Clinical Manifestations and Presentation of Diseases — MCQs

On this page
What is the Lovibond angle?
Which of the following statements is true regarding digital clubbing?
Which of the following statements about weight loss is TRUE or FALSE?
Which of the following statements regarding dyspnoea are True or False?
Pitting edema indicates an excess of what volume of fluid in tissue spaces?
Obesity predisposes to all the following conditions except:
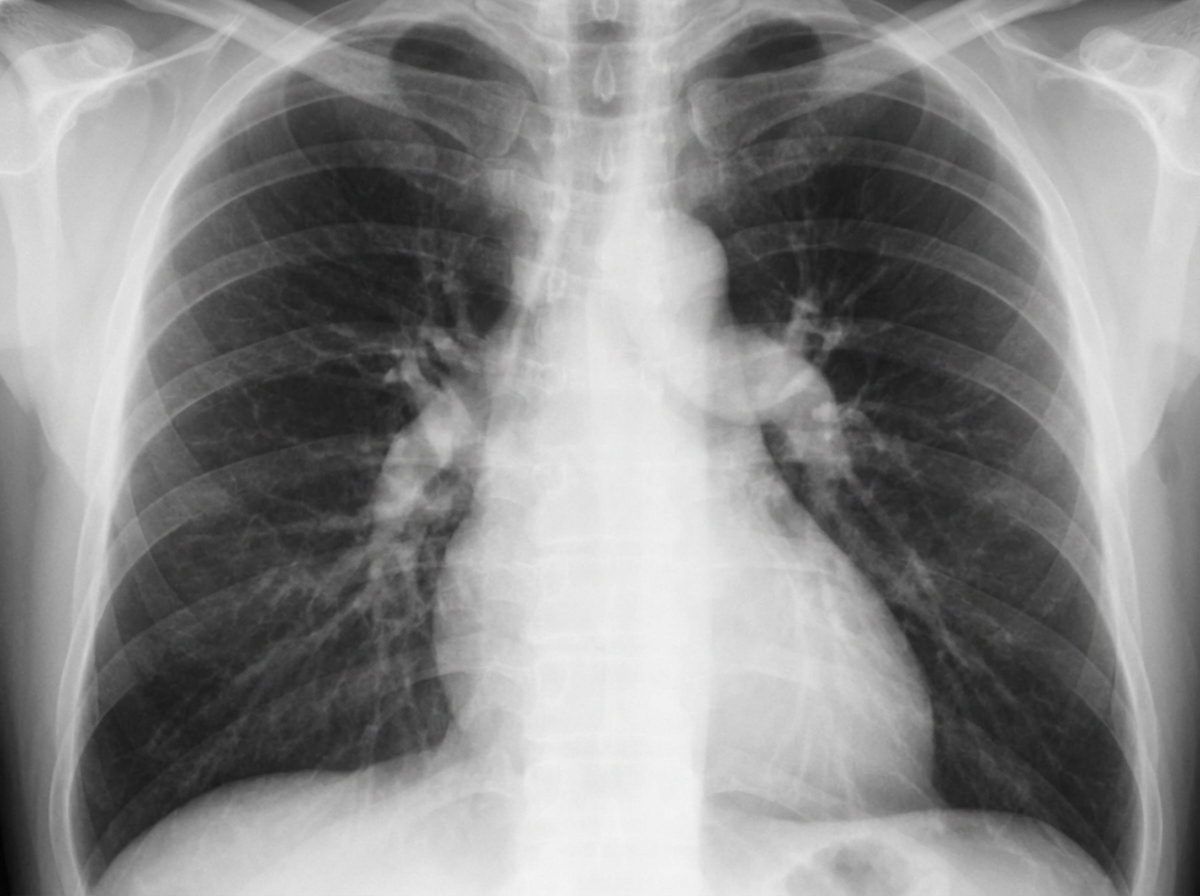
A 24-year-old female graduate student reports increasing shortness of breath with exercise and has recently noticed dyspnea on mild activity. One day before presenting at the office, she experienced sudden loss of consciousness while shopping at a grocery store. On physical examination, vital signs are: pulse 88 bpm; temperature 97.8degF; respirations 18/min; blood pressure 100/70 mm Hg. BMI is 34. ABGs on RA: pH 7.43; PCO2 36 mm Hg; PO2 87 mm Hg. Chest x-rays are shown. What clinical and chest radiographic diagnosis may be commonly associated with this presentation?
Clubbing of the fingers is seen in all of the following conditions except:
Dependent edema is a clinical sign commonly associated with which of the following conditions?
What is the definition of sustained fever?
Practice by Chapter
Approach to Common Symptoms (Fever, Pain, Fatigue)
Practice Questions
Constitutional Symptoms and Their Differential Diagnosis
Practice Questions
Syncope and Presyncope
Practice Questions
Dizziness and Vertigo
Practice Questions
Dyspnea and Respiratory Distress
Practice Questions
Chest Pain Evaluation
Practice Questions
Abdominal Pain Assessment
Practice Questions
Headache Classification and Management
Practice Questions
Weight Loss and Cachexia
Practice Questions
Edema and Fluid Retention
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
