Cardiology — MCQs

On this page
Duroziez sign is seen in which of the following conditions?
A patient develops sudden palpitation with HR 150/min, regular. What could be the cause?
What is the most appropriate intervention for acute myocardial infarction?
What are the absolute contraindications for fibrinolytic therapy?
What is the abnormality shown in the ECG?
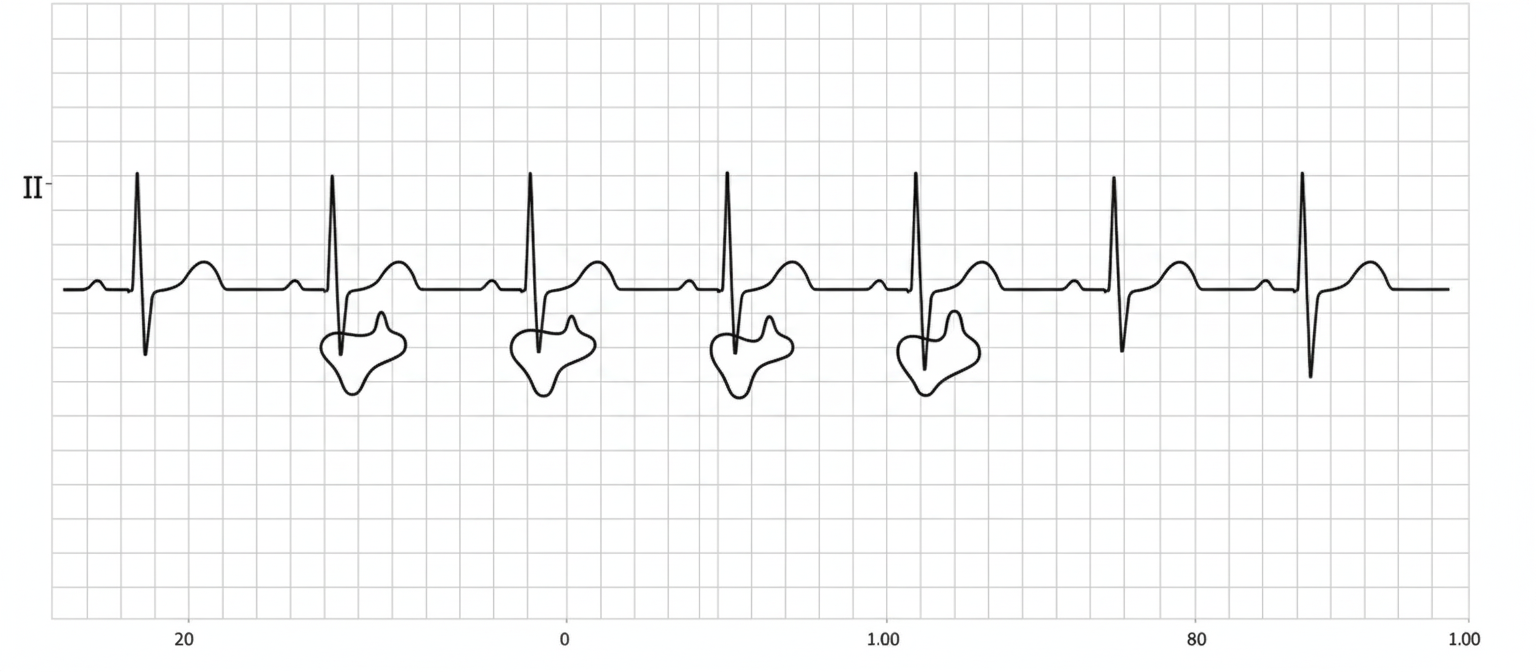
Pulsus bisferiens is best felt in which artery?
Which of the following arrhythmias is most frequent in Holiday Heart Syndrome?
Which of the following is the best predictor of cardiovascular risk?
A 73-year-old man has angina pectoris on exertion, but an angiogram reveals noncritical stenosis of the coronary arteries. This clinical presentation is most frequently associated with which of the following valvular heart diseases?
A patient with acute inferior wall myocardial infarction has developed shock. Which of the following is the most likely cause of shock?
Practice by Chapter
Coronary Artery Disease and Angina
Practice Questions
Acute Coronary Syndromes
Practice Questions
Heart Failure
Practice Questions
Cardiac Arrhythmias
Practice Questions
Valvular Heart Diseases
Practice Questions
Cardiomyopathies
Practice Questions
Pericardial Diseases
Practice Questions
Congenital Heart Disease in Adults
Practice Questions
Hypertension and Hypertensive Emergencies
Practice Questions
Pulmonary Hypertension
Practice Questions
Non-invasive Cardiac Diagnostics
Practice Questions
Preventive Cardiology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
