Cardiology — MCQs

On this page
According to the New York Heart Association (NYHA) functional classification, patients with marked limitation to physical activity belong to which grade?
What is the metabolic defect in accelerated hypertension?
What is a typical finding in cardiac tamponade?
A 72-year-old male presented to the ER with falls. Based on the provided ECG interpretation, what is the likely diagnosis?
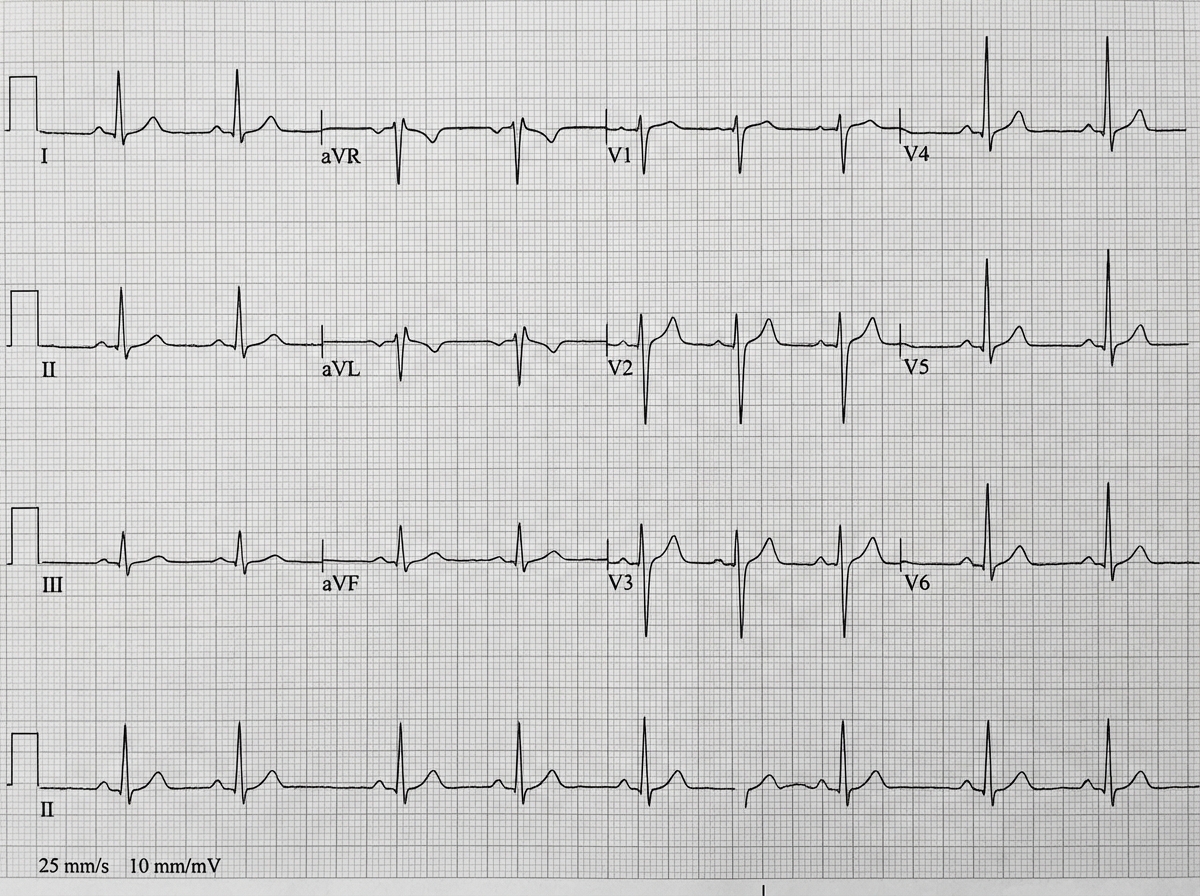
What is the characteristic cardiac anomaly associated with Lutembacher syndrome?
Which of the following is true about sinus tachycardia?
Pulsus paradoxus is seen in which of the following conditions?
Which of the following is seen in torsades de pointes?
A 20-year-old female patient presents with non-exertional chest pain. On auscultation, she has multiple non-ejection clicks. What is the investigation of choice?
Which of the following is NOT true regarding Wolff-Parkinson-White (WPW) syndrome?
Practice by Chapter
Coronary Artery Disease and Angina
Practice Questions
Acute Coronary Syndromes
Practice Questions
Heart Failure
Practice Questions
Cardiac Arrhythmias
Practice Questions
Valvular Heart Diseases
Practice Questions
Cardiomyopathies
Practice Questions
Pericardial Diseases
Practice Questions
Congenital Heart Disease in Adults
Practice Questions
Hypertension and Hypertensive Emergencies
Practice Questions
Pulmonary Hypertension
Practice Questions
Non-invasive Cardiac Diagnostics
Practice Questions
Preventive Cardiology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
