Clinical Manifestations and Presentation of Diseases — MCQs

On this page
Smoking is associated with all the following diseases except:
Which one of the following is the investigation of choice in a patient with haematemesis?
The most common complication of pancreas divisum is:
The most common route of spread in a case of pyogenic liver abscess is:
A patient has recurrent abdominal pain and jaundice. The blood investigations reveal reticulocytosis and hyperbilirubinemia. What is the clinical diagnosis?
The capillary refill time is prolonged in all types of shock EXCEPT:
Which of the following statements regarding lymphoedema are correct? 1. Patients experience constant dull ache and even severe pain sometimes 2. Manual lymphatic drainage has a role 3. Primary lymphoedema is caused by congenital lymphatic dysplasia 4. Nonne Milroy's disease is a type of primary lymphoedema Select the correct answer using the code given below:
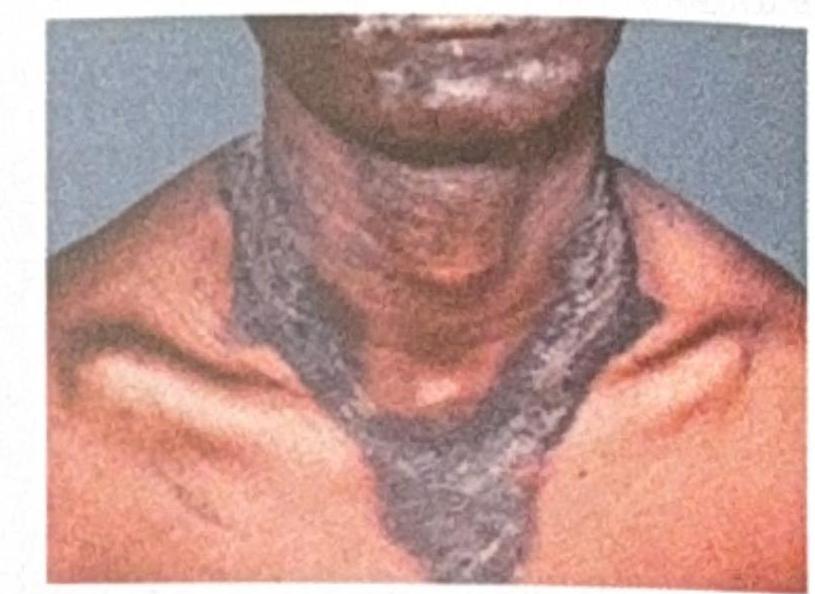
A 45-year-old man presents with the following skin changes (as shown in the image). What relevant history should be taken to diagnose this condition?
Frontal headache is due to inflammation of which sinus?
Gynecomastia is seen in all except;
Practice by Chapter
Approach to Common Symptoms (Fever, Pain, Fatigue)
Practice Questions
Constitutional Symptoms and Their Differential Diagnosis
Practice Questions
Syncope and Presyncope
Practice Questions
Dizziness and Vertigo
Practice Questions
Dyspnea and Respiratory Distress
Practice Questions
Chest Pain Evaluation
Practice Questions
Abdominal Pain Assessment
Practice Questions
Headache Classification and Management
Practice Questions
Weight Loss and Cachexia
Practice Questions
Edema and Fluid Retention
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
