Clinical Manifestations and Presentation of Diseases — MCQs

On this page
A 45-year-old man presents with hoarseness of voice and difficulty in breathing. Examination reveals a lesion affecting the left recurrent laryngeal nerve. What is the most likely diagnosis?
A 35-year-old male presents with nasal obstruction, rhinorrhea, and sneezing. Examination reveals pale, edematous nasal mucosa. What is the most likely diagnosis?
A 30-year-old woman presents with a painful breast lump that has increased in size over the past two weeks. She also reports fever and malaise. What is the most likely diagnosis?
Which vitamin deficiency is associated with Bitot's spots?
A 24-year-old woman presents with recurrent vulvovaginal candidiasis. Which condition should be considered?
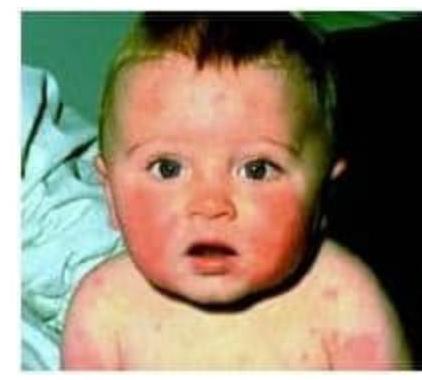
A child with history of fever, photosensitivity, rash sparing nasolabial fold presents to OP. Identify the condition?
Which of the following conditions does not lead to pseudoparalysis?
Cullen's sign is associated with which of the following conditions?
Presence of Velcro crackles at the lung base on auscultation is a sign of which condition?
Which of the following is the most specific risk factor for esophageal cancer in Plummer-Vinson syndrome?
Practice by Chapter
Approach to Common Symptoms (Fever, Pain, Fatigue)
Practice Questions
Constitutional Symptoms and Their Differential Diagnosis
Practice Questions
Syncope and Presyncope
Practice Questions
Dizziness and Vertigo
Practice Questions
Dyspnea and Respiratory Distress
Practice Questions
Chest Pain Evaluation
Practice Questions
Abdominal Pain Assessment
Practice Questions
Headache Classification and Management
Practice Questions
Weight Loss and Cachexia
Practice Questions
Edema and Fluid Retention
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
