Cardiology — MCQs

On this page
Which of the following statements regarding torsades de pointes is FALSE?
Osler's nodes are seen at:
A continuous murmur is heard in all of the following conditions except?
Which of the following statements about Osler's nodes is FALSE?
Non-ejection clicks are heard in which of the following conditions?
Changing character of a murmur in a patient with joint pain and embolic phenomenon indicates which of the following diagnoses?
Women with myocardial infarction are more likely to present with which of the following complications than males?
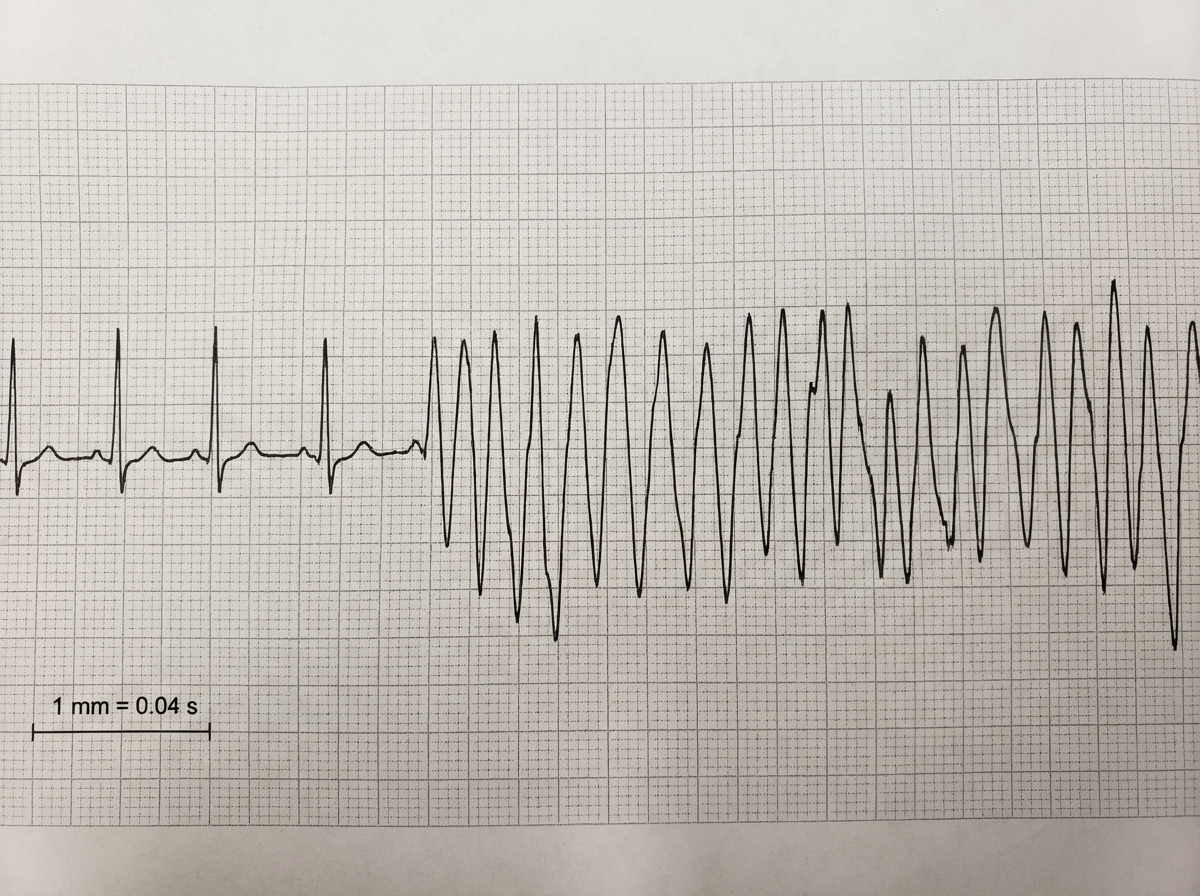
All the following statements are true regarding the given ECG except?
A 45-year-old man experiences crushing substernal chest pain after arriving at work one morning. Over the next 4 hours, the pain persists and begins to radiate to his left arm. He becomes diaphoretic and short of breath but waits until the end of his 8-hour shift to go to the hospital. An elevated serum value of which of the following laboratory tests would be most useful for the diagnosis of this patient on admission to the hospital?
Which of the following is NOT true regarding Mitral valve prolapse syndrome?
Practice by Chapter
Coronary Artery Disease and Angina
Practice Questions
Acute Coronary Syndromes
Practice Questions
Heart Failure
Practice Questions
Cardiac Arrhythmias
Practice Questions
Valvular Heart Diseases
Practice Questions
Cardiomyopathies
Practice Questions
Pericardial Diseases
Practice Questions
Congenital Heart Disease in Adults
Practice Questions
Hypertension and Hypertensive Emergencies
Practice Questions
Pulmonary Hypertension
Practice Questions
Non-invasive Cardiac Diagnostics
Practice Questions
Preventive Cardiology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
