Cardiology — MCQs

On this page
Reversible myocardial stunning with ECG changes of acute myocardial infarction is seen in which of the following conditions?
ECG changes in atrial fibrillation do not include which of the following?
A 35-year-old lady presents with a skin lesion and repeated episodes of syncope on sudden change of position. What does the ECG show?
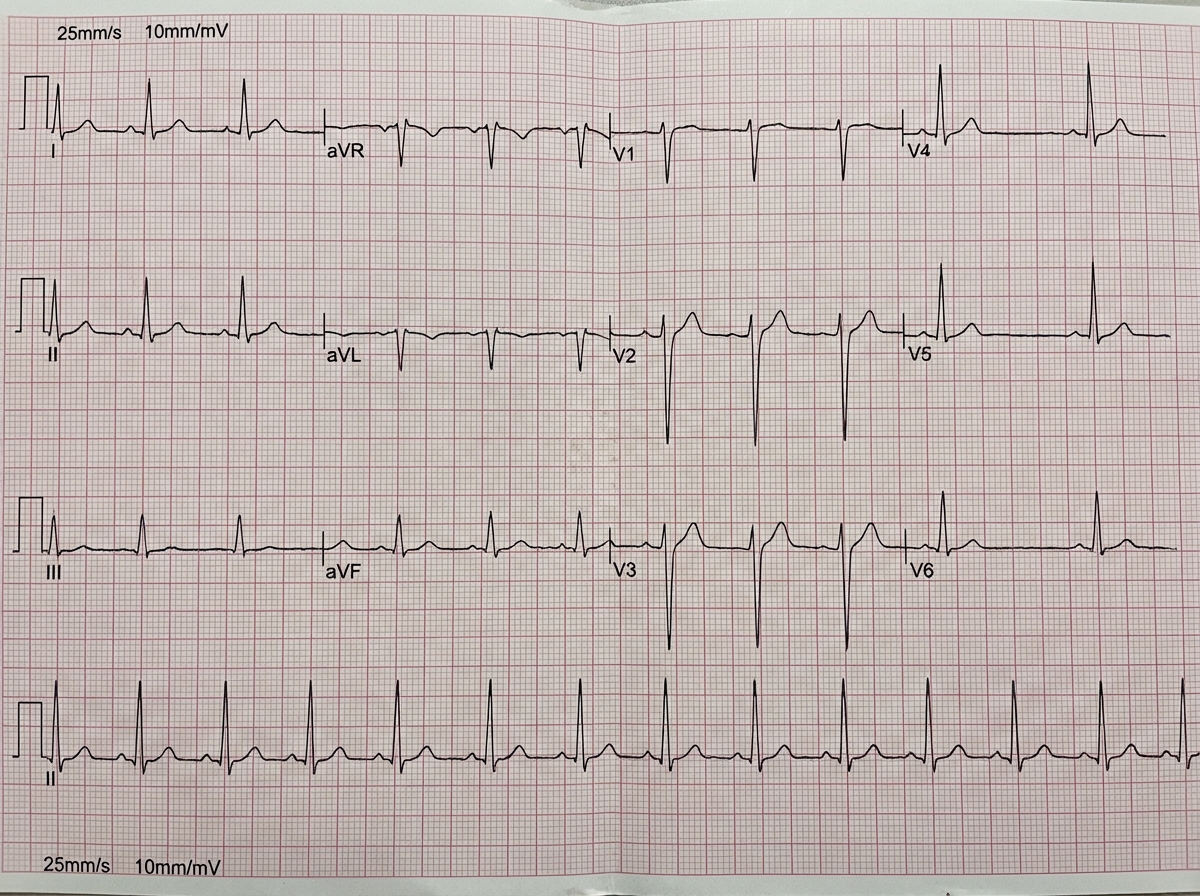
What is the most common valvular lesion in carcinoid syndrome?
A 72-year-old man has had poorly controlled hypertension for the past 20 years. Over the past day he has had a severe headache with nausea, followed by confusion, then convulsions. On examination he is afebrile, but his blood pressure is now 260/150 mm Hg. There is bilateral papilledema. Which of the following pathologic lesions is most likely to have developed in his brain during the past day?
A 60-year-old man presents with dizziness, nausea, and shortness of breath of several months' duration. Physical examination shows hepatomegaly, ascites, and anasarca. His blood pressure is 200/115 mm Hg. A chest X-ray demonstrates cardiomegaly and mild pulmonary edema. Although different mechanisms may have contributed to the pathogenesis of hypertension in this patient, what is the common end result for all of them?
All are features of the given ECG except:
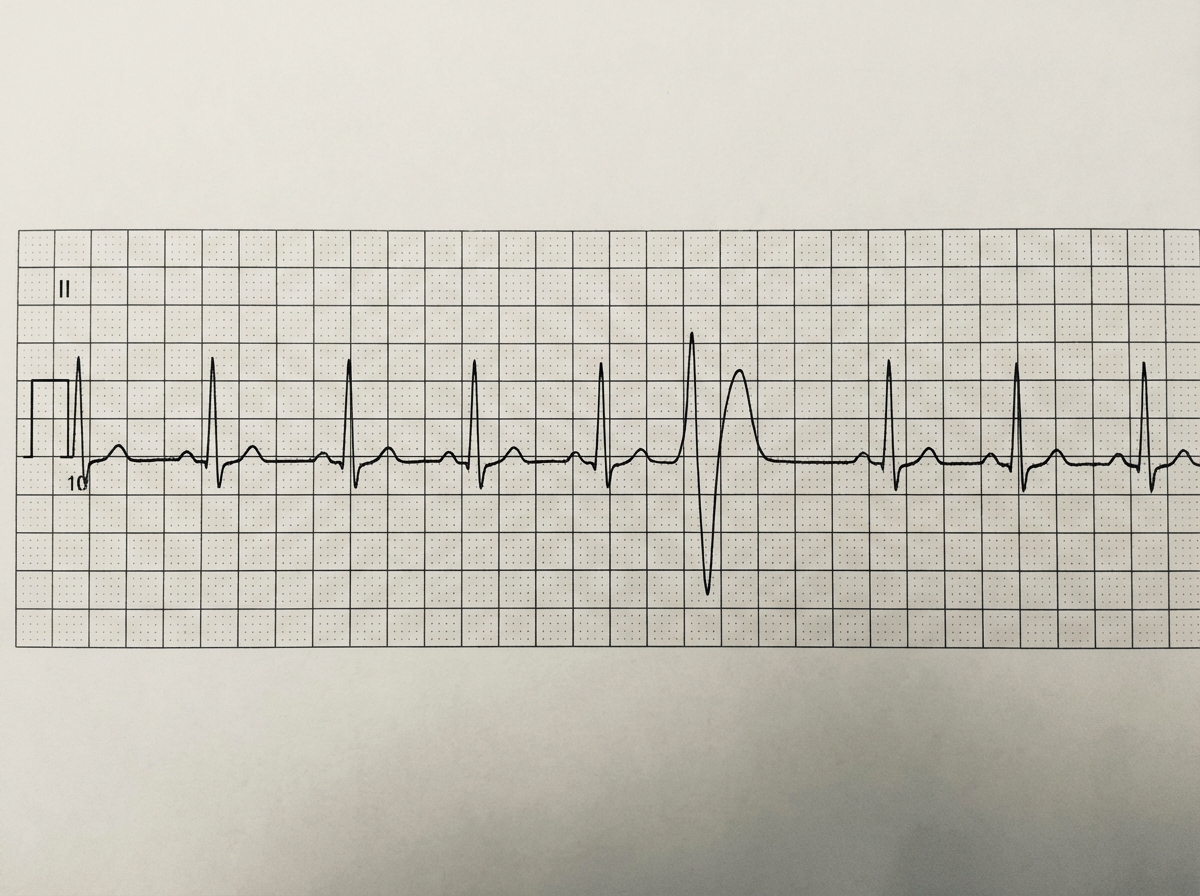
Which of the following is NOT a feature of atrial septal defect?
A 55-year-old man presents with gradually increasing shortness of breath and leg swelling over the past month. He has orthopnea and paroxysmal nocturnal dyspnea. His medical history includes hypercholesterolemia treated with simvastatin and hypertension treated with hydrochlorothiazide. Current blood pressure is 140/90 mm Hg. Physical examination reveals mild jugular venous distension, bibasilar crackles, an S3 gallop, and minimal pedal edema. Echocardiography shows a left ventricular ejection fraction (LVEF) of 40% without segmental wall-motion abnormality. The patient wishes to minimize his medication regimen. What change in his management would you recommend?
Intermittent claudication is characterized by which of the following?
Practice by Chapter
Coronary Artery Disease and Angina
Practice Questions
Acute Coronary Syndromes
Practice Questions
Heart Failure
Practice Questions
Cardiac Arrhythmias
Practice Questions
Valvular Heart Diseases
Practice Questions
Cardiomyopathies
Practice Questions
Pericardial Diseases
Practice Questions
Congenital Heart Disease in Adults
Practice Questions
Hypertension and Hypertensive Emergencies
Practice Questions
Pulmonary Hypertension
Practice Questions
Non-invasive Cardiac Diagnostics
Practice Questions
Preventive Cardiology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
