Cardiology — MCQs

On this page
Which of the following is not a major Framingham criterion for heart failure?
Pulsus paradoxus is present in all of the following conditions except:
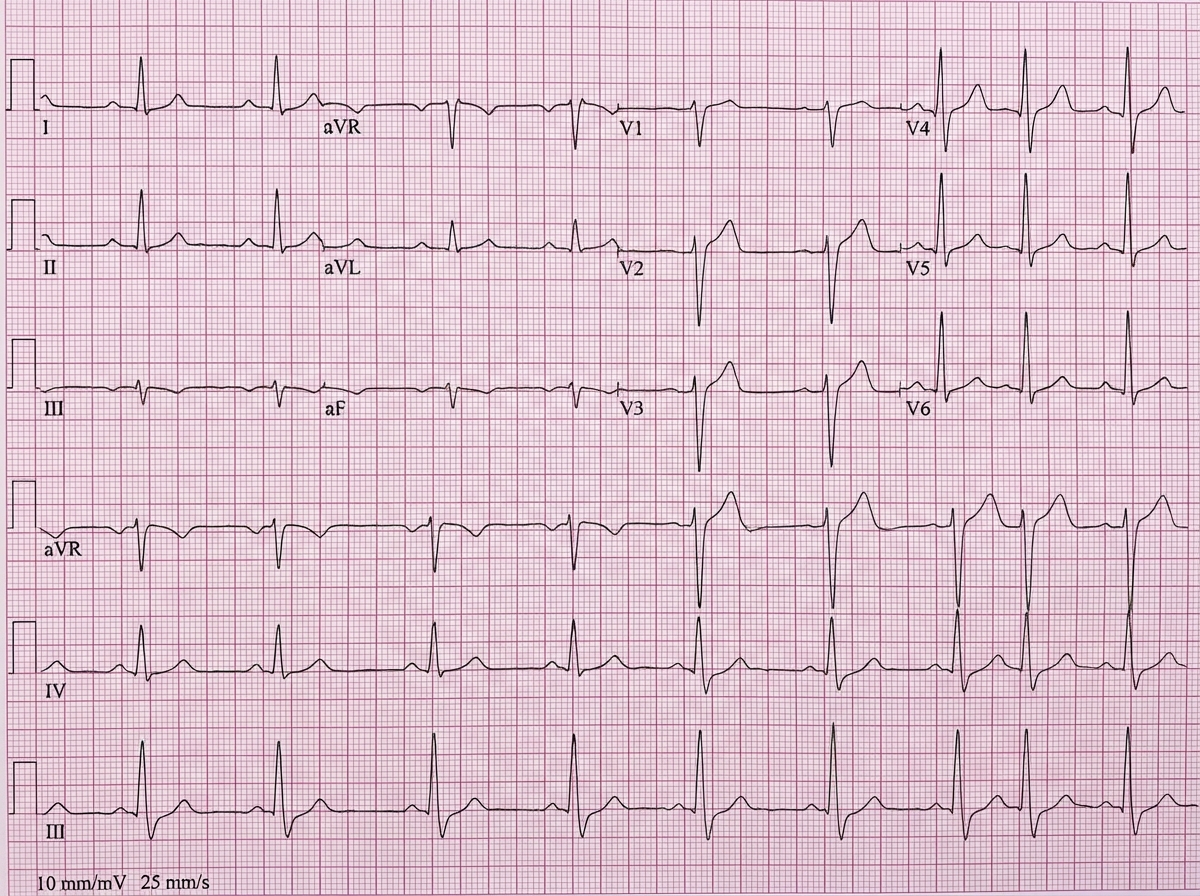
A 70-year-old man with a past medical history of ischemic heart disease and hypertension presents to his GP with recurrent episodes of syncope over the past 2 weeks. Based upon this ECG, which of the following clinical findings is most likely to be present?
Atrial fibrillation may occur in all of the following conditions, except?
A patient with acute inferior wall myocardial infarction has developed shock. Which of the following is the most likely cause of shock?
Which of the following produces a continuous murmur except?
Pulsus paradoxus is seen in all of the following EXCEPT:
A 55-year-old woman presents with complaints of chest pain. She states that the chest pain predictably occurs when she climbs four flights of stairs to reach her apartment or when she has been jogging for more than 10 minutes. She is particularly concerned because her mother died of a myocardial infarction at 50 years of age. Which of the following best describes this patient's state?
A 65-year-old man with a history of syncopal attacks on exertion and angina is undergoing heart valve surgery. Which kind of pulse is expected to be present before surgery?
Ewa's sign is seen in:
Practice by Chapter
Coronary Artery Disease and Angina
Practice Questions
Acute Coronary Syndromes
Practice Questions
Heart Failure
Practice Questions
Cardiac Arrhythmias
Practice Questions
Valvular Heart Diseases
Practice Questions
Cardiomyopathies
Practice Questions
Pericardial Diseases
Practice Questions
Congenital Heart Disease in Adults
Practice Questions
Hypertension and Hypertensive Emergencies
Practice Questions
Pulmonary Hypertension
Practice Questions
Non-invasive Cardiac Diagnostics
Practice Questions
Preventive Cardiology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
