Cardiology — MCQs

On this page
All the following are major criteria for the diagnosis of rheumatic fever except?
A 41-year-old woman presents with chest pain, shortness of breath, and worsening fatigue for the past day. The chest pain initially worsened with lying down and improved with leaning forward, but now it seems equal in intensity over all positions. On examination, she has labored, fast breathing and appears to be in pain. She has jugular venous distention. She is tachycardic, and has distant heart sounds with a friction rub. Her lungs are clear to auscultation bilaterally, and she has no limb edema. Her pulse is 126/min, BP is 89/66 mm Hg, respiratory rate is 32/min, and oxygen saturation is 98% on room air. Which of the following is the most likely diagnosis?
Which of the following statements regarding the ECG findings in acute pericarditis is FALSE?
What does the ECG show?
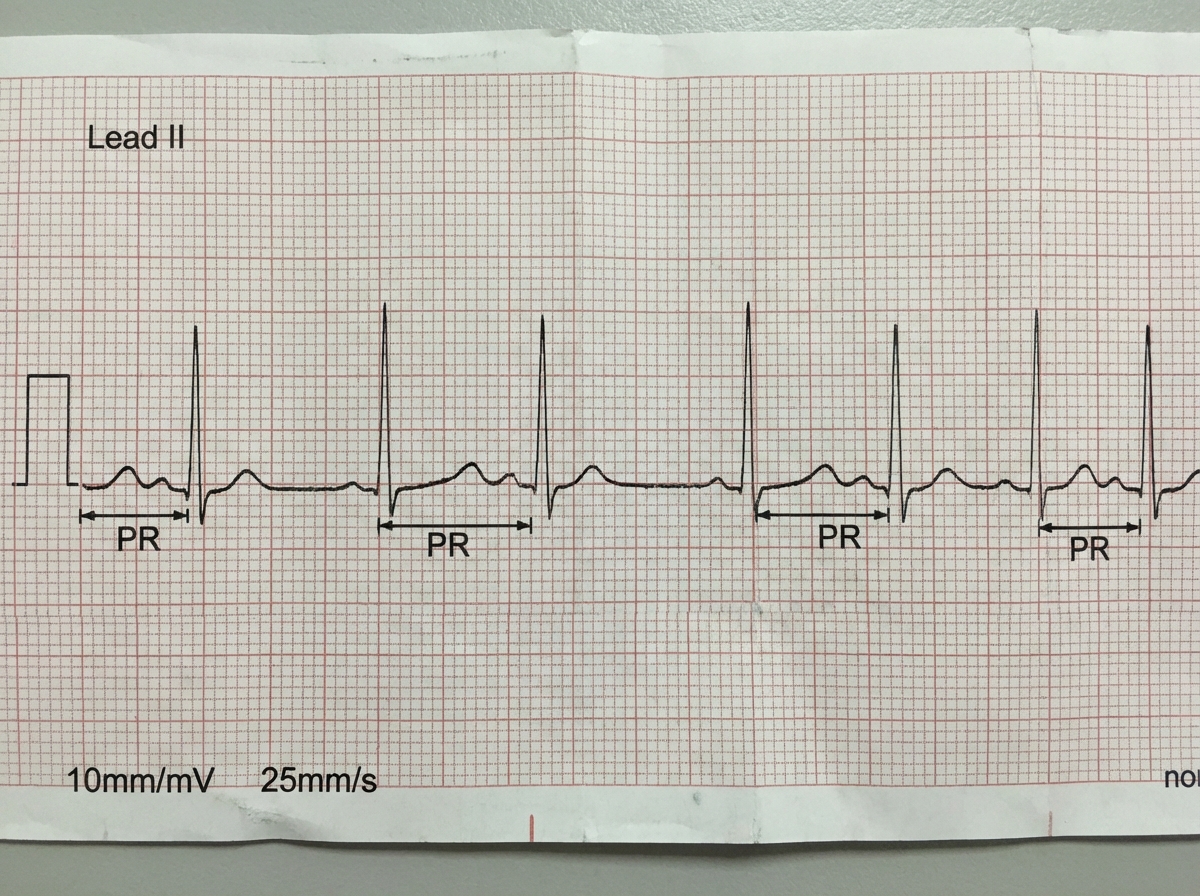
What type of mutation is most commonly associated with Brugada syndrome?
Elevated JVP is seen in all except?
Pulse deficit may be seen in all of the following, except:
A dicrotic pulse is observed in which condition?
Which of the following conditions is also known as pulseless disease?
Which is not a feature of chronic mitral regurgitation?
Practice by Chapter
Coronary Artery Disease and Angina
Practice Questions
Acute Coronary Syndromes
Practice Questions
Heart Failure
Practice Questions
Cardiac Arrhythmias
Practice Questions
Valvular Heart Diseases
Practice Questions
Cardiomyopathies
Practice Questions
Pericardial Diseases
Practice Questions
Congenital Heart Disease in Adults
Practice Questions
Hypertension and Hypertensive Emergencies
Practice Questions
Pulmonary Hypertension
Practice Questions
Non-invasive Cardiac Diagnostics
Practice Questions
Preventive Cardiology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
