Cardiology — MCQs

On this page
Which of the following is untrue regarding sick sinus syndrome?
What causes Wolff-Parkinson-White syndrome?
Regarding Hypertrophic Obstructive Cardiomyopathy (HOCM), all are true except?
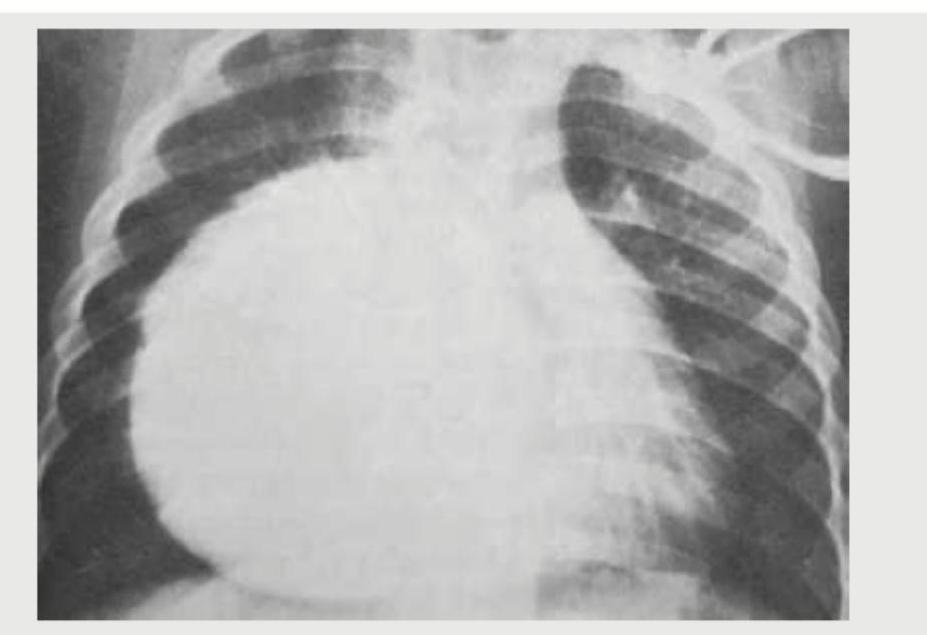
A 60-year-old smoker presents with breathlessness for 2 weeks. On examination, heart rate is 100/min, BP = 90/60 mm Hg, and neck veins are distended with a palpable liver. CXR is shown. What is the probable diagnosis?
What is the critical degree of narrowing of coronary vessels that causes angina?
Aggravation of symptoms of angina in a patient when given nitrates is seen in which of the following conditions?
A 49-year-old man has his serum lipids measured. Which pattern suggests the lowest risk for coronary artery disease?
A Carey coomb murmur is heard in which of the following conditions?
What is not true about infective endocarditis?
What is true regarding cardiomyopathy?
Practice by Chapter
Coronary Artery Disease and Angina
Practice Questions
Acute Coronary Syndromes
Practice Questions
Heart Failure
Practice Questions
Cardiac Arrhythmias
Practice Questions
Valvular Heart Diseases
Practice Questions
Cardiomyopathies
Practice Questions
Pericardial Diseases
Practice Questions
Congenital Heart Disease in Adults
Practice Questions
Hypertension and Hypertensive Emergencies
Practice Questions
Pulmonary Hypertension
Practice Questions
Non-invasive Cardiac Diagnostics
Practice Questions
Preventive Cardiology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
