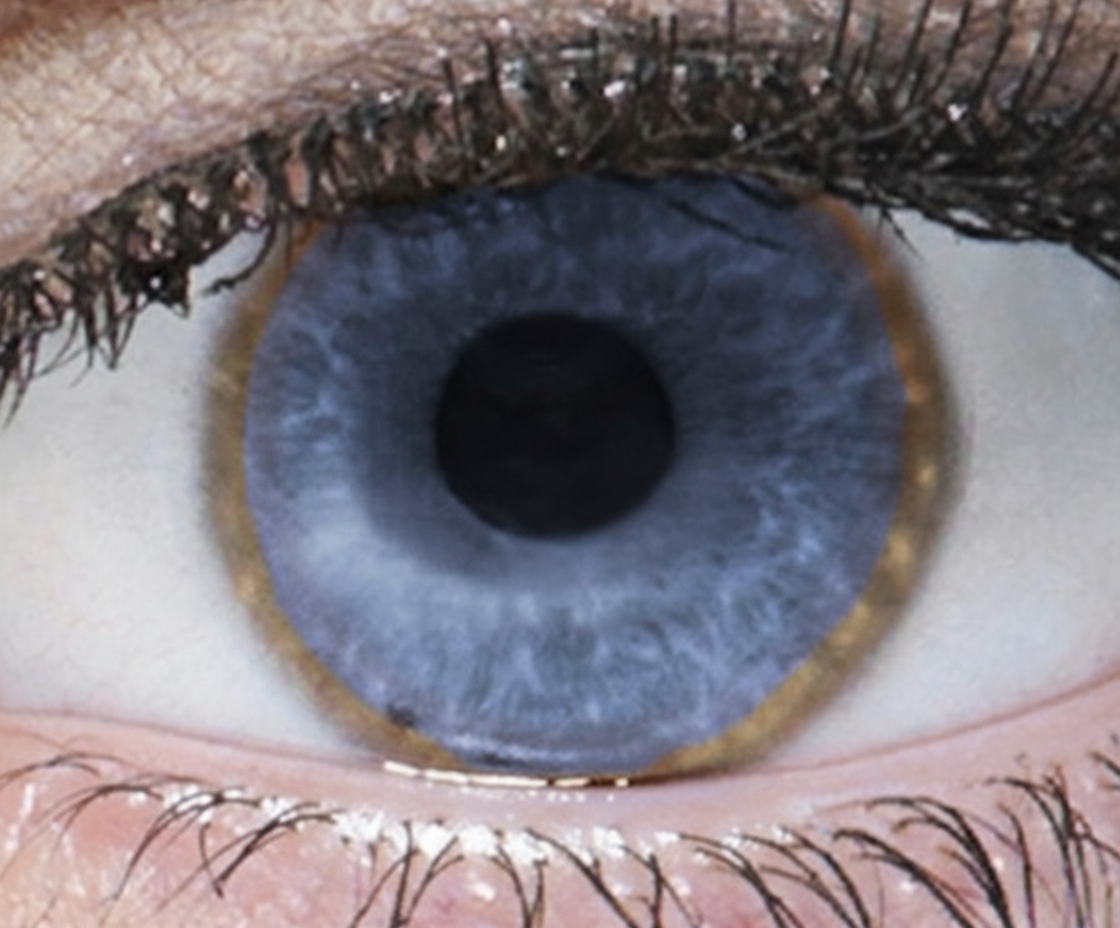
A patient presented with diminished vision and neuropsychiatric manifestations along with hepatic dysfunction. Ocular examination revealed characteristic findings. What is the next investigation to be performed?
All of the following are features of Superior Vena Cava (SVC) Syndrome except?
A 60-year-old male presented to the emergency with breathlessness, facial swelling, and dilated veins on the chest wall. What is the most common cause?
A pigmented lesion is found in the mouth but not on the skin. What is the most likely diagnosis?
Practice by Chapter
Approach to Common Symptoms (Fever, Pain, Fatigue)
Practice Questions
Constitutional Symptoms and Their Differential Diagnosis
Practice Questions
Syncope and Presyncope
Practice Questions
Dizziness and Vertigo
Practice Questions
Dyspnea and Respiratory Distress
Practice Questions
Chest Pain Evaluation
Practice Questions
Abdominal Pain Assessment
Practice Questions
Headache Classification and Management
Practice Questions
Weight Loss and Cachexia
Practice Questions
Edema and Fluid Retention
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
